Head and Neck Outreach (HNO) is a non-profit organization founded in 2014 by Dr. Chad Zender and Katrina Harrell in collaboration with Dr. Jeff Otiti of the Uganda Cancer Institute (UCI). HNO currently operates in partnership with UCI and Makerere University School of Medicine to train the next generation of Ugandan clinicians and to provide diagnosis and treatment services to a severely underserved population.
The World Health Organization (WHO) considers surgery to be an integral part of primary health care as a preventative strategy and cost-effective method for addressing many health challenges in developing and low socioeconomic countries. In many of these countries, such as those in Central and East Africa, the burden of surgical disease far surpasses provided capacity. In Uganda, a country of 37 million people, the ratio of surgeons to the population is 7 to 1 million. As a result, the majority of the population lacks access to quality surgical care. The HNO team was the first to successfully perform surgery at UCI and to date, the program has performed over 250 complex head and neck surgeries and treated more than 500 patients in clinic.
Head and Neck cancer affects individuals worldwide, with approximately 600,000 new cases diagnosed globally each year. In countries like Uganda, without health care systems that are able to provide access to radiation therapy, surgical resection and reconstruction is the only treatment option. Having only 30 ENT specialists in the country and only one fellowship-trained ENT oncology specialist, Ugandans suffering with head and neck conditions are unable to receive adequate diagnostic and therapeutic interventions.
To address Uganda's discrepancy of resources, HNO established a partnership with Dr. Jeff Otiti of the Uganda Cancer Institute and became the first group to successfully perform surgeries at UCI. HNO now travels to Uganda biannually to complete two-week surgical camps, evaluating patients in clinic and performing complex head and neck surgeries. Physician referrals and word of mouth recommendations have resulted in patients traveling across Uganda as well as neighboring countries.
From a clinical perspective, we anticipate a high surgical workload, with daily operations from morning to evening. Our primary objective is to maximize patient treatment within our limited time frame. In addition to helping the patients and their families, HNO incorporates a professional education component to aid local clinicians, nurses, and students in developing skills to apply long-term. We believe that empowering the local health professionals will lead to sustainable changes that endure far beyond our trips alone.
As a rising PGY-5, this opportunity presents a chance to refine my clinical and surgical skills in managing head and neck cancer with limited resources. I’ve also considered embarking on mission trips as an independently practicing otolaryngologist, and I believe this experience will significantly shape my career trajectory. I hope to use this opportunity to gain a deeper understanding of global surgery and become a more vocal advocate for patients from underserved communities.
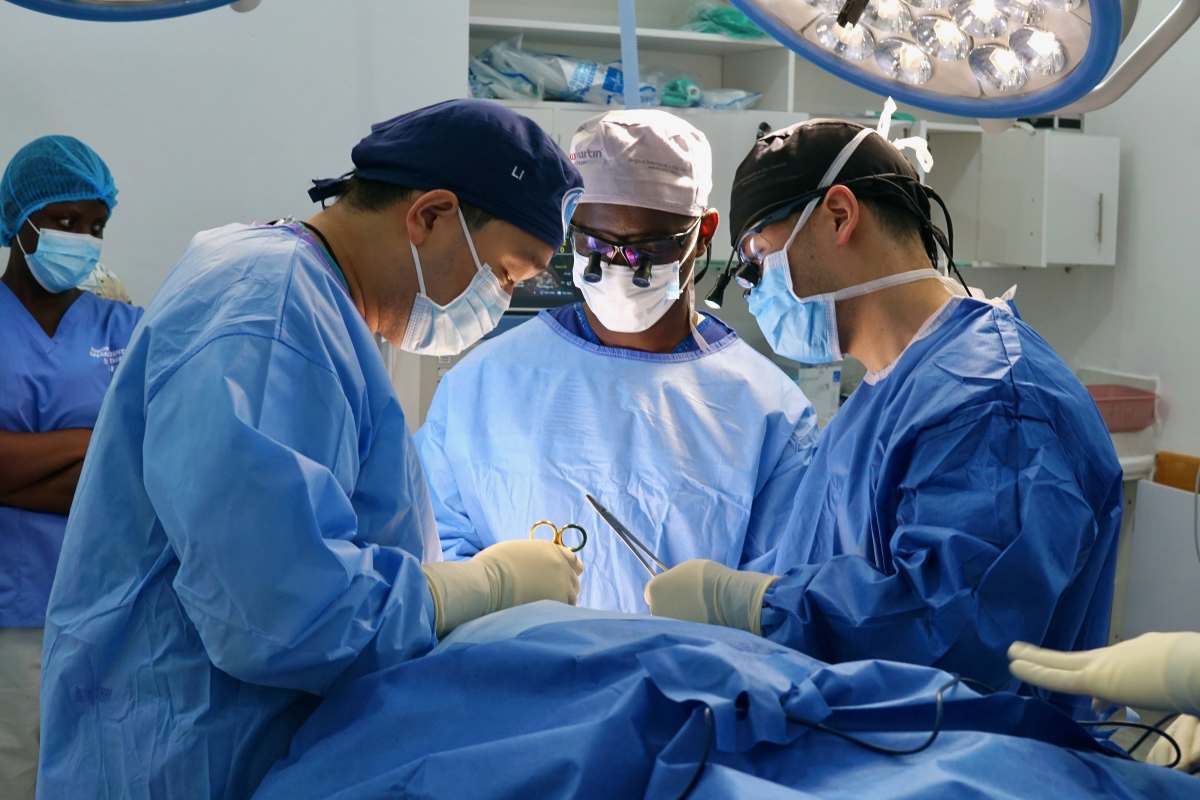
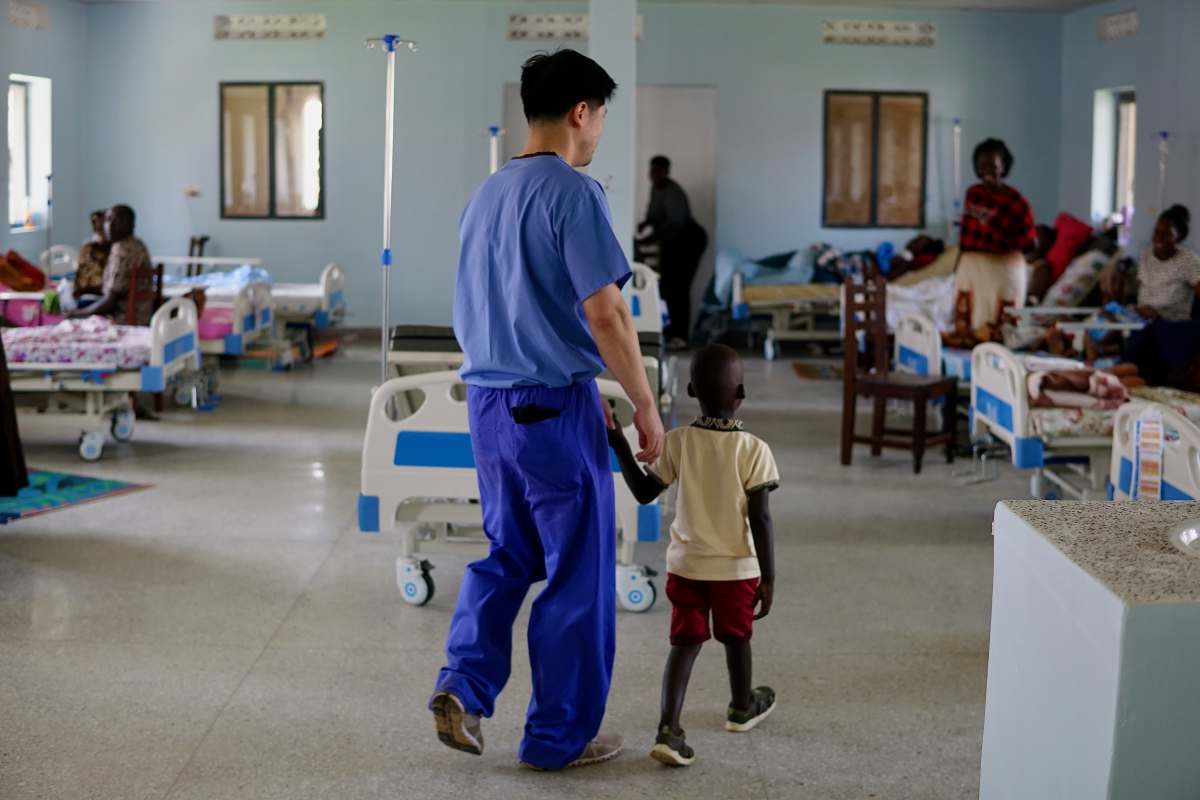








As head and neck surgeons, our recent mission to Uganda was an opportunity to apply our skills where the need is immense. Working alongside our dedicated local partners, Dr. Jeff Otiti and Dr. Isaac Mukiibi, our team treated patients with benign and malignant head and neck tumors, many of whom required complex free flap reconstructions. These local partners worked diligently to identify patients who would most benefit from our specialized services.
We started our trip with a clinic on Sunday to screen potential surgical candidates. We then traveled to Kiwoko Hospital, a private community hospital located about two hours north of the capital. While Dr. Zender's organization has been active in the region for over a decade, this trip was one of the highest-volume in terms of complex cases with a final case list that included eight surgeries requiring microvascular free tissue reconstruction and a similar number of lower-complexity procedures. With only two fellowship-trained head and neck surgical oncologists and one fellow, Ugandans face a tremendous imbalance between the demand for care and the supply of specialized providers. The patients we treated had traveled from all over the country, seeking a level of care that is simply unavailable to them locally.
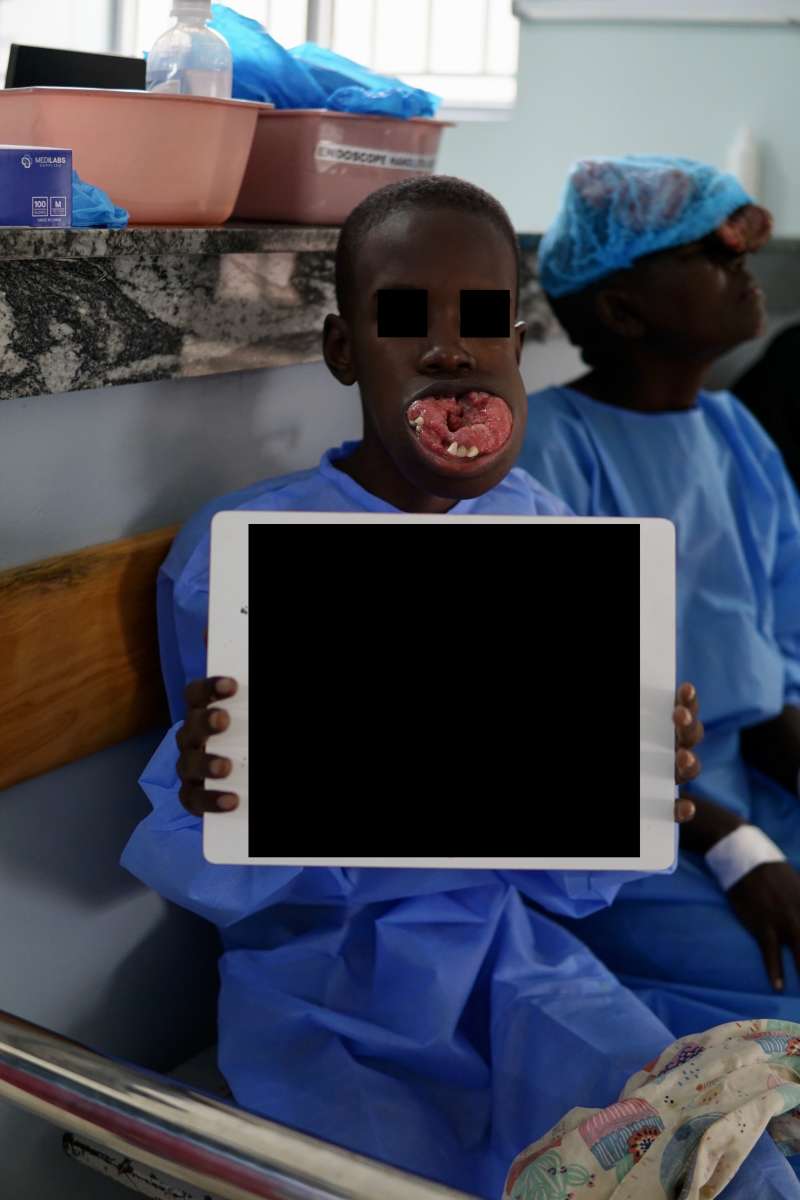
During our surgical camp, we treated patients with extremely bulky tumors. One case was a middle-aged woman with a large scalp cancer (dermatofibrosarcoma protuberans) that prevented her from opening her right eye. Another was a teenage boy with an ameloblastoma that was eroding his entire mandible, making it impossible for him to maintain adequate nutrition.
We also performed surgeries to improve patients' quality of life. One such case was a middle-aged woman who had unilateral vocal cord paralysis following a previous vagal paraganglioma resection. We were able to restore her voice by performing a medialization thyroplasty, using her own thyroid ala as a graft. Working closely with our Ugandan ENT colleagues, we were able to share surgical techniques that will help augment local care for years to come.
Beyond our surgical accomplishments, our mission was defined by the new friendships and partnerships we forged. With the Uganda Cancer Institute expanding its own surgical capacity, our organization has been searching for a new site where our team can provide the most impact. We believe we have found our new home at Kiwoko Hospital. When we departed, we were proud to leave behind leftover supplies, including a Bovie machine and a set of bipolar forceps. The surgeons at Kiwoko were particularly excited about this equipment, which will support their work and serve their community long after our team has gone.