There are 4 domains to this medical mission which is primarily focused on building capacity to reduce maternal and infant mortality in Sierra Leone where approximately 10% of childbirths result in the death of the mother and/or newborn. Reducing this mortality is a major focus for the Ministry of Health in SL. Helping Children Worldwide (HCW, an NGO) has been sponsoring an annual conference to train midwives to address this need. Dr. Taylor was a course trainer for the 2025 conference but also was instrumental in setting up a sickle cell clinic at Mercy Hospital in Bo (a hospital sponsored by HCW) during that trip. Dr. Taylor has recently joined the board of directors of HCW Goals for this mission trip: 1. Teach in Essential Newborn Care WHO course for midwives (annual conference) at Magburaka Hospital, Magburaka. 2. Staff sickle cell clinic at Mercy Hospital in Bo (est. 2025 after my 2025 visit). I will aid in implementing sickle cell diagnostics, treatment, and sustainable clinic budgeting. I will be traveling with a donated diagnostic instrument solicited from a biotech company. 3. Meet with Minister of Health Demby RE: courses and briefing on sickle cell disease [follow-up to prior meeting Jan. 2025]. Dr. Demby is well known to the Howard University administration, and my role at Howard can amplify the objectives of this mission with the MOH. 4. Provide on site supervision of the activities of Helping Children Worldwide and at Mercy Hospital as a volunteer member of the Board of Directors. In summary, the primary purpose of this mission is focused on reducing maternal and infant mortality by training midwives in life saving interventions in the delivery room. In parallel, my expertise in sickle cell disease has led to a new initiative in a country where there is typically no care for this common genetic disease.
Involvement in the WHO course designed to reduce maternal and infant mortality will benefit the people of Sierra Leone by building local capacity. The population of Bo, Sierra Leone’s third largest city, is already benefiting from the sickle cell program established in 2025. Like the WHO course, I am building local capacity by training physicians in treatment of patients with sickle cell disease. Sickle cell disease is an order of magnitude more common in Africa with an estimated 1.5% of the population affected by the disease. At least 20% of the population are carriers of sickle cell trait and are at risk for having children with disease. Historically, this society was destroyed by a civil war in SL that lasted until 2002. I became engaged with Helping Children Worldwide in 2019 through the United Methodist Church. Since that time, I have hosted physicians from Mercy Hospital at Howard University for training in SCD. It was not until 2025 that HCW approached me about participating in onsite courses and as a volunteer on the Board of Directors. This mission will strengthen my personal connections with staff members at Mercy Hospital. The choice of Sierra Leone is through this opportunity. However, 25% of the SCD patients in Washington DC are foreign born with SL representing 1 of the top 4 countries of origin for these patients. The interactions with the Ministry of Health in SL are similarly aligned with my role as Director of the Center for Sickle Cell Disease at Howard University, and this trip will benefit the university mission to serve the undeserved.
The expected impact of the WHO maternal and infant mortality training conference is to produce a large group of midwives with the skills to save lives in the delivery room in a low resource environment. Helping Children Worldwide monitors the effectiveness of this program through survey instruments for participants and health outcomes in the hospitals of course participants. The impact of the SCD clinic in Bo is that it has already provided hope to parents of children with sickle cell disease as there has been no screening program or treatment available until this year. After I return, I will carry lessons learned in sickle cell disease to other international outreach efforts for SCD that I spearhead through Howard University. I have already introduced the SL Mercy Hospital team to my sickle cell hematology colleagues in the Republic of Congo (Brazzaville) in the hopes that they will benefit from shared clinical experience. I am also considering proposing a research project for my colleagues in SL as maternal mortality is up to 60 times greater in pregnant women with sickle cell disease. I hypothesize that pregnancy in women with SCD could be a significant factor contributing to the high maternal/infant mortality in Sierra Leone. Further study could answer this question.

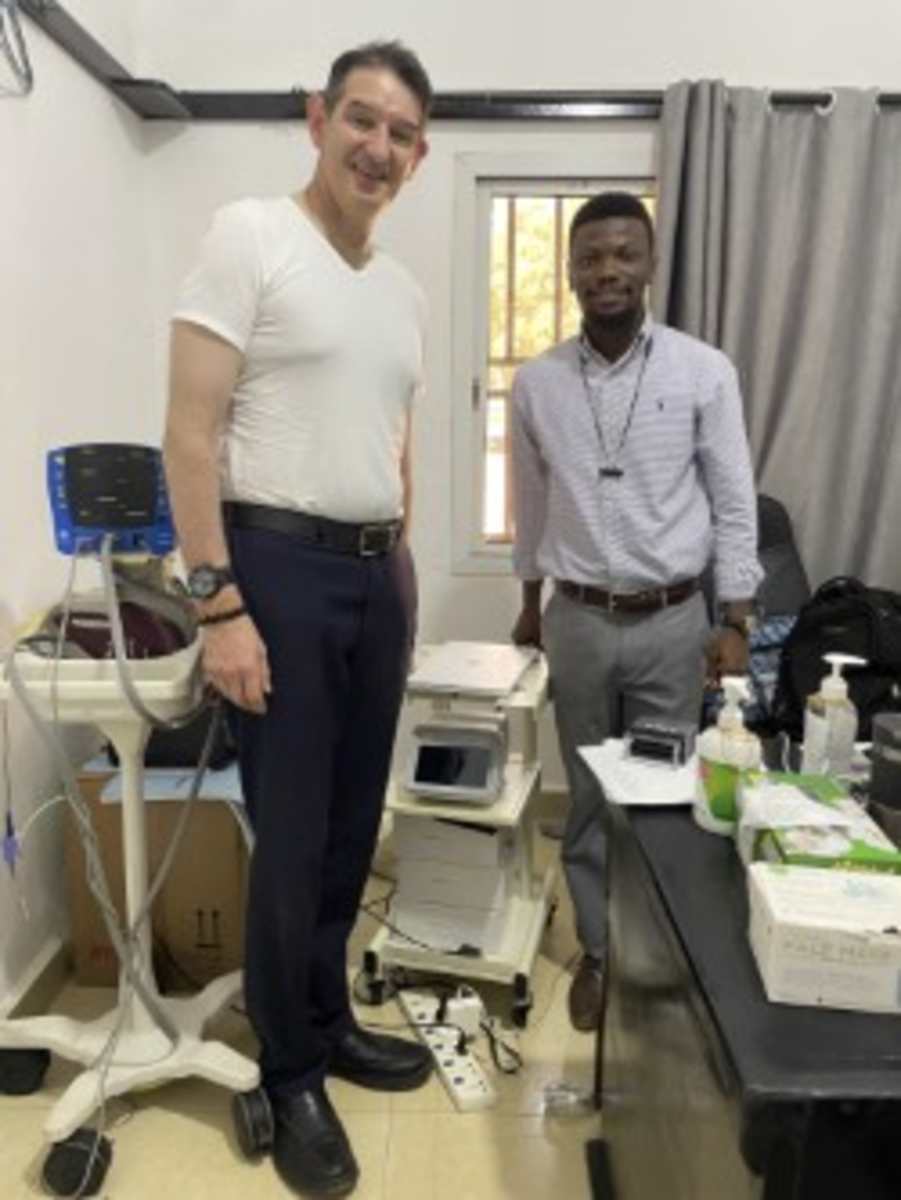





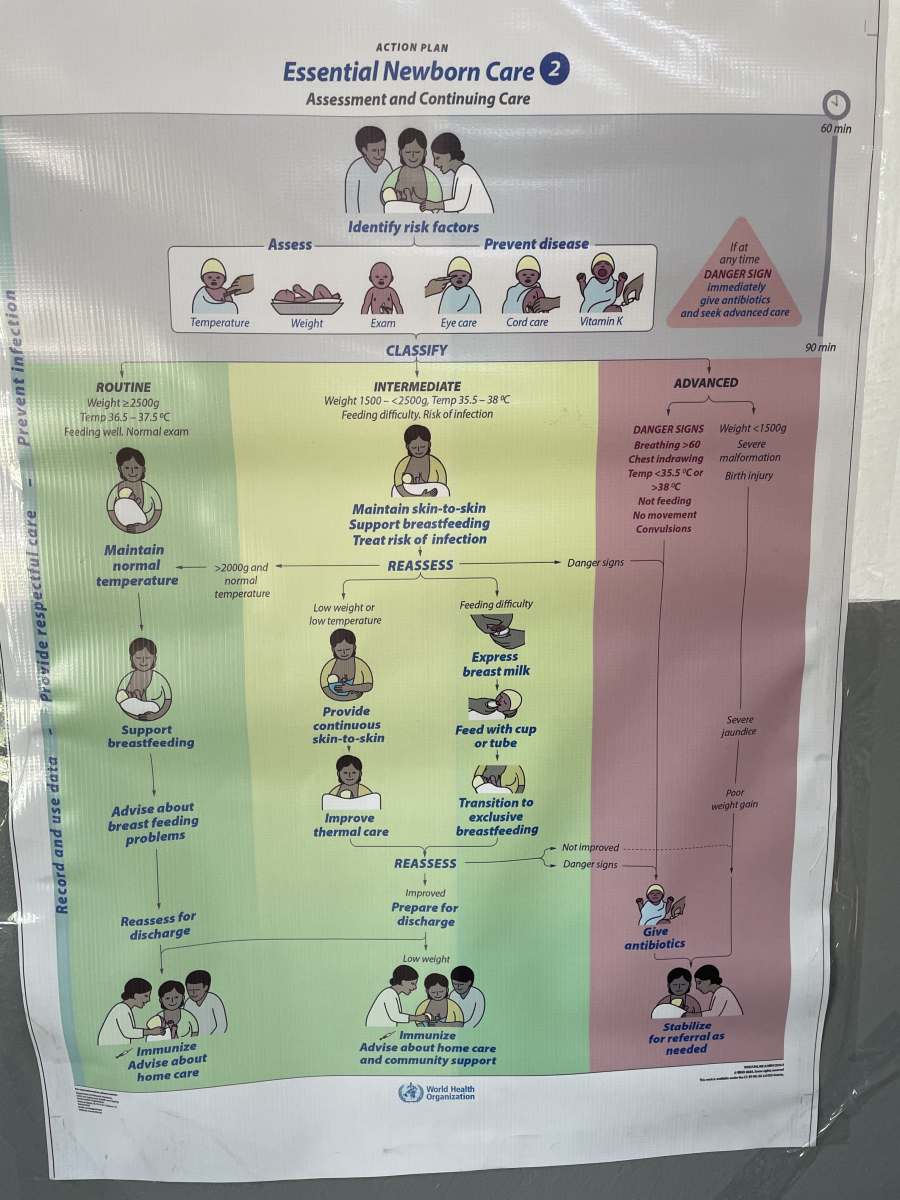














Traveled to Makeni Sierra Leone and taught a course on Essential Newborn Care (modified NALS) to RN-midwives at the Magburka District Hospital. Course designed to reduce infant and maternal mortality during childbirth as this is the #1 public health issue in SL. Maternal mortality rate is 717 deaths/100,000 live birth and Infant Mortality Rate is 75 deaths/1000 live births (per the SL Ministry of Health when I visited Minister Demby in 2025). Faculty is a mix of Americans and local trainers in SL - we have been working together for a few yrs. Highlight was having a student from 2025 course become a rising trainer on the faculty. I also spent time with my co-faculty member Banneh Daramy. She is pictured with me wearing a Howard University Center for Sickle Cell Disease t-shirt. All of the students are nurse-midwives from across SL who will return to their district hospitals to improve the quality of care during childbirth. The students are always eager to learn and have a lot of book knowledge combined with practical hands on training in neonatal bag mask ventilation. I always emphasize the need for muscle memory for our students which means that they must perform bag mask ventilation 1500 times before the skill is rote memory. The course always ends with traditional music to celebrate the end of hard work and a lot of learning.
Then I made a trip to the Wesleyan Hospital in Kamakwie (north near the Guinea border) to tour the hospital and discuss possibility of a sickle cell program there. This was a long drive on rough roads with the highlight of the trip crossing a river via a bridge that had washed out in a storm several years ago. Wesleyan Hospital has 2 missionary physicians who on their first trips to Africa. I also toured their living quarters for students or other visitors. Perhaps someday, medical students from Howard University will be able to spend a month there learning about medicine in low resource environments.
I then drove to Bo to visit Mercy Hospital to visit Dr. Morie Vandi who has started SL's 3rd sickle cell clinic. I delivered a Hemex Gazelle diagnostic system to Mercy Hospital courtesy of Hemex to allow Dr. Vandie to make a sickle cell diagnosis. Dr. Vandie established this clinic in 2025 about 6 months after we held a meeting about SCD at Mercy Hospital in Bo. Thanks fundraising by Helping Children Worldwide and the Healey International Relief Foundation, children treated in this clinic receive care free of charge. I also toured Mercy Hospital (my 2nd visit there) as I have also recently joined the board of directors for Helping Children Worldwide which sponsors Mercy Hospital (since the end of the SL civil war 25 years ago).
I then drove back to the airport for the trip home confident that I was able to help train a new set of nurse mid-wives in Essential Newborn Care AND that I was able to use my hematology knowledge to further help Mercy Hospital to develop their new sickle cell disease clinic. Special thanks to the Dox Foundation for their assistance with this trip