As a resident physician participating in the UNC Global Anesthesia Program at Kamuzu Central Hospital (KCH) in Lilongwe, Malawi, I will serve as a clinical supervisor and educator for the region’s anesthesia providers. These providers, called “Anesthesia Clinical Officers” (ACOs), are part of the local initiative to address an anesthesia provider shortage in the region. Since 2014, UNC’s Global Anesthesia Program has had a long-standing partnership with the KCH ACO group. This partnership focuses on advancing their medical education and improving their anesthesia care in low-resource settings to create a lasting positive impact on the region.
The primary beneficiaries of my project will be the ACOs at KCH in Malawi, and by extension, the patients that they go off to serve. This population was chosen because Malawi faces a severe shortage of trained anesthesia providers, with approximately only five physician anesthesiologists in a nation of over 21 million people. As a result, ACOs play an essential role within the Malawian healthcare system to fill the anesthesia gaps needed for surgical patients. ACOs are mid-level healthcare practitioners who undergo specialized training in anesthesia and deliver majority of anesthesia services in smaller district and regional hospitals.
By investing in the education of the ACOs at Kamuzu Central Hospital, this program contributes to a long-term impact of creating a stronger, more self-sufficient anesthesia workforce for the people of Malawi. The ACOs will learn clinical knowledge and technical skills that they can take to continue to train others, ultimately expanding access to surgical care for Malawi’s underserved population.
The lessons I gain from this experience will also carry forward into my own career. After residency, I plan to pursue a fellowship in Pain Medicine, a field defined by its sensitive nature and a patient population that often feels unheard. Pain Medicine, much like anesthesia in low-resource settings, demands empathy, adaptability, and creative problem-solving in the face of limitation. Ultimately, this program will not only allow me to contribute to global health equity but also help shape me into the anesthesiologist I aspire to be - one who can deliver high-quality care in any environment, regardless of resources, and who approaches every patient with compassion and empathy.




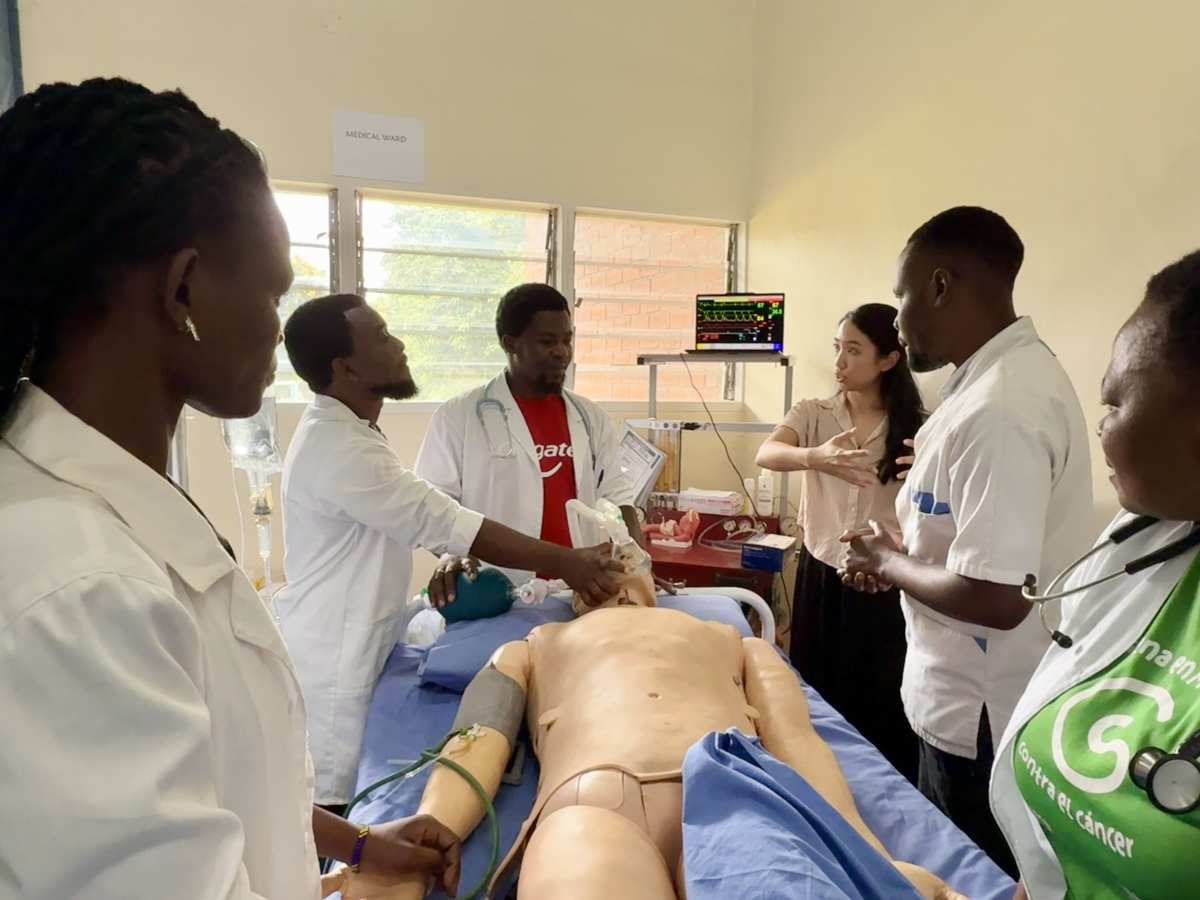







My time in Malawi was focused on supporting anesthesia education in a country with a critical shortage of anesthesia providers. I had the opportunity to teach a class of 17 anesthesia clinical officers (dedicated positions in Malawi to fill the anesthesia workforce gap). Through lectures, clinical teaching, and hands-on simulations, we focused on building practical skills and strengthening clinical decision-making in resource-limited settings. Working with such motivated learners was inspiring, and it reinforced how education and local training programs are essential to expanding safe anesthesia care throughout Malawi.