I will make my first trip with the Asclepius Snakebite Foundation in late May and early June. I will help train our Guinean colleagues in emergency medicine and envenomation medicine. We will soon be opening our new clinic, which will be able to serve more snakebite victims. We plan to replicate this model in other parts of Africa and the world to help those most affected by venomous snakebite.
The people of Guinea will benefit from this project. Snakebite is a neglected tropical disease with a high burden on human populations in the tropical world. Many people die annually and many more are injured with long-term morbidity. Guinea has a high number of severe snakebites. We are able to treat over 500 bites per year in a single small facility. We plan to continue to develop our model in our new facility, which is set to open soon. The longer term goal is to replicate this model elsewhere to make a bigger impact on the snakebite problem.
The immediate impact will be to care for patients, gain firsthand experience in treating African snake envenomation, learn more about the patient population and the snakes and bring supplies to the clinic.
The longer term impact will be to replicate the snakebite clinic model in other vulnerable areas. As an emergency medicine educator, I will share my knowledge and experience with medical students, residents, and colleagues. It will also help in my efforts to secure funding for our organization.
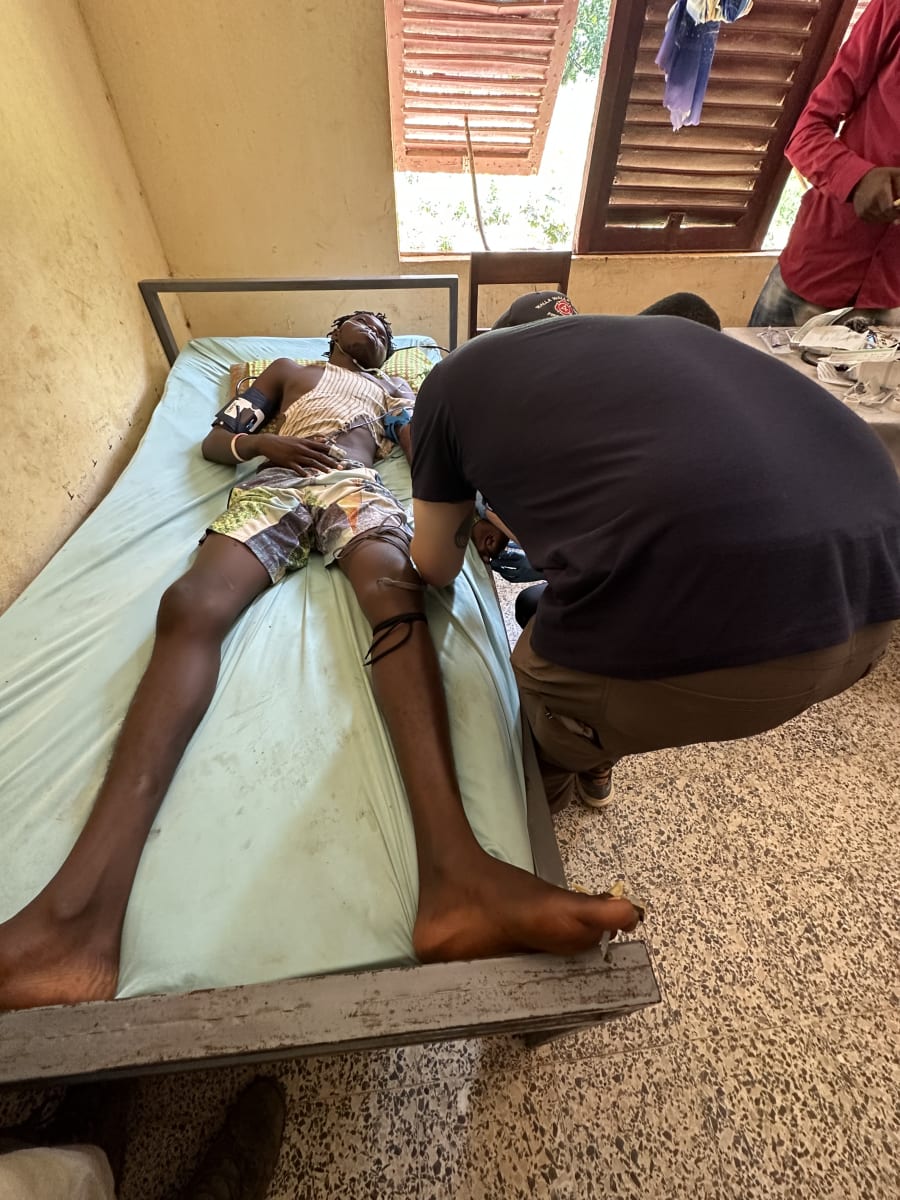














Guinea is a beautiful country with wonderful people. Unfortunately, a large number of Guineans experience poverty. Globally, snakebite envenomation is a disease that most affects the impoverished. People living off the land encounter venomous snakes frequently and bites are common in Guinea and throughout the tropical world. The mission of the Asclepius Snakebite Foundation is to reduce the burden of snakebite in such places. We do this by helping to provide safe and effective antivenom (the only current effective treatment), providing other medical equipment, teaching emergency medicine and critical care medicine, and studying the snakes that are causing the injuries. During my trip with ASF, we were able to further each of these goals. We brought a large amount of medical supplies, did instructional sessions with our Guinean clinician partners, and were able to capture and study numerous venomous snakes of different species. We treated several envenomation victims, one of whom was a 21 year old man who was dying from a a neurotoxic cobra bite. After antivenom administration and supportive care, he was able to go home to his family the next day. We also, unfortunately, saw delayed presentations of snakebite, including a 7 year old boy bitten on the ankle by a spitting cobra. Spitting cobra venom is highly tissue destructive. This boy lived far away from our clinic and had initially presented a week after the bite. He did receive antivenom at this time, but after a week, the benefit is greatly reduced. During our trip, he came for a recheck now 4 weeks after the bite. He had severe damage to the tissues of his leg and foot with exposed bone, tendon rupture, infection, and severely compromised neuromuscular function. This sad case reinforced why our efforts to provide timely antivenom and other rapid interventions are so important. If he had presented earlier and received antivenom, this outcome could have been prevented. Of course, we helped with any other medical issues that presented, which included malaria cases, infected wounds, scorpion stings, and other problems. We achieved all of our goals for this trip, but our long term goal is to see our Guinean clinic become self-supporting and then use this model to establish other similar envenomation clinics throughout Africa and wherever else there is a need.