As part of a collaborative effort with Rad-Aid International and the University of Nairobi, interventional Radiology faculty volunteers have been working for several years to help establish the first interventional radiology fellowship program in Kenya. These faculty members visit the site at Kenyatta National Hospital to supplement the education of the interventional radiology physician trainees through lectures and hands-on teaching. Dr. Stewart has served as a faculty member for this program for 4 years, and last visited the site in spring 2021, the first trip by an adjunct faculty member since the pandemic began. For this trip, along with Dr. Kesselman from Stanford, Dr. Stewart plans to lead a group including an interventional radiology residents from UCLA and Stanford, a nurse practitioner (me) experienced in managing patients admitted to interventional radiology, and a medical student working on several collaborative research projects with the Kenyan interventional radiologists. This experienced team will continue our educational efforts and help to optimize patient care from multiple perspectives for the entire interventional radiology team at Kenyatta National Hospital. The team will work with their colleagues there for 2 weeks in February 2023.
The population of Nairobi and surrounding areas benefit greatly from increasing the capacity of Kenyatta National Hospital, the country's major referral hospital, to provide minimally invasive image guided therapies. These treatments are especially helpful in a resource limited region where access to surgical care and recovery support is difficult. This program seeks to educate future interventional radiologists and support the entire IR program to increase the quality and quantity of IR services that can be offered to this patient population.
Our team will help provide training to the interventional radiology fellows, radiology residents, and interventional radiology nurses and technologists at Kenyatta National Hospital as part of a longitudinal relationship between colleagues in the United States and in Nairobi. This relationship has been built over the past several years and this visit helps to continue this through in-person collaboration and hands on teaching, helping it continue to flourish. Specifically, this collaboration has helped lead to the initiation of the first interventional radiology fellowship program in Kenya, helping to keep talented physicians in the region to provide specialized services in this underserved area. This educational outreach program helps ensure that their education is robust and continues to develop outstanding interventional radiologists to serve the people of Kenya.













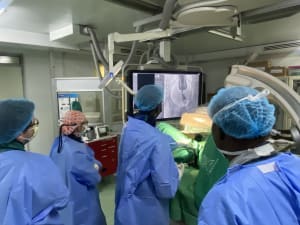
TRIP REPORT
Trip objectives: met
As a nurse practitioner, my objective was to learn the patient workflow of the IR department. I spent my week shadowing both the nurses and the doctors.
The Kenyatta National Hospital is the oldest hospital in Kenya. It is a public, tertiary, referral hospital for the Ministry of Health. It is also the teaching hospital of the University of Nairobi College of Health Sciences. It is the oldest and 2nd largest hospital in the country and East Africa as well. The radiology department is comprised of a CT scanner, an MRI scanner, an angio suite (which is currently broken) and are using a C-arm instead, and 2 ultrasound areas. The entire radiology department is run by a team of 4-5 nurses. They have 9 radiology trained nurses but a few are currently out on leave. Virginia is the Unit Director. In IR, they have one nurse assigned to check the patients in and 2 nurses circulates in the procedure, one in US and one in fluoro. A nurse is also assigned to MRI.
The nurse checks the patient in and takes them back to get changed. Almost all procedures are local anesthetic only, except for their sick inpatients or pediatric cases, which require anesthesia. The nurses are not trained to give sedation.
The majority of patients are referred to IR as outpatients from other services. They are referred for various procedures, but the most common procedures are biopsies and drains.
Wednesday is IR clinic. I shadowed Muhammad, one of the second year IR fellows from Mombasa. Patients essentially show up at random, it is a first come, first serve arrangement. There are no appointment times. Patients check-in at the front desk and the admin people pull their paper chart. Patients can show up at 730am and not get seen til 1pm. Clinic is very busy, they see up to 40 patients every Wednesday. The Attendings (called Consultants) and fellows individually see patients. They will see all the patients who show up. Nobody will be turned away without being seen.
Patients show up to clinic with a referral paper that states were referred for. When the patient comes to the consultation room they often have copies of their US, CT (not on a disc but slices on film). The doctor reviews the paper chart, looking at labs, reading recent history, and looks at images to decide the plan of care. The doctor fills out forms for the patient (surgical service pre-authorization form & radiological report form) that the patient will take to the NHIF desk (National Health Insurance Fund) - to have the procedure approved. The patient will receive a text that the procedure is improved usually within a few days. The doctor also gives the patients a paper to give to the lab. For the most part they only check Hgb/plt prior to the procedure. About 70% of people have insurance, 30% do not. I am told insurance cost about $10 per month. The median income for a person in Nairobi is $600/month. The doctor also writes a short consult note in the paper chart. The patient is advised to come back to IR clinic the following Wednesday with proof of procedural approval and lab work. Then the procedure is scheduled for following week, or sooner if urgent. The paper chart goes back to medical records after the consultation. Consultation costs 1,100 shillings or $9 dollars for the consult There are no nurses involved in IR clinic day.
On all other days, IR clinic starts at 730-8am. Patients check in at the HI (health information desk) where they either show their invoice for their procedure/study that states the procedure is covered by insurance, or if they have no insurance, they pay for the procedure. The department does not perform studies or procedures without ensuring payment was posted. Then patients are taken back to a waiting area where they wait. It doesn’t appear that the patients have appointment times, they are told to show up on a particular day. Patients bring their health information with them, such as X-rays or lab results. Patients know their histories. The department keeps a calendar with the patients names along with the procedures they need. Each day they have roughly 10-12 patients scheduled. They also add-on inpatient cases.
I observed the in-take process. The nurses asks them how they are feeling. Takes vitals. Checks if the have paid for the procedure via receipt if they are paying cash or for an invoice if they are paying by public insurance. Most patients have public insurance. Patients do not have scheduled appointment times, rather they show up in the morning and it’s a first come first served arrangement. Once they are checked in they wait in the cue outside the department. Patients here are very patient. The patients will put a gown on before the procedure. The nurse will set up the sterile table and grab supplies. The technologist will be running the C-arm or CT scanner. The doctors will prep the site. The circulating nurse will assist the doctor during the procedure and grab whatever they request. The few procedures I observed they did not do a time-out. They are not given any prophylactic antibiotics. After the procedure, the patient is given instructions by the nurses. They are asked to return to the clinic in a few weeks for a follow up. It is unclear how many patients return for follow-up.
Inpatient process is similar, a senior resident comes down to the IR department with the consultation request. They usually bring the patients chart. IR MD reviews consult. If they agree with the procedure, then they write NHIF paperwork. Either the porter from the ward or family member brings the paperwork to be processed with NHIF. The patient or family member will receive a text message with approval, then the IR team will be consulted, then they will be added to the schedule.
My objective for the trip was to learn the patient workflow. In collaboration with Virginia, the nurse manager, one of the nurses, Joshua, and one of the IR fellows, Dr Mohammed Bashaeb, I will create patient education form for the most popular procedures that the hospital will translate into Swahili. It is my hopes that these education forms will improve patient understanding of their procedure, device, and provide the nurses and doctors with a form they can refer to when educating patients.
I should mention the hospital is in the process of switching from paper charting to electronic charting.
Some interesting take aways from my hospital tour. I toured the renal unit, which is a mix of inpatients and outpatients. People pay for every single dialysis treatment. Patients at Kenyatta get HD two days a week because they can’t afford three days a week. Most patients are catheter dependent. Only a few patients have fistulas, mostly because they cannot afford a fistula. Probably only half of the dialysis machines are funtctioning. The broken machines are crowded into the corner. Dialysis lines are placed by the nephrologists, not IR. I toured the main ICU, which is a mixed pediatric and adult ICU, 22 patients, 11 per side, open unit without curtains or walls to separate the beds. There are nursing ratios for ICU and step down, similar to US, but there are no nursing ratios on the floor. Floor nurses can be responsible for 20-30 patients each. There are also no nursing assistants. Ports (transporters) help with some of the work traditionally performed by nursing assistants.
If you don’t have private insurance, you likely don’t get any preventative screening. There are higher rates of cervical and breast cancer because most Kenyan woman are not receiving proper screening. Very sad that the government cannot afford life-saving screening for the masses. People present when they are symptomatic, which usually means the cancer is pretty advanced.
Contact Information on who you interfaced with for nursing (principles, administrators, staff)
Virginia is the unit director of the Radiology Department
Spent time working with Harriet and Joshua, nurses
Also met with Dr. Miriam Wagoto (director of nursing of the University of Nairobi)
Lectures given
I lectured on Zoom for the residents, fellows from the University of Nairobi. Roughy 20 people attended the lecture. I spoke about my role as an IR NP and how I run the inpatient consultation service at UCLA. They don’t have nurse practitioners in Kenya. The closest thing to a mid-level practitioner is a clinical officer. A clinical officer is essentially a physician half way through med school training. Sometimes, in Kenya, physicians take a break half way during med school to work. These clinical officers often provide care in rural areas.
I met with the radiology nurses and Virgina one afternoon. I explained my role back home and asked each nurse for their opinion on things that could be improved in the department. Each nurses shared their perspective on things the changes they would like to see in the department. Virginia expressed disappointment because the doctors were not doing Time-Outs prior to procedures. I brought this up in my lecture with the doctors, in an effort to remind them of the importance we place on Time Outs prior to the procedure. I explained that we would never start a procedure without a Time-Out to ensure we have the right patient, right procedure, etc. Nurses also expressed concern about the lack of standardization for procedures. Antibiotics are not given to outpatients but are given to inpatients. Some patients receive an oral pre-medication prior to the procedure (Tylenol) where others do not for the same procedure. Nurses were requesting more anesthesia support for painful procedures so the patients aren’t suffering during the procedure. Nurses also would like to be trained to give sedation during the procedure to alleviate patient suffering.