We plan to take an eighteen-member medical team consisting of twelve physicians, five nurses, and one physical therapist to serve in the community of Andajuaylillas Peru. We will plan to have three days of clinic in the town center, three days of outreach health fairs, and one day of home visits. We are estimated to see five hundred patients which will include children, adults, and home bounded patients. We will address both acute and chronic, screen for preventative diseases (hypertension, diabetes), and provide palliative care when possible. With our outreach health fairs, it’s not uncommon to see patients who have never seen a doctor. We will hire local Quechua interprets to communicate with non-Spanish speaking patients. Medications for acute and chronic diseases will be purchased and brought to treatment this community. We will partner with local community leaders and the local community to assist with continuity of care. When possible, we will provide tools such as with diet, physical therapy exercises, and recommendations on life style modifications to prevent disease and maintain their health. In previous years there was a single medical trip to Andajuaylillas, but in 2019 there will be three different medical trips to this community of which will be leading the second group. We plan to coordinate with the other two medical teams to better prepare and address the needs of the community.
We chose this rural agricultural population for several reasons. Within this community there is a large population of indigenous Quechua farmers that are highly underserved and limited in resources. Within the town center there has a single small clinic, but it’s not utilized by the surrounding Quechua communities due to lack funds, lack transportation, and occasionally feelings of discrimination amongst their population. Conditions commonly encountered conditions include hypertension, obesity, diabetes, skeletal muscular conditions, gastritis, dermatological conditions, women’s health issues, infectious diseases, mood disorders, and a need for well child checks and palliative care services.
Our goal is to screen for acute and chronic diseases (diabetes, hypertensive, CAD, obesity) to prevent the consequences of uncontrolled conditions. This will be accomplished by measuring vitals, history collections, physical examinations, and simple lab tests (urine analysis, urine pregnancy, blood sugar test, A1c blood test). When appropriate we will treat acute and chronic conditions with life style changes, medications, and physical therapy. We will attempt to partner with local community leaders and the medicine services for continuity of care. We will also share our demographic findings (age, gender, medical conditions, medications used and needed) with the other medical teams for later trips. The medical team members will also continue to benefit from this experience back in the USA by learning about cultural differences in healthcare and treatment in Peru, challenges of providing medical care in low resource communities, and work with interpreters to provide better care.




Within a 8 day period our medical team had the good fortunate to volunteer and serve in Andahuaylillas, Peru. Our medical team consisted of eleven physicians, five nurses, one physical therapist, seven interpreters, and one undergraduate student. Seven physicians were residents within our Family Medicine training program. During this period we saw and treated 691 patients. We saw primarily common medical conditions such as skeletal muscular pain, headaches, dyspepsia, dermatological conditions, fatigue, hypertension, and well child checks. These medical trips are an invaluable part of resident physician’s education as it allows them in experience medical practice in low resource communities, and treating patients from another country with limited access to physicians.
We conducted a number of home visits by breaking up into three medical teams. By foot we would travel to homes of house bounded patients. In this photo one of our residents treats a patient with advance osteoarthritis with a intra-articular steroid injection.
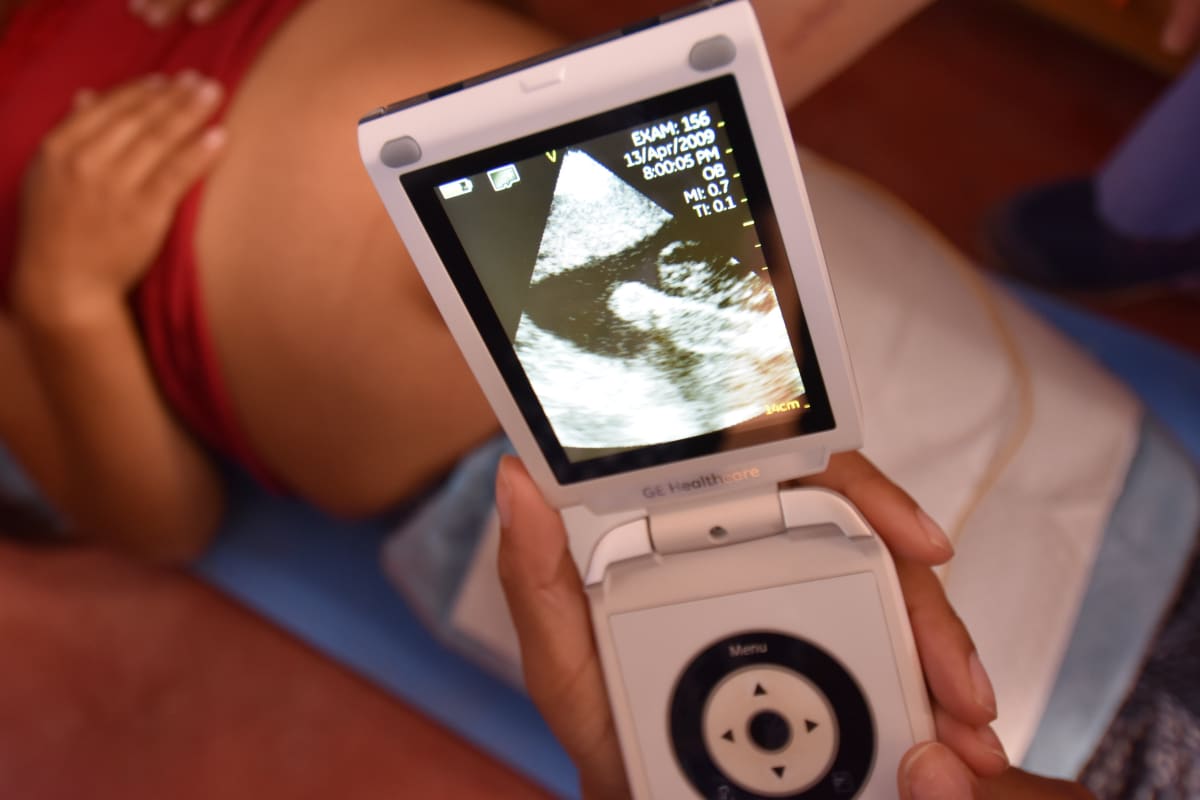
On this trip we brought a hand held ultrasound device for point of care usage in the primary care setting. This device was used to show a young female at 37 weeks gestation her baby for the first time. Her smile was priceless as she watched her baby’s arms and legs move about on the screen of the ultrasound.
Education is a huge component while volunteering abroad. Here a resident physician educations a patient on diet and lifestyle changes to prevention hypertension and diabetes.
Thank you, Dennis Andrade