As part of the Yale Interventional Radiology (IR) Global Outreach initiative, I will help to bring IR to remote parts of the globe, such as Tanzania. IR uses various imaging modalities to perform minimally invasive procedures, and to diagnose and treat a wide range of conditions. With the help of Ultrasound, Computed Tomography (CT), and Fluoroscopy, the interventional radiologist performs procedures that often allow for shorter hospital stays and lower complication rates than comparable open surgical approaches. IR is recognized as integral for diagnosis and treatment in modern medical care and adds great value to the healthcare system. Unfortunately, many third-world countries do not have the staff or facilities to train their doctors in IR procedures, or to provide these services to their patients. With the IR Global Outreach Program, we not only provide the exposure and training related to IR, but also teach the various institutions how to establish their own procurement process in order to maintain sustainability. Having an IR service onsite will help provide, cheaper, faster and safer solutions to many of the medical problems that would otherwise bring about significant morbidity, lengthy hospital stays and even death within a given patient population. For example, a procedure as simple as percutaneous abscess drainage can help fend off the ensuing sepsis and possible death that quickly follows if not treated quickly and adequately.
Based on the findings of an initial IR readiness assessment, we developed a plan to address the urgent need for IR in Tanzania. We believe that establishing an IR training program in Dar es Salaam in collaboration with RAD-AID and other academic institutions from across the US will provide the most effective and sustainable solution with lasting impact on the Tanzanian healthcare system. Our efforts are currently concentrated on the Muhimbili National Hospital in Dar es Salaam, a hospital with modern-day facilities and the necessary staff and radiology residents to make the setting up of IR facilities more sustainable. We are also working with the IR program of RAD-AID and the Resident, Fellow and Student section of the Society of Interventional Radiology (SIR RES) on creating an IR curriculum for the resource limited setting. This will provide an educational blueprint for establishing and maintaining comprehensive Interventional Radiology training programs in the developing world. The curriculum focuses on teaching routine and high yield procedures with supplementation of more complex procedures as the program matures. Lastly, the radiology residents at Muhimbili National Hospital will attend weekly IR lectures via the web given by faculty at Yale, Emory and the Montefiore Medical Center--the same lectures given to their respective home residents.
The end-goal is a self- sustaining IR residency program at Muhimbili, with Tanzanian IR faculty training Tanzanian residents. In collaboration with RAD-AID and academic hospitals from across the US, we are planning to send up to thirty groups of interventional radiologists accompanied by IR technologists and IR nurses to Tanzania in two-week blocks over the next three to five years. I will be in attendance with the group traveling in February 24 to March 10, 2019.


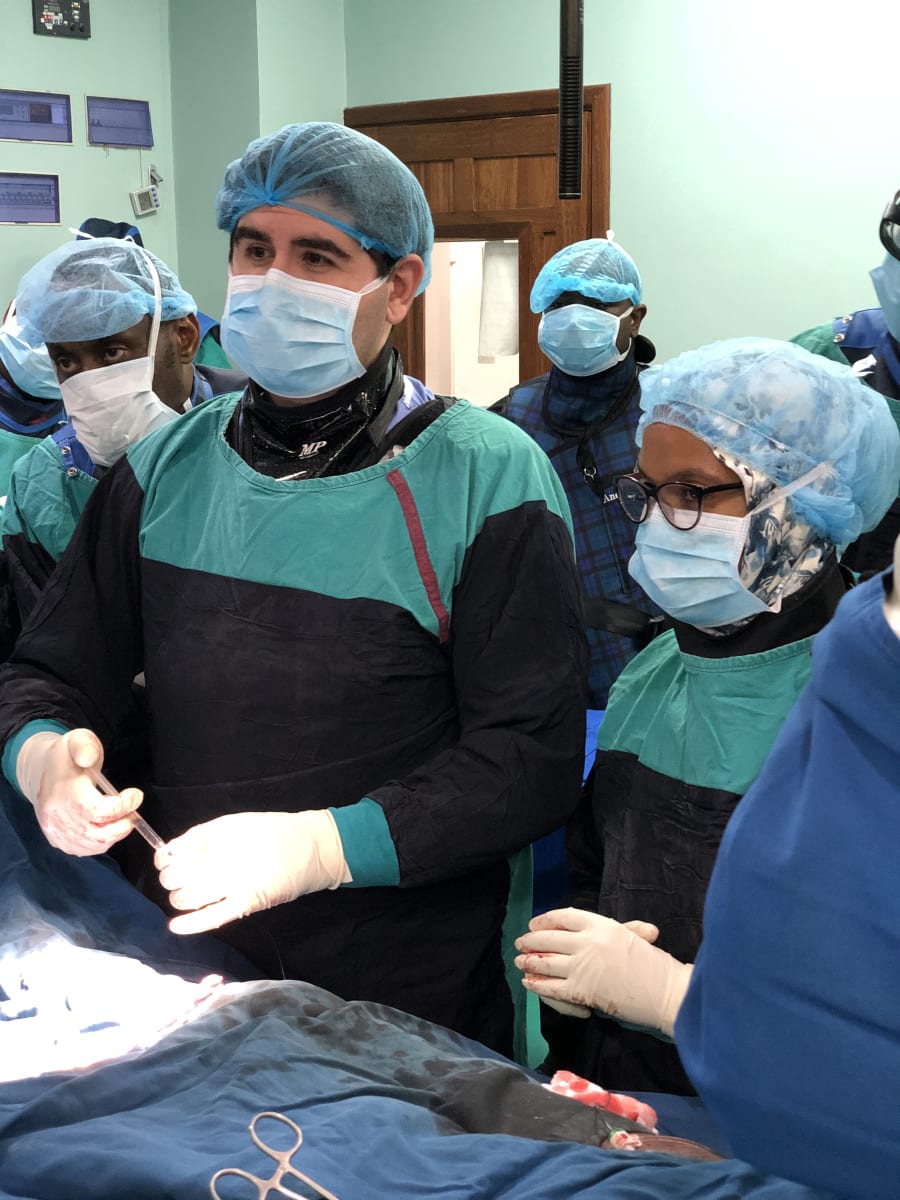
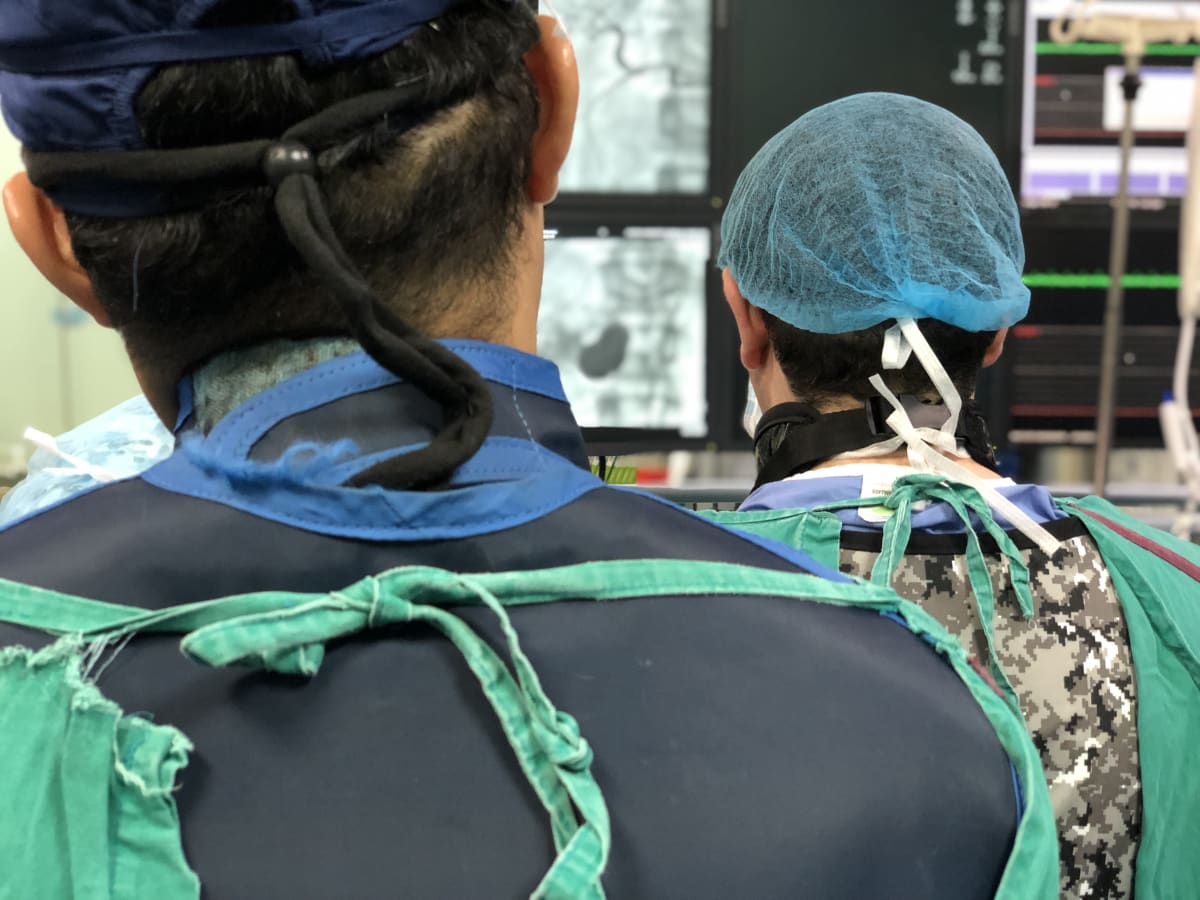

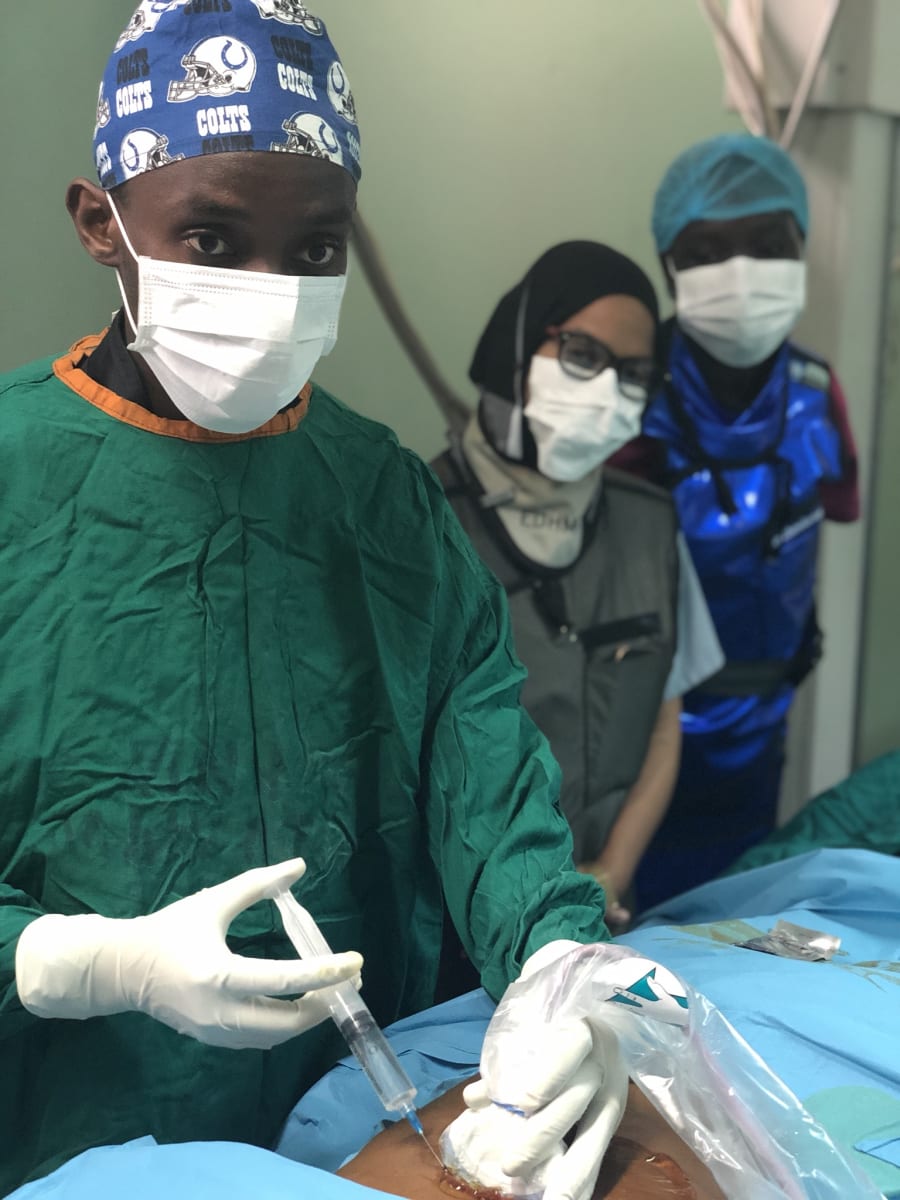
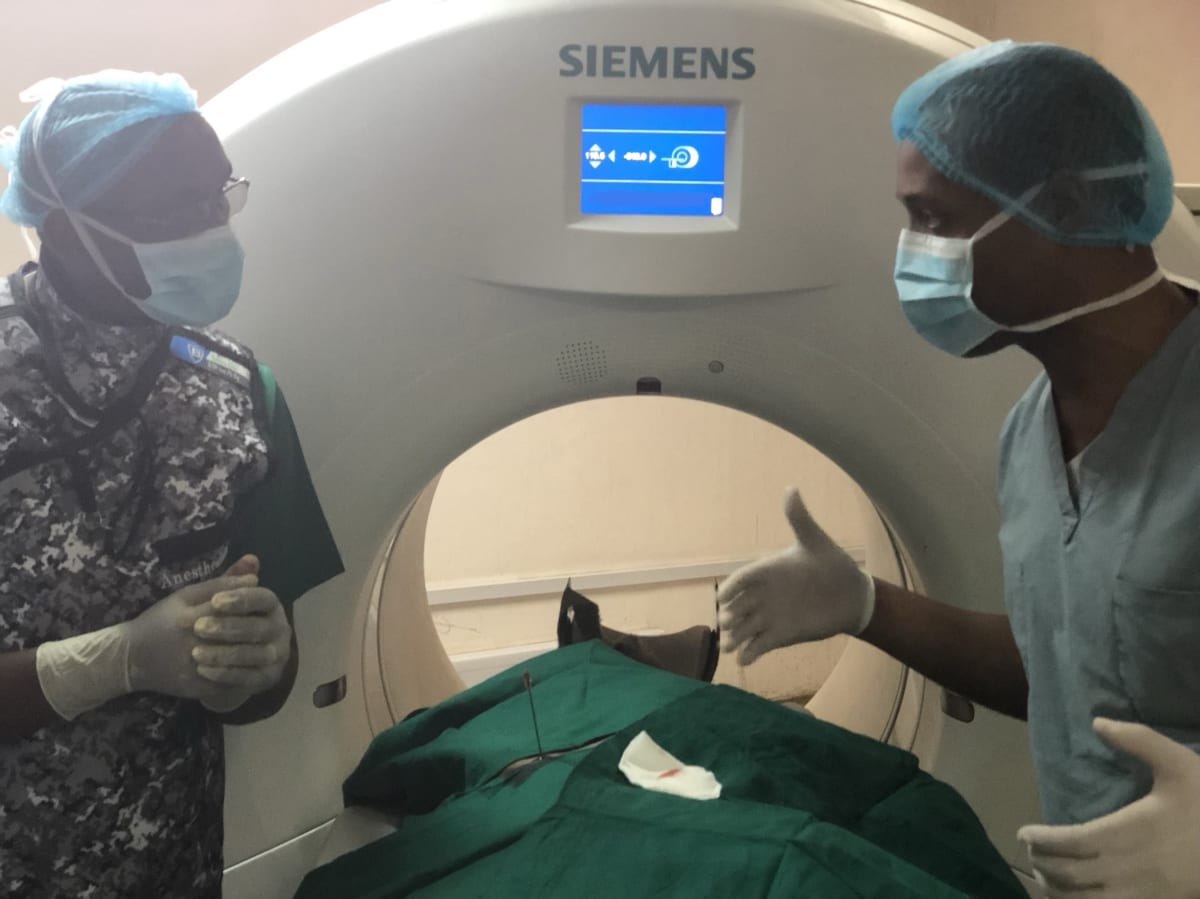



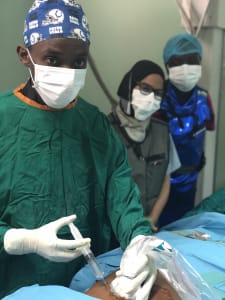
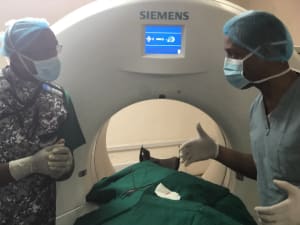
This trip was amazing! The people of Dar es Salaam were so welcoming, friendly and very appreciative of the help that we aimed to offer. We worked closely with the radiology department at the Muhimbili National Hospital, teaching the IR residents many of the simple procedures that are commonly done in the USA, that were previously unavailable in Tanzania. By training the residents to be interventional radiologists, they learned how to perform procedures such as nephrostomy tube placement, percutaneous biliary drain placement/decompression, percutaneous abscess drainage and CT-guided biopsy, among other procedures. Many of the common pathologies that we routinely see/treat in US patients were the cause of morbidity and mortality in Tanzania, due to the lack of healthcare access, specifically minimally invasive procedures performed by an interventional radiologist. For example, patients would die of renal failure secondary to urinary obstruction; and a simple “fix” such as a percutaneous nephrostomy tube placement was not available. Our trip allowed us to continue educating the radiology residents both in interventional and diagnostic techniques to provide cheaper, faster and safer care to their patient population. Care that was once only dreamed of.