I plan to provide human labor support and contribute to clinical care and capacity-building efforts working alongside Malawian residents, medical students, and other trainees at Mangochi District Hospital. The experience will entail working in both inpatient and outpatient settings for 4 weeks from 12/08/25 through 01/02/26. This trip is organized by a partnership between Providence Global and Domestic Engagement and Kamuzu University of Health Sciences in Malawi. This site is chosen because of an expressed need from the ministry of health and the college of medicine in Malawi to provide human resource support for this under-resourced district hospital that serves over 1.5 million people. Under the guidance of Malawian faculty and Providence mentors, I hope to help fill service delivery gaps in this community while learning to practice medicine with creativity and adaptability in the absence of advanced diagnostics and interventions. I intend to support Malawian-led quality improvement initiatives and provide clinical support for the Malawian residents and other trainees through daily ward collaboration, case write-ups, and presentations. I hope to build relationships that strengthen the training environment for Malawian learners, offering peer-to-peer exchange that is mutually enriching. By modeling comprehensive, integrated family medicine, I hope to support the broader goal of systems development that prioritizes prevention and community health. This experience will provide immediate human resource support to an overburdened health system, while also investing in the long-term capacity of Malawian clinicians and trainees.
The direct effect of this project will be to reduce the workload on the over-burdened and understaffed Malawian clinicians by providing human labor support. In turn, this will subsequently positively impact the patients and families served by Mangochi District Hospital. This population faces significant barriers to care, namely limited financial resources, shortages of trained providers, and systemic inequities that perpetuate cycles of illness and poverty. By contributing to direct patient care under supervision, I will help fill service delivery gaps and ensure that individuals in immediate need receive timely and compassionate care. Equally important, the Malawian learners that I will work with will benefit from collegial peer exchange and case-based teaching. Strengthening the training environment is a priority of this program, and by supporting learners as they develop their clinical and leadership skills, the project invests in the long-term capacity of Mangochi’s health system. These trainees are the future of family medicine in the community, and by contributing toward building their skills, we support a sustainable path toward better health outcomes.
I expect two primary results of this project: immediate contributions to patient care and, more importantly, hopefully a longer-term strengthening of Mangochi’s health system via the continued development of their future healthcare practitioners. In the short term, by supporting clinical care, I will help fill gaps in service delivery. In the long term, the project’s impact lies in its focus on capacity building. By sharing knowledge, modeling family medicine’s principles of holistic, community-centered care, and engaging in peer-to-peer collaboration, I hope the impacts of the project will continue even after my rotation ends. These efforts will hopefully provide patients comprehensive care while also investing in the growth of future family physicians. As with many global health projects, I fear that the short duration of my individual project lasting only 4 weeks may limit the utility of my efforts. However, I am reassured specifically by this project as the partnership between Providence Global and Domestic Engagement and Kamuzu University of Health Sciences has been present for years and ensures that this project continues to support local Mangochi providers after my departure from the country. In fact, the partnership has even led to a bidirectional exchange with Malawian residents coming to the United States and rotating at a Providence-based hospital in Washington in order to expand their clinical development. Global health is a slow and iterative process, so this long-term collaboration provides positive downstream effects that far outlast the individual impacts of any single person.




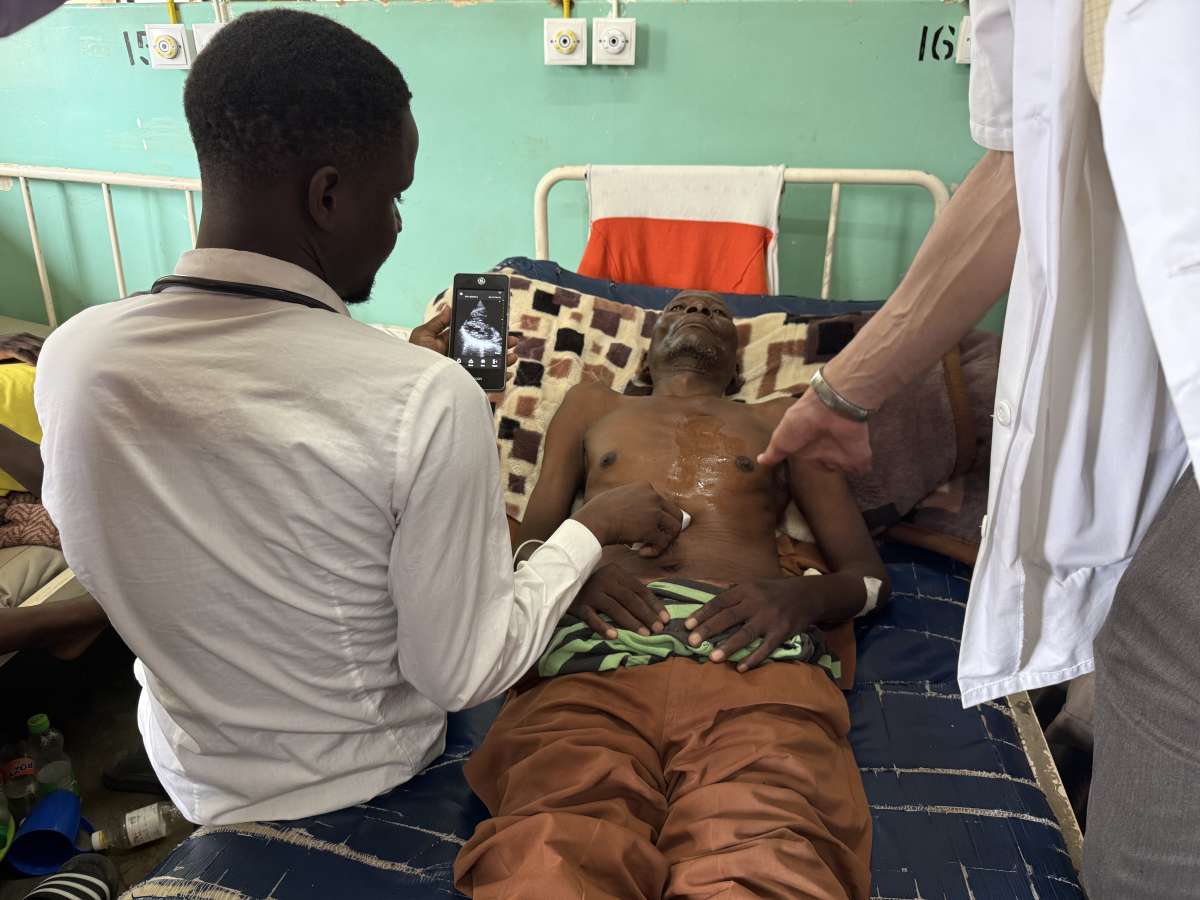






My month-long global health rotation at Mangochi District Hospital in Malawi was an incredible experience. As is often the case with global health work, the experience was mutually beneficial for the Malawian medical providers I came to support as well as for myself. The Ministry of Health of Malawi has recognized the need and value of training family physicians to meet the medical needs of their population. So, starting in September 2014, a partnership with Swedish Family Medicine, Kamuzu University of Health Sciences in Malawi, and SEED Global Health was formed to create family medicine residency training sites throughout Malawi, now with a steady flow of Malawian family medicine physician graduates each year. My role while at Mangochi District Hospital was to help support the training of the family medicine resident physicians (known as registrars) in an advisory role, as well as mentor the clinical officer (equivalent of advanced practice provider in the United States) interns and students, especially as the clinical officers are currently the primary medical providers of the rural district hospitals like Mangochi. The goal of this support and mentoring is for capacity building of the medical providers within Malawi, and may even perhaps have the potential to create a model of family medicine training development that can be modeled by other developing nations. That being said, the challenges are still formidable. I shared and aided in working through the diagnostic uncertainty that the clinical officers faced daily in many situations due to a lack or limited availability of diagnostic investigations, as simple as electrolyte levels to more advanced modalities like CT or MRI imaging. I helped teach clinical officers basic use of Point of Care Ultrasound (POCUS) to aid in diagnostic certainty as well as therapeutic interventions like thoracentesis or paracentesis. I shared in the mourning of loved ones lost to a preventable illness complication. I also shared in the joys of patients who were initially seemingly on the brink of death, but then significantly improved back to their baseline after the hard work of their clinical officer providers to accurately diagnose and treat the root cause of their illness, rather than just their symptoms. Although my time in Mangochi ended after only one month, I am encouraged by the longitudinal nature of the partnership to develop more family medicine physicians in Malawi, as I know this program will continue to bear fruit long after my time in the country.