The Orthopedic Overseas program is based at Yangon General Hospital, the major trauma hospital in the region. As a hand and orthopedic surgeon, I work with the local orthopedic residents, fellows, and attendings. I provide instruction during morning fracture conference, in outpatient clinics, during ward rounds, and in the operating theatre. I also give formal lectures as needed. I never operate alone. Rather, I supervise or assist the local surgeons and trainees. I also schedule teaching sessions with the staff and nurses about the basics of orthopedic care.
Most patients at Yangon General are victims of road traffic accidents and industrial injuries. Many patients have infections. Nearby Yangon Orthopedic Hospital provides reconstruction, oncology, and elective treatment. The Pediatric Hospital addresses the non-trauma needs of children. All three of these are public, civilian hospitals.
My goal is to teach the residents clinical decision making skills, focus on the basics of orthopedic care, and assist them with complicated orthopedic. I never recommend anything they couldn’t do for themselves, or resources they don’t already have. The hope is to create a more sustainable model of volunteerism.
This will be my third visit to Myanmar in six years. I am the program director of the Myanmar site. In addition to the above duties as a volunteer, I also plan to assess the impact of the project. I will see how the volunteer program has improved patient care and clinical outcomes. I will ascertain what the residents feel are gaps in their education, and whether future volunteers can help meet those needs.




















Navigating around Yangon General Hospital (YGH) is no mean feat. Yangon General Hospital is a public 2000 bed facility, a red brick Victorian structure built by the British in 1899.
As an HVO volunteer my focus was teaching, not doing. The orthopedic department has grown over the last few years. The hierarchical team includes professors, associate professors, consultants, fellows, residents, interns, and medical students. There are currently 80 orthopedic residents in the 3 year program, with fellowships available in Hand, Pediatrics, and Spine.
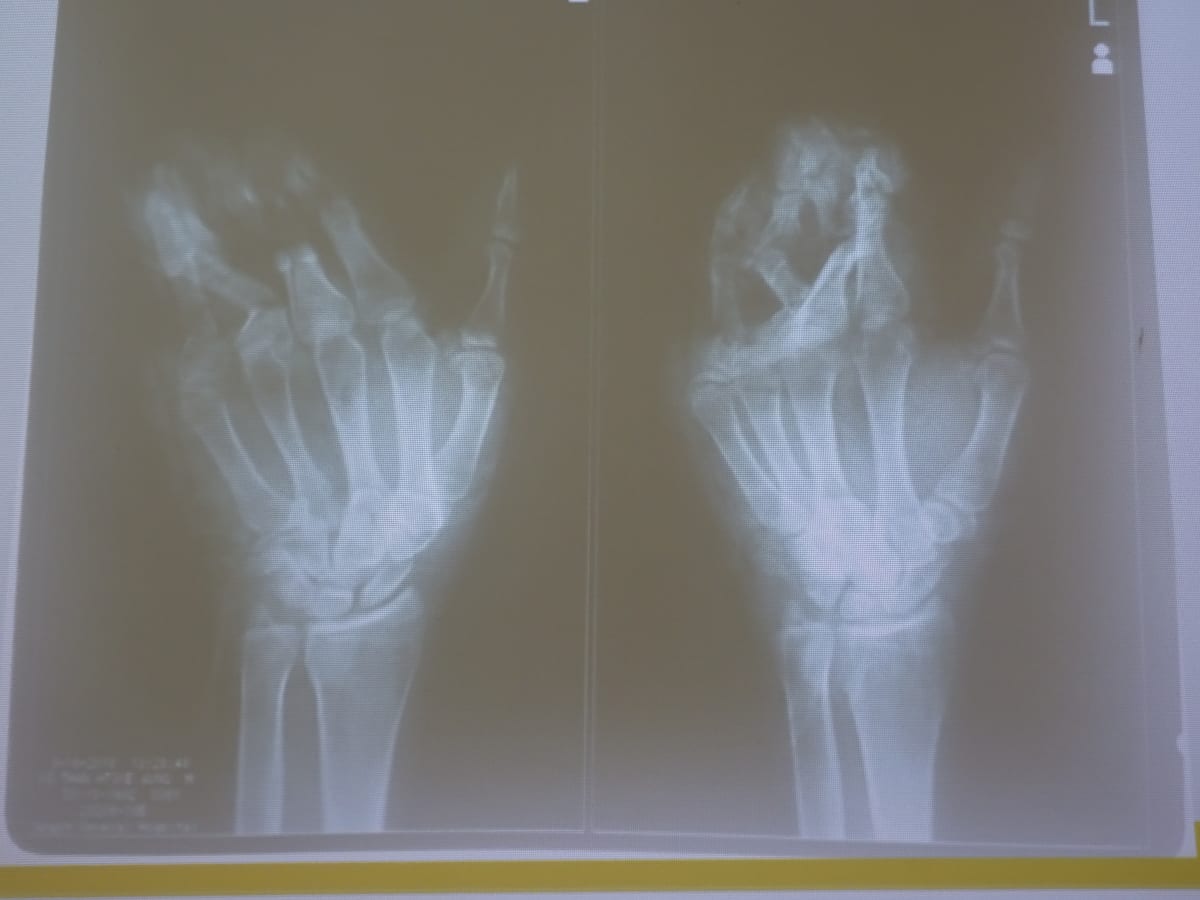
As a senior consultant (in hand and general orthopedics), I provided feedback during the morning fracture conference (“audit”), where the on-call resident presents admissions from the previous 24 hours. The majority of these patients are polytrauma victims from road traffic accidents. Trauma affects the poor disproportionately. Traffic is chaotic and poorly regulated. Industrial injuries are also common. In my first week I saw three patients with injuries from sugar cane juicing machines alone. The safety guards on the juicing machines had been removed. These hands were mangled, with extensive bony and soft tissue damage, with little hope for regaining much function.
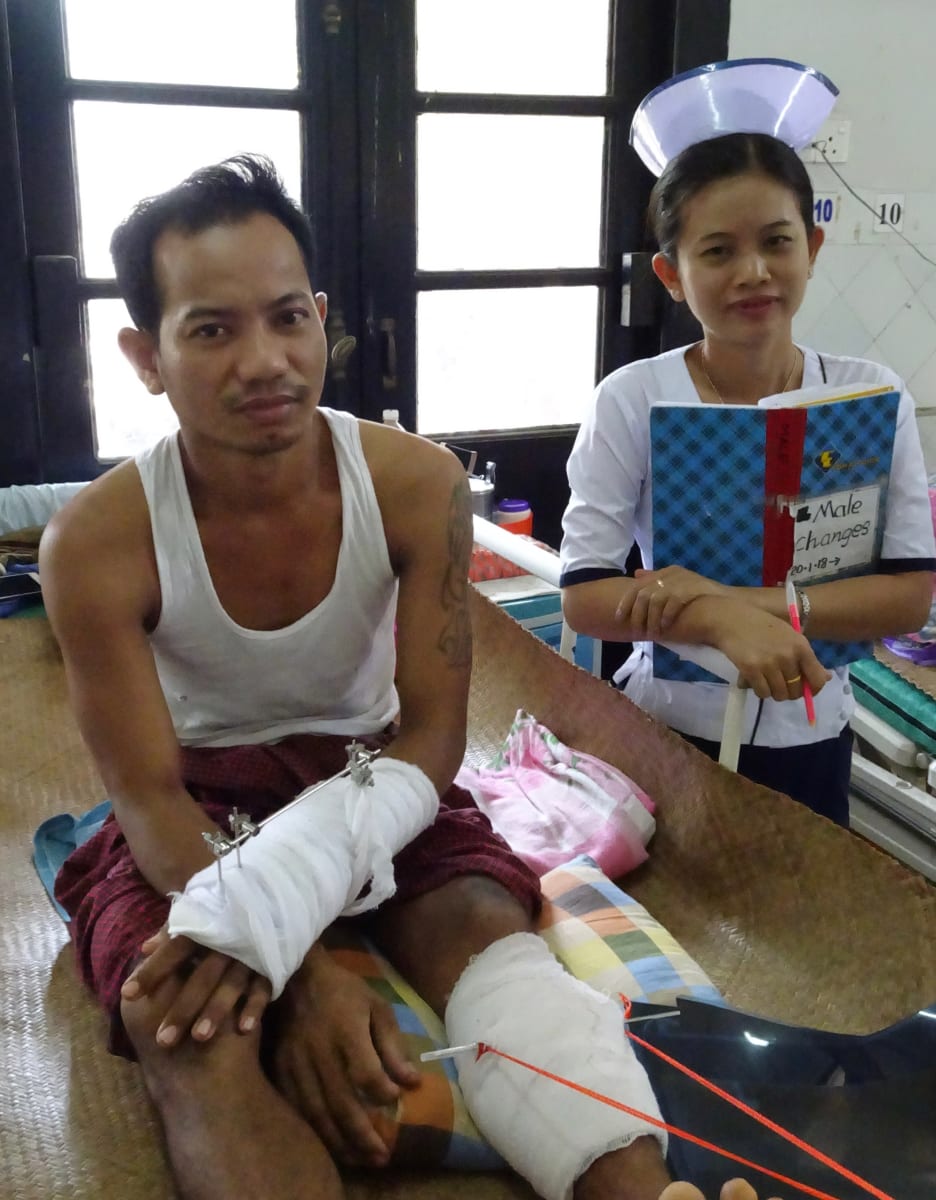
The residents perform basic wound debridement and preliminary stabilization in a surgical suite adjacent to the emergency room. The orthopedic wards are filled with patients in external fixators and traction for their various long bone fractures. Some patients wait weeks for their definitive surgeries. The delay can lead to malunions, blood clots, pneumonia, and skin breakdown. Soft tissue and bone infections are common on the wards. There are no hand washing stations and few hand sanitizer dispensers. The lack of infection control is disheartening. Given the number of in-patients, rounds were done hurriedly. I focused on the basics (e.g. documenting radial nerve function after a humerus fracture; use hand sanitizer between patients.)
The residents are well versed in fracture classification systems. These systems can help determine mechanism of injury and guide treatment. Treatment guidelines are often developed in places like Switzerland. The criteria may be less relevant places with different pathology and resources. I encouraged the residents to “treat the patient, not the X-ray.” We considered patient age, medical comorbidities (e.g. malaria, HIV, Tb), and resources available (e.g. OR time, implants, and fluoroscopy) in patient care.
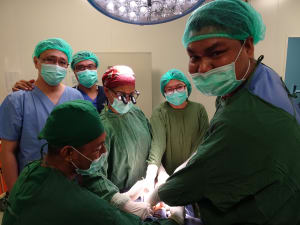
The Hand Surgery Unit is skilled in microsurgical procedures, including fistula placement and brachial plexus surgeries. I observed a para-umbilical, antero-lateral thigh, groin, and supra-malleolar flaps. I rarely do flaps in my community-based practice in the US, so I was of limited help in these cases. I was more useful in bony and ligamentous surgeries, such as multiple metacarpal fractures, a scaphoid dislocation, and a base of the thumb metacarpal fracture.
When not in the operating theatre, I staffed the outpatient clinics. Many poor patients don’t seek care until the injury becomes disabling, resulting in chronic dislocations and malunions. We saw an incarcerated 34-year-old man who had a neglected mid-shaft both bone fracture which had gone on to malunion. He presented with a deformed and painful forearm. We rounded on him in the hospital jail, located in the dungeon of the building. His surgery involved shortening and plating the fractures.
As is often the case, I learned as much as I taught. I saw examples of tuberculosis in the upper extremity, including the elbow and wrist. The wrist masses clinically appeared to be ganglions but were in fact “melon seed” granulomas of the wrist and hand. Occasionally there were heartbreaking cases with no easy solutions. There was a case of a 53-year-old man who had been diagnosed with a sarcoma of his forearm the prior year. He had been lost to follow-up, and now presented with a massively enlarged right arm, lymphedema, and nerve compression. Given the aggressive extent of the tumor, he was likely to lose his arm (if not his life).
I presented a few formal lectures for the junior and senior residents, covering a variety of topics. For both groups, I reviewed distal radius fractures and the various treatment options. I discussed the biomechanics and indications for volar locked plating. This is a relatively new technique in Myanmar, and I focused on preventing complications with the available implants.
The month in Myanmar passed quickly. Despite the limitations of teaching in English, (the national language is Burmese and comfort with English varies widely) I did feel that my efforts were beneficial. The lack of resources, infrastructure, and injury prevention can be frustrating. I believe educating the local health care providers is vital not only for patient care, but also for addressing these larger systemic issues.