I will be traveling to Lusaka, Zambia next month (May 2023) to assist the local anesthesia department with teaching regional anesthesia and pain medicine procedures. I will be there for two weeks to help teach and perform acute pain procedures for Zambians undergoing surgery. I believe my presence there will help build their local knowledge and expertise such that they can provide better pain control to their patients around the time of surgery.
Acute pain medicine is often a neglected aspect of surgical care in low-income countries. Patients often are not provided with postoperative analgesia due to lack of familiarity with regional anesthesia procedures or expertise. Even though regional anesthesia/pain procedures do not usually require expensive equipment to perform, these procedures are seen as requiring significant expertise. My teaching there will help them perform these procedures by themselves by providing in-person, real-time guidance.
I expect to help with pain control for the patients that I will encounter in Lusaka. I hope my expertise in this area will help local residents and attendings feel more comfortable performing these pain procedures after I leave.





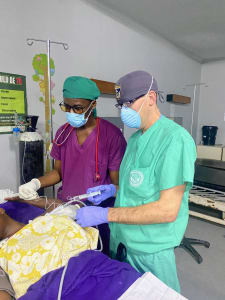



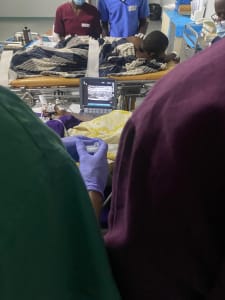
During my trip to Lusaka, Zambia, I spent two weeks at the University Teaching Hospital in Lusaka focused on teaching the local Zambian anesthesia residents in the operating rooms. We spent a great deal of time performing ultrasound-guided nerve blocks preoperatively and postoperatively to help Zambian patients with pain control around the time of surgery. We performed 23 nerve blocks in total over the two weeks for surgeries ranging from painful extremity fracture repairs to large exploratory laparotomies. Without my expertise, nerve blocks are not routinely performed at that hospital unless an external expert is available to help guide them during the procedures. Many of the nerve blocks served as their primary anesthetic, so general anesthesia was not needed (increasing the overall safety for the Zambian patients). We also spent a great deal of other time in the operating room performing general and spinal anesthetics for other types of surgery. In these settings, you do see a great deal of advanced pathology that you might not see in the US. Helping the residents safely navigate these patient's pathologies and provide a safe and effective anesthetic is hugely valuable for the local patients and surgeons. I also spent a great deal of time giving formal didactic lectures and organized an ultrasound workshop for them to practice their ultrasound and regional anesthesia skills. I was aided in my teaching by ZADP (Zambia Anaesthetic Development Program), which is a UK-based group of teaching fellows providing in-country education to Zambian trainees since 2012.
The local Zambian anesthesia residents were very grateful for the teaching and clinical care I provided. They want to be able to learn nerve blocks sufficiently so they can perform them independently once they finish residency. This type of teaching helps them achieve their goals. I hope my teaching and expertise there gives them the confidence and knowledge to perform nerve blocks for their patients in a safe and effective manner.
I will be returning next May to Lusaka to continue my work there with the emphasis on sustainability and capacity building. I cannot thank the Dox Foundation enough for their support during this trip and (hopefully) future trips.