UNC Chapel Hill has a hospital in Malawi with a solid infrastructure to support residents and medical students. However, there are multiple GI issues that are under-recognized and treated for this population. Liver disease is unfortunately quite common. This includes chronic Hepatitis B (and its complications), alcohol-related liver disease, hepatocellular carcinoma as well as non-cirrhotic portal hypertension from Schistosomiasis. Currently, there is no dedicated personnel at Malawi that are able to provide longitudinal care for these patients. My aim is to develop and teach a curriculum related to early detection and management of liver disease/portal hypertension to the current trainees and attendings at Kamazu Hospital in Lilongwe, Malawi. This will include a didactic curriculum as well as endoscopic teaching for patients with liver disease/portal hypertension. The goal is to spread this curriculum to all relevant trainees and provide them with the tools to care for these sick and underserved patients.
There are substantial disparities in both access to and quality of liver-related care in Malawi, particularly for the diagnosis and management of portal hypertension and cirrhosis. The high prevalence (almost 8%) of hepatitis B virus (HBV) infection is compounded by limited access to screening, with most testing restricted to hepatitis B surface antigen and basic liver function tests; advanced diagnostics such as HBV DNA quantification, transient elastography, and liver biopsy are rarely available outside major urban centers, leading to underdiagnosis and late presentation.
Out project will ultimately benefit the population of the people of Malawi to help improve their care of liver disease. But it will also spread awareness of early detection and screening for chronic Hepatitis B and liver carcinoma. Finally it will benefit the medical professionals and trainees who will be directly learning a new skillset to care for their patients; with an eye on developing mechanisms for early detection and screening.
The impact should be immediate as we will be providing direct care to patients. It will also give local providers skills to continue this treatment plan until we can return for future trips. Secondary goals will be to create a portal hypertensive registry to study the global health of this population and areas of need. This will then be used to modify the curriculum and support given to the local providers.
There is a longitudinal plan to return to Malawi as well. There are three current gastroenterologists/hepatologists at my institution that will rotate every 6-9 months on trips to Malawi to continue to support the local healthcare and infrastructure. We will use the data from our portal hypertensive registry to target the biggest needs for this patient population and develop interventions to improve their health.

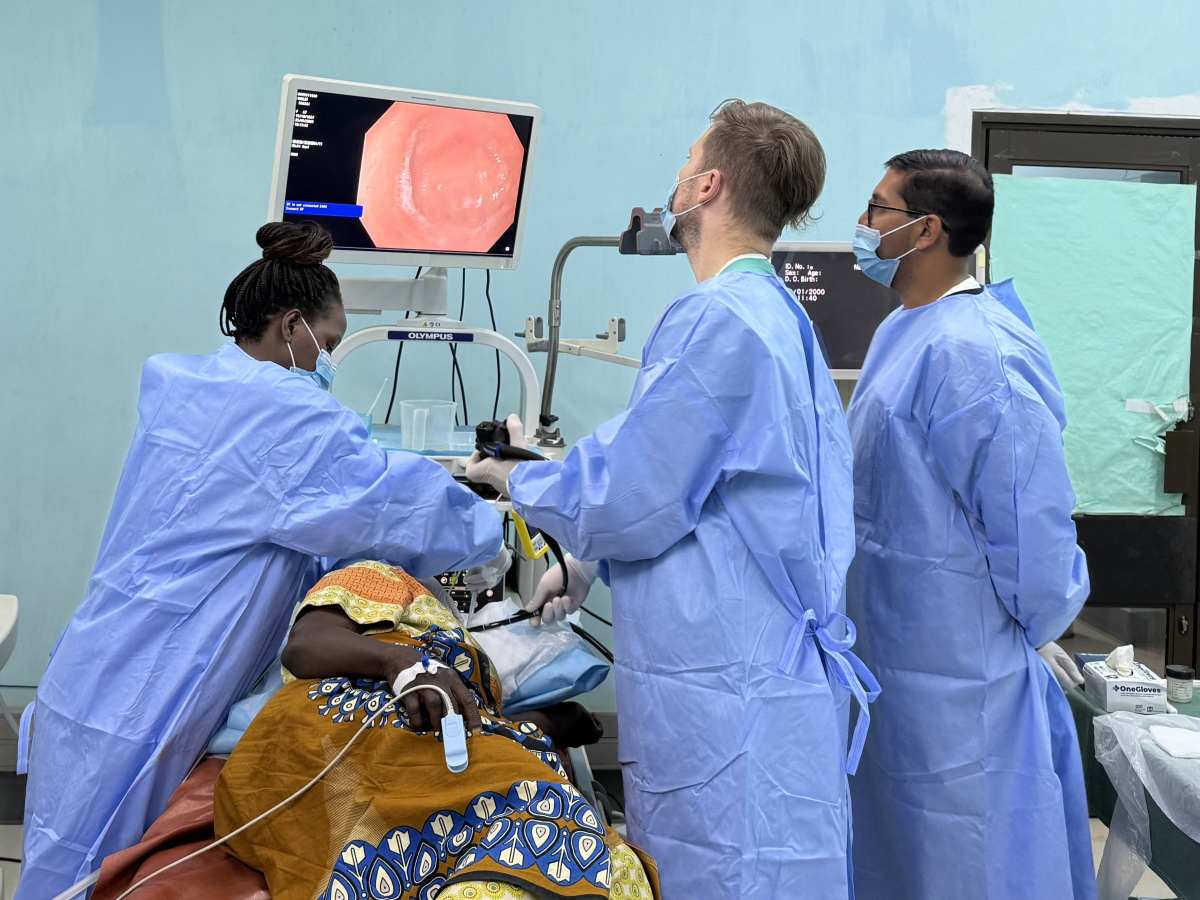







The people most impacted by my trip to Malawi were the patients living with advanced liver disease—individuals who often present only when portal hypertension has already led to life-threatening complications. This a country where about 8.1% of adults carry hepatitis B surface antigen, and chronic liver disease is a major and under-recognized public health problem. Furthermore, schistosomiasis is endemic and also leads to portal hypertensive bleeding. These patients, along with the clinicians who care for them in an overstretched system, were the primary beneficiaries of the work we began in building a structured portal hypertensive initiative.
During my time at Kamuzu Central Hospital, I saw patients arriving in crisis: massive GI bleeding, advanced cirrhosis, and esophageal cancer. Many of these individuals only present to care when complications of portal hypertension have already set in, because early diagnosis and specialized liver services are limited. Many were transported by “guardians” from rural areas, exhausted and desperate for answers. In the endoscopy suite I assisted with unsedated procedures and helped band bleeding varices—a lifesaving intervention in a setting with few alternatives.
Local clinicians and trainees were deeply impacted, too. Many had never received structured training in portal hypertension or cirrhosis management. Through bedside teaching, didactic sessions, and hands-on endoscopy, I saw their confidence grow. They also promised to continue teaching these skills after I left, expanding the ripple effect of our work and setting into place some of the protocols that we hope will allow for improved care.
In a health system burdened by limited resources and a high prevalence of liver disease, this initiative was more than academic: it offered a path toward earlier detection, safer treatment, and real hope for patients who otherwise face very poor outcomes.