While at Mulago Hospital/Makerere University in Kampala, Uganda I will spend time rounding with the inpatient pediatric team, exploring the specialty clinics, especially HIV clinic, and I will spend time teaching residents and students. My current training is in pediatric infectious diseases and therefore I will be doing a lot of teaching in this area, which is an area of need for teaching. My current research is in how healthcare personnel interact with freely available healthcare mobile applications and therefore I plan to explore the feasibility of using mobile applications in healthcare in Uganda or how applications need to be modified.
Both the patients that I will be seeing and the residents and students I will be teaching will benefit. Mulago hospital is the main regional hospital for the entire country of Uganda. In 2014-2015 the hospital only had 67% of their positions filled and were in need of more staff and had 829,817 outpatient visits and 761,573 inpatient admissions. This hospital is the primary teaching hospital for the Makerere College of Health Sciences. This population is underserved, understaffed, and presents with different illnesses and different problems than in the U.S.A. The residents and students will benefit directly from learning. The patients will benefit while I am there through care I provide and will benefit later through the information taught to the residents and students.
The expected impact will initially be in the instruction of the residents and students who will hopefully apply what I have taught them and this information will carry over once I have returned. I hope that information I gain in regards to use of healthcare mobile applications might lead to the development of healthcare applications that can apply to locations with limited resources and therefore be used globally from rural U.S.A. to different parts of the world that are low or low-middle income. The development of more mobile applications that can help with clinical decisions not only will carry over but hopefully have a global impact.


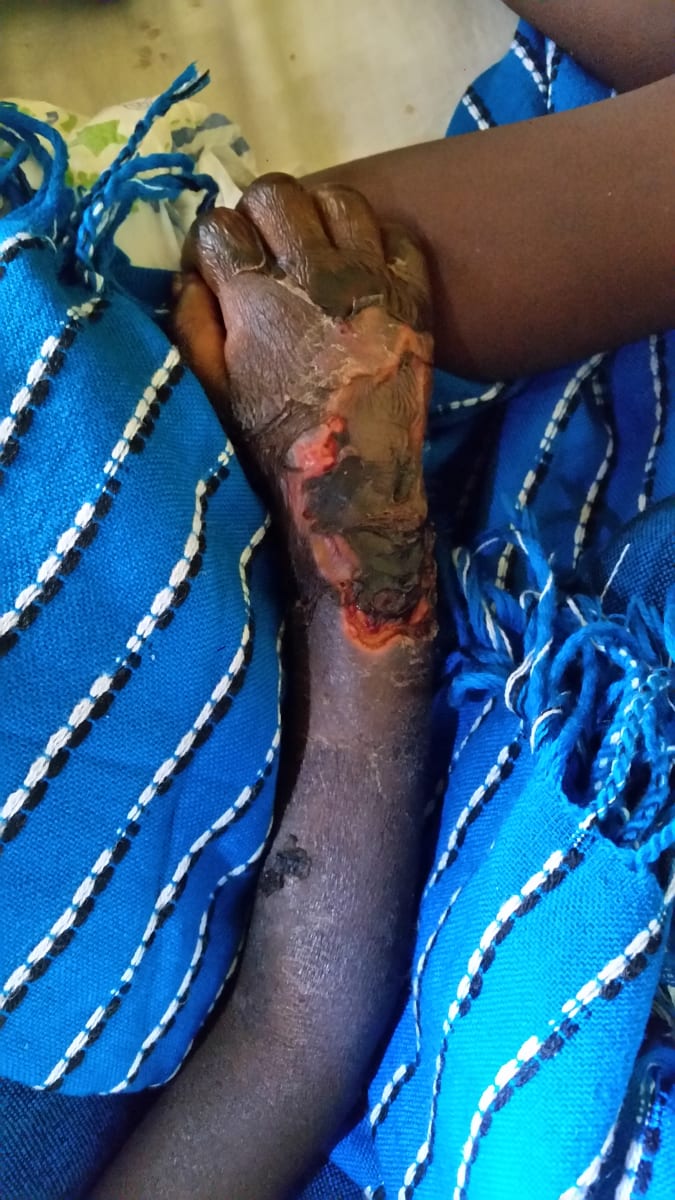
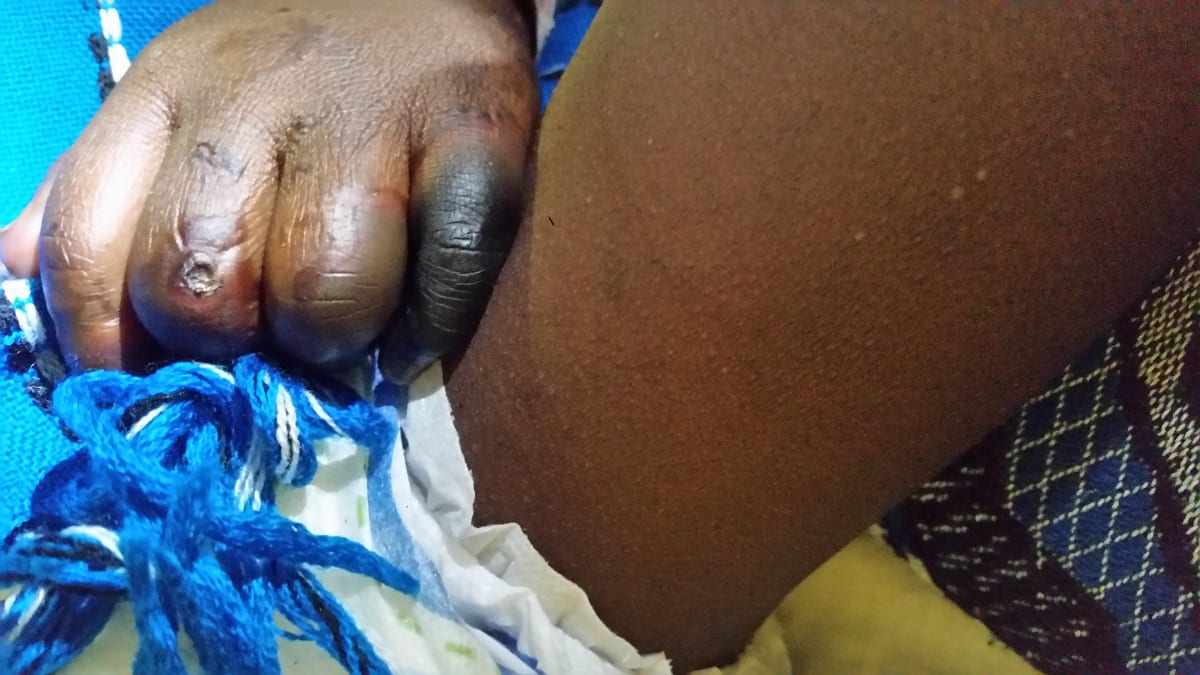












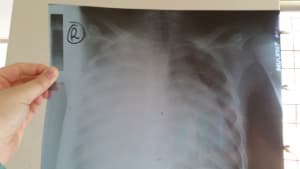






My time in Uganda was both good and hard. There are several limitations to practicing medicine in Uganda one of which is the fact that patients have to pay for things like labs, imaging, certain procedures, and consultations before they will be performed. This meant that as an infectious diseases physician I saw a lot of overuse of or improper use of antibiotics due to patients not being able to afford testing. This has led to a lot of antimicrobial resistance. I spent a lot of time seeing patients as well as teaching medical students, interns, and house officers (equivalence of residents). The trainees in Uganda excel at examination skills and are eager to learn. I especially loved teaching the students about antibiotics and how they work, neonatal sepsis in developing countries, and management of severe acute malnutrition. The different pathology seen in Uganda is fascinating. I saw a lot of congenital heart disease, neonatal seizures and fever, hyperbilirubinemia, endocarditis, pneumonia, and malnutrition. My pictures highlight the malnutrition ward with a zebra and giraffe statues outside and a child with severe acute malnutrition with edema and subsequent ulceration. There is another picture of a child with necrosis of some fingers, hand edema who had purpura fulminans. Her blood culture was pretreated and therefore I do not know what organism caused this, but she did recover with amputation of some digits. Another picture of a chest x-ray with empyema shows the purulence draining from the chest tube. This patient was still recovering when I left but doing well. I’ve also highlighted a parade that was taking place for breast cancer awareness as well as some of the wildlife that I could see right around the hospital with the monkeys. Not all of the patients survived due in large part to limited resources, however I was impressed by how hard many people worked including the picture of a couple of interns who I could trust to take good care of patients.