During my clinical rotation in Kigali, Rwanda, I will have the opportunity to contribute to the continued development of an emergency medicine (EM) curriculum at the teaching and multi-specialty quaternary hospital, King Faisal Hospital. Working closely with local physicians and educators, and drawing from my own experiences as a senior emergency medicine resident at Massachusetts General Hospital and Brigham and Women’s Hospital in Boston, Massachusetts, I will assist with designing learning objectives, identify gaps in the current training, and support the creation of educational materials tailored to the country’s cultural norms and beliefs.
My work will involve observing clinical practices in the Emergency Department to better understand local workflows, resource limitations, and common case presentations. I will participate in case discussions, bedside teaching, and feedback sessions with Rwandan medical students and residents. This will allow me to align educational content with both the clinical realities on the ground and the broader goals of emergency care in a low-resource setting. Lastly, I will help to develop simulation-based learning modules and interactive case scenarios for common emergency conditions, including trauma, sepsis, and obstetric emergencies.
This experience will deepen my understanding of global health, medical education, and the importance of context-driven curriculum design. It will also strengthen my skills in cross-cultural communication, collaboration, and ability to adapt educational tools to meet diverse healthcare needs. Overall, contributing to the long-term goal of building sustainable emergency medicine capacity in Rwanda will be both professionally and personally meaningful.
During my clinical rotation in Kigali, I will work with the diverse patient population served by King Faisal Hospital, the largest referral hospital in the country. Many of their patients come from urban and peri-urban areas, while others travel from rural regions to access emergency care. I anticipate seeing cases that reflect a wide spectrum of health challenges, including trauma, infectious diseases, chronic conditions, and maternal health emergencies. Underlying many of these clinical presentations will be structural barriers—such as poverty, limited access to primary care, and resource constraints—that continue to shape Rwanda’s healthcare landscape.
The population served is also deeply shaped by the legacy of the 1994 Genocide Against the Tutsi, which resulted in the deaths of over 800,000 people and devastated Rwanda’s social, economic, and healthcare systems. In the aftermath, the country faced an acute shortage of healthcare professionals, the collapse of medical education infrastructure, and the destruction of physical facilities. Many survivors still face long-term physical and psychological consequences, including post-traumatic stress, untreated injuries, and generational trauma that influences care-seeking behaviors and trust in the medical system.
Despite these challenges, Rwanda has made remarkable progress in rebuilding its healthcare system through a strong emphasis on equity, community-based care, and workforce development. Understanding this history is essential to providing compassionate, context-aware care and provides me with a deeper appreciation for the role of medicine in healing not only individuals, but entire communities. I am excited to contribute to emergency medicine education in this context and further the country’s commitment to transforming its health system.
This experience is expected to have both immediate and long-term impacts on Rwanda’s healthcare system, as well as on my own development as a physician. By contributing to the design of a context-appropriate emergency medicine (EM) curriculum, I will support efforts to strengthen clinical training and improve the quality of acute care delivery in Kigali. As emergency medicine is a developing specialty in Rwanda, creating structured educational pathways helps build a more resilient, skilled workforce capable of responding to the country’s growing burden of trauma, communicable diseases, and maternal emergencies.
A sustainable EM curriculum can have a direct impact on patient outcomes by improving diagnostic accuracy, streamlining triage and management, and equipping healthcare providers with the tools to make critical decisions in resource-limited settings. Over time, this contributes to reducing preventable morbidity and mortality, particularly in underserved populations. By supporting local ownership and alignment with national health goals, I am hopeful that the curriculum will reinforce the infrastructure for emergency care training in Rwanda.
Professionally, this experience will expand my understanding of global health systems, curriculum development, and the ethical practice of medicine in cross-cultural environments. I look forward to gaining valuable skills in educational design, interprofessional collaboration, and systems thinking. Working alongside Rwandan clinicians will deepen my appreciation for adaptability, humility, and equity in healthcare delivery. These lessons will continue to shape my career, particularly my interests in academic medicine, health systems strengthening, and working to reduce health disparities at both local and global levels.


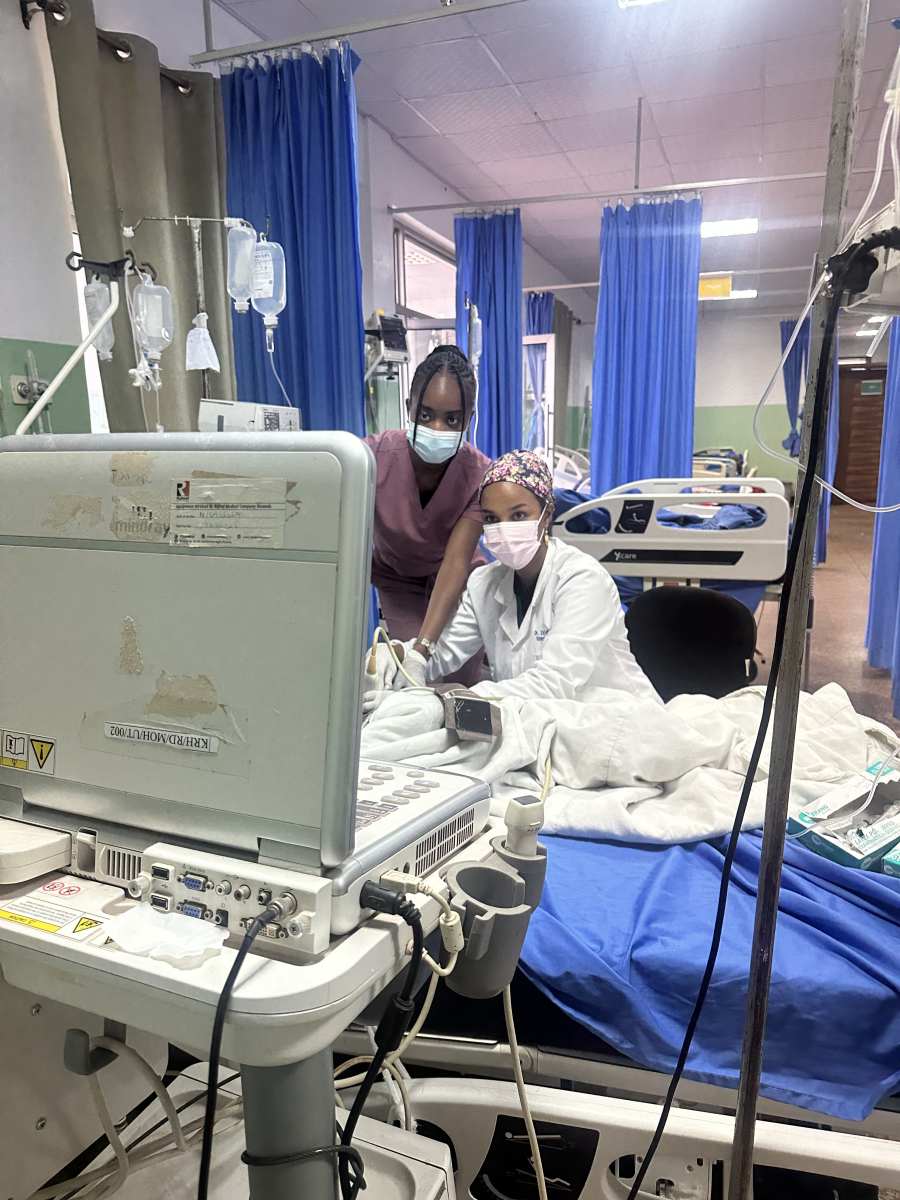



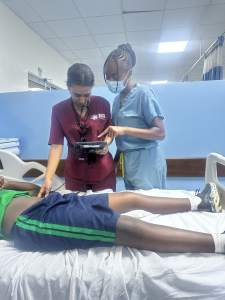




During my time in Rwanda, I had the privilege of working alongside the emergency medicine residents to teach point-of-care ultrasound at the bedside. We often engaged in thoughtful discussions on how to incorporate ultrasound to make rapid clinical decisions, as access to advanced imaging could sometimes be limited. Additionally, we came up with strategies on how to develop broad differential diagnoses, with special attention to infectious diseases that are less prevalent in the United States. I also delivered a lecture on traumatic orthopedic injuries with consideration on how to stabilize such injuries with limited resources.
As part of my experience, I split my time between three different hospitals across the country, which gave me a broader perspective on healthcare delivery in Rwanda. In particular, I gained insight into the differences between urban and rural medicine in the country. Observing this contrast deepened my appreciation for context-driven medicine and reinforced the importance of tailoring teaching to local realities. Ultimately, my time in Rwanda was one of the most meaningful experiences of my training and career. It strengthened my commitment to global health partnerships and I am grateful to Doximity for helping me realize this experience.