I plan to work with Ugandan experts in medicine to care for children who are hungry and sick -- who we expect to grow and heal with specialized care.
In general, the objective of the elective project is to partner and work to assess, describe, and assist with the current treatment of malnourished children according to the internal program’s defined goals and UNICEF guidelines on the Integrated Management of Acute Malnutrition.
The internal program or institution abroad is: The Mwanamugimu ("Healthy Baby") Nutritional Unit. This unit is an inpatient nutrition ward of the Mulago Hospital in Kampala, Uganda. Recognized as center of excellence in clinical care and teaching in the management of children with severe acute malnutrition, it is staffed by pediatricians, nurses, and nutritionists. The Mulago Hospital is a teaching hospital partnered with Makerere University - Department of Pediatrics and Child Health.
(https://www.unicef.org/uganda/stories/ therapeutic-feeding-programme-turns-tide-battle against-malnutrition-uganda)
The primary beneficiaries of care at the Mwanamugimu "Healthy Baby" Nutrition Unit will be: children meeting criteria for inpatient care of severe acute malnutrition (ie, marasmus and kwashiorkor) and their mothers in the broad catchment area of the Mulago National Referral Hospital. This includes Uganda and commonly refugees from Congo.
The secondary beneficiaries should be the long-term attending physicians, nurses, and administrators at the local institution. That is, the project should serve the leadership and staff who work full-time and longitudinally for malnourished children and their mothers in Uganda.
We can and should prioritize this population of kids and moms based on their need for basic health care services.
The expected impact will be to lend support to ongoing care of malnourished children, and to leave at least one useful project to support the dedicated local physicians and staff.
Specifically, impact objectives on 'giving back' should align first with what the overseas mentor attending physician suggests would be most helpful to the nutrition ward. From previous work together, one attending physician Dr. Nicolette Nabukeera-Barungi had asked me to prepare training/orientation materials, including 5 minute videos, for first year medical students who have a 1-week rotation through the nutrition ward. These training materials may relieve some of the burden to the nutrition ward's full time staff on orienting new trainees every week.
Another objective would be to capture useful data and observation from outstanding care of malnourished children in addition to what staff are doing currently. This extra data collection could aid in ongoing research and quality improvement project -- specifically, the applicant (myself) could spend additional time contacting and documenting the reasons for loss to follow up in children who are discharged to the
outpatient malnutrition feeding program, and present the findings to leadership.
Finally, findings could also be compiled to demonstrate clinical excellence that benefits kids and moms in Uganda for promotion and philanthropy.



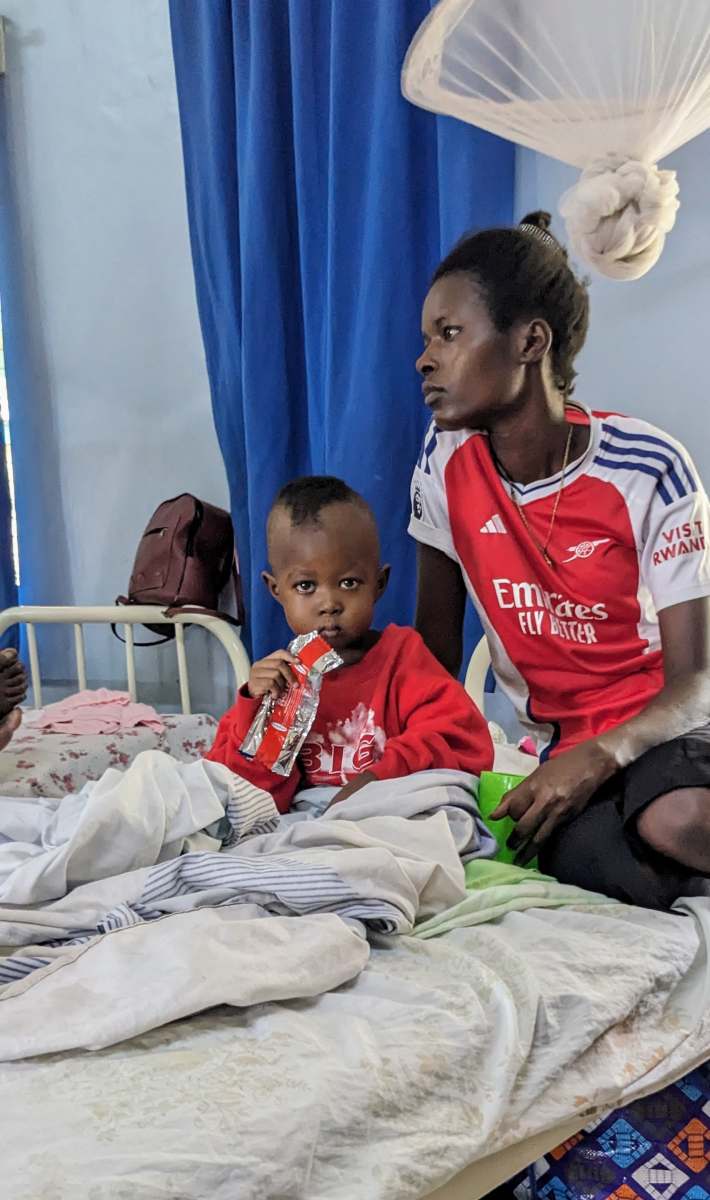










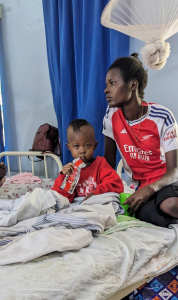




I had a wonderful visit returning to see my friends and colleagues at the Mwanamugimu Healthy Baby Nutrition Unit in Uganda!
Pediatricians with many years of experience of clinical care and research for malnourished children run a special unit at Mulago Hospital in Kampala, Uganda. This unit admits children with complicated malnutrition – the kids who need special therapeutic feeding and complex care.
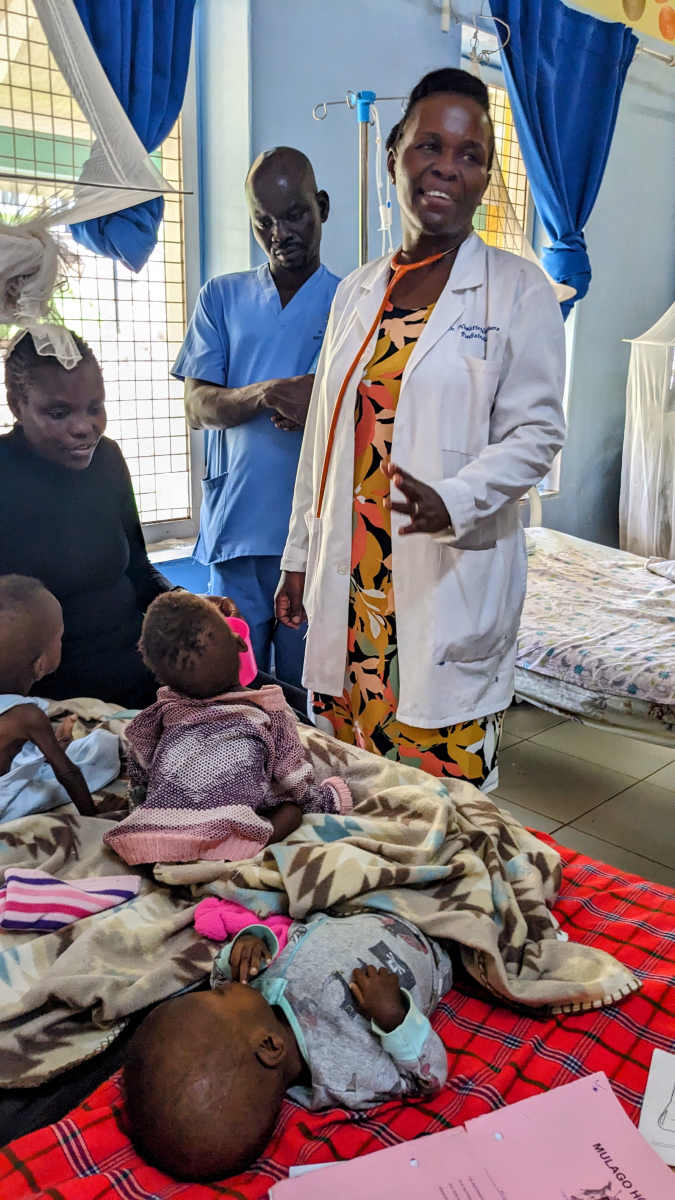
Two of the leaders are Dr. Nicolette and Dr. Esther, who are both professors of pediatrics. I worked to support their project and take care of children who were staying in the nutrition ward while they recovered.
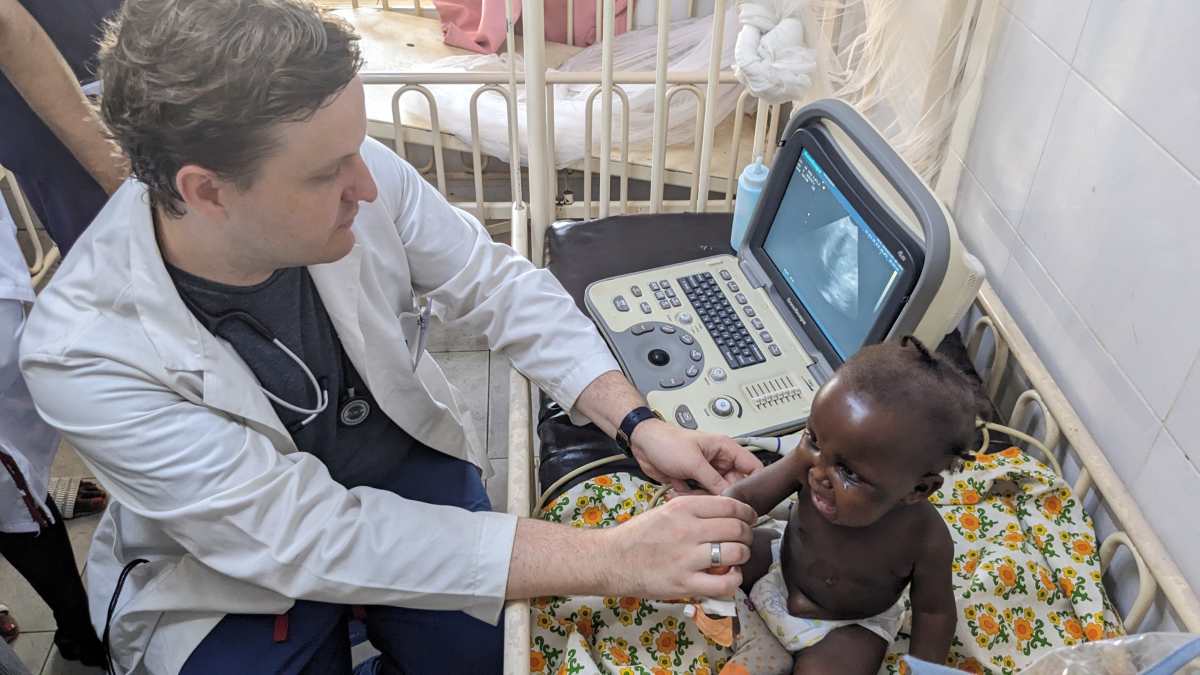
Dr. Nicolette’s research includes ultrasound to show the changes in certain organs during malnutrition, and we used her ultrasound machine to check children with severe forms of edematous malnutrition.
Many children are able to be medically stabilized from a severe condition like pneumonia, and then are able to graduate through a series of planned care regimens and feedings. Children who are almost ready to go home with special feeds take a peanut-butter based nutritional product. This produce is called ‘Ready-to-Use Therapeutic Food.’ The pouches that we use and send families home with are made locally in Kenya! UNICEF supplies these to our nutrition ward.
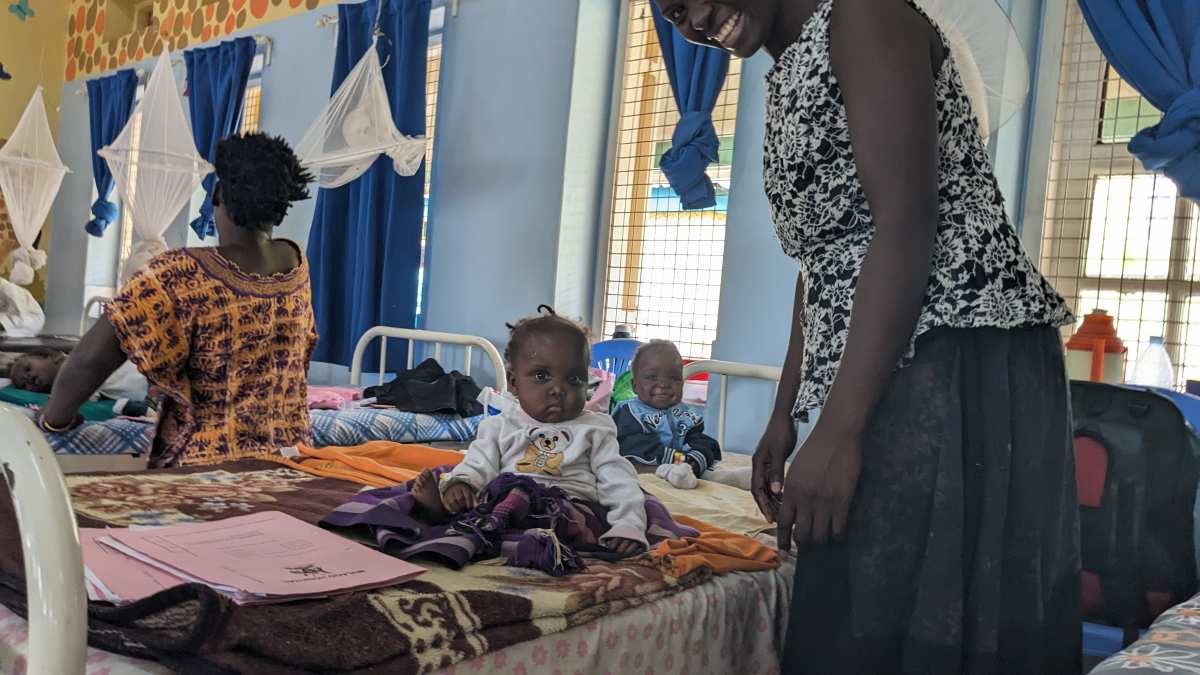
The children, like the ones in the pictures, are able to heal and grow enough to go home with a healthy appetite and a supply of the specialized food. They get to return home (thank goodness!) and come back once per week for more pouches of special food until they have gained a healthy amount of weight. That is the success story – just like the young boy “Mr. Big” and his mom!
I am grateful to the pediatricians, nurse managers, and nutritionists who work to make this special Healthy Baby Nutrition Unit running smoothly, so that kids and moms can heal and grow!