Background
Since 2011, Drs. Ann Markes and Matthew Kane have been going to Uganda, specializing in maternal and newborn care through training of WHO-supported curricula. In 2023, the medical program became an independent organization, Well On their Way (WOtW), committed to training frontline providers in lifesaving obstetric and neonatal skills.
Executive Committee:
• Megan Carmel MD – Medical Director
• Matthew Kane MD – Financial Director
• Dr. Ann Markes MD – Executive Director
To date, WOtW has trained 100+ healthcare workers at 26 health centers, serving ~135,000 residents (6,000 pregnancies annually). Facility deliveries remain around 50%.
Program Expansion
1. Village Health Team (VHT) Training
In 2025, WOtW received an iCATCH grant from the American Academy of Pediatrics to train 180 VHTs annually (2025–2028) using Uganda’s “Wheel of Good Practices” curriculum.
Focus areas:
• Promoting facility deliveries
• Prenatal/postnatal education
• Immunization awareness
• Addressing barriers to healthcare access
During the 2026 visit, WOtW will:
• Gather feedback from VHTs and Health Assistants
• Review successes and challenges
• Evaluate early data to refine Years 2–3 training
2. Obstetric Ultrasound Training
In June 2025, WOtW received $28,000 in private donations to launch an ultrasound training initiative, aligning with WHO’s recommendation for at least one early pregnancy scan.
Program Overview
• 10 midwives will complete an online course and a two-week hands-on course.
• 5 Lumify portable ultrasound units will be provided for ongoing use in rural clinics.
• Training led by a skilled sonography team, with oversight from WOtW’s executive team and Gulu specialists.
Sustainability & Quality Assurance
• Continued mentorship and remote image review
• Integration of ultrasound into routine antenatal care
Gulu District, located in northern Uganda, has a population of approximately 130,000 people. The district was deeply affected by the 20-year conflict between the Lord’s Resistance Army (LRA) and the Government of Uganda, during which the majority of residents were displaced into Internally Displaced Persons (IDP) camps. The prolonged conflict severely disrupted community structures, eroded traditional support systems, and left a legacy of physical, psychological, and socioeconomic trauma.
Although stability has returned, Gulu remains impoverished, and most families rely on subsistence farming. Health services are stretched across 156 villages covering about 1,300 square miles, connected largely by dirt roads.
Health services in Gulu District are provided through a network of facilities at varying levels of capacity:
• Level IV Health Center (1): District referral facility with inpatient, maternity, and surgical services.
• Level III Health Centers (8): Each has a delivery room and limited inpatient capacity.
• Level II Health Centers (16): Small rural units with 1–2 staff, offering basic outpatient and preventive care.
• Level I Health Centers: Community-based services delivered by Village Health Team members from their homes.
An estimated 6,250 pregnancies occur annually, yet only about 3,000 deliveries take place in health facilities. This means fewer than half of births are attended by skilled providers, while many home deliveries go unrecorded. Traditional birth attendants (TBAs), though banned from conducting deliveries under Ugandan law since 2013, continue to assist some births due to cultural familiarity and limited access to skilled care.
Gulu district currently has only one antiquated ultrasound machine and one trained ultrasonographer.
Strengthening community-level engagement and enhancing the capacity of health workers are critical toward ensuring that every mother and newborn has access to skilled care.
Expected Outcomes and Sustainability
Ultrasound Training
Expected Outcomes:
• Capacity Building: 10 midwives trained and able to independently perform basic obstetric ultrasounds.
• Access to Care: Increased availability of early pregnancy scanning services across Gulu District.
• Improved Health Outcomes: Earlier detection of complications leading to improved maternal and neonatal outcomes.
• Quality of Care: Enhanced diagnostic accuracy and confidence among midwives during antenatal care assessments.
Sustainability:
• Integration into Routine Care: Ultrasound services will be embedded into standard antenatal care at health facilities and outreach clinics.
• Local Ownership: Equipment will be maintained locally by trained staff, ensuring continued functionality.
• Ongoing Professional Development: Continued skills improvement through collaboration with local ultrasound professionals and periodic remote mentorship and quality assurance reviews.
• System Strengthening: Development of local expertise will reduce reliance on external trainers.
Village Health Team (VHT) Training
Expected Outcomes:
• Community Engagement: VHTs will effectively promote facility-based deliveries and educate families on prenatal and postnatal care.
• Health Behavior Change: Increased awareness and uptake of immunizations, as well as improved attendance at antenatal and postnatal visits.
• Early Detection and Referral: Improved identification and early referral of mothers and infants showing danger signs.
• Health Access Facilitation: VHTs will help families overcome social, economic, and logistical barriers to accessing care through the government health system.
Sustainability:
• Integration with Existing Systems: VHTs are already embedded within the community and the government health system, ensuring program continuity.
• Empowerment and Confidence: Enhanced knowledge and skills will boost VHT confidence in community engagement and strengthen their advisory role.















































Overview
Well On their Way – a healthy start for every mother and baby - is a small nonprofit organization committed to the health of mothers and babies in Gulu District, northern Uganda, through medical capacity building. Currently an organization of ten members, four American and six Ugandan, we have provided training in six Helping Babies Survive and Helping Mothers Survive curricula, with widespread implementation through a Trainer of Trainers model. Our goal is to have every nurse, clinical officer, and midwife, working within the Ministry of Health system in this rural agrarian underserved region, prepared to identify and provide early management for newborn and maternal complications and emergencies. This training has been sustained through annual refresher training.
We have just returned from the February 2026 site visit, which had two main emphases which built on the work we have been doing for over a decade: 1) Following up on a newly implemented program of Village Health Team training. 2) Introducing obstetric Point of Care Ultrasound.
Village Visits and Village Health Team training
In late 2025, with partial support from the ICATCH grant from the American Academy of Pediatrics, WOtW implemented training of Village Health Team members (VHTs). VHTs are volunteers elected by their villages. They are trusted, highly respected, but have very little formal medical training. Using a wonderful curriculum with pictorial explanations called Wheel of Good Practices, 180 VHTs were educated in topics of maternal/child health during a 2-day training period (six sessions, 30 VHTs). The goal of these training sessions was to have the VHTs in turn educate the families in their village about the importance of attending antenatal clinics, delivering in the health centers, and following up for postnatal care and immunizations. It is too early to accurately comment on these health care seeking behaviors, but early data tracking is showing positive trends - team members are optimistic!
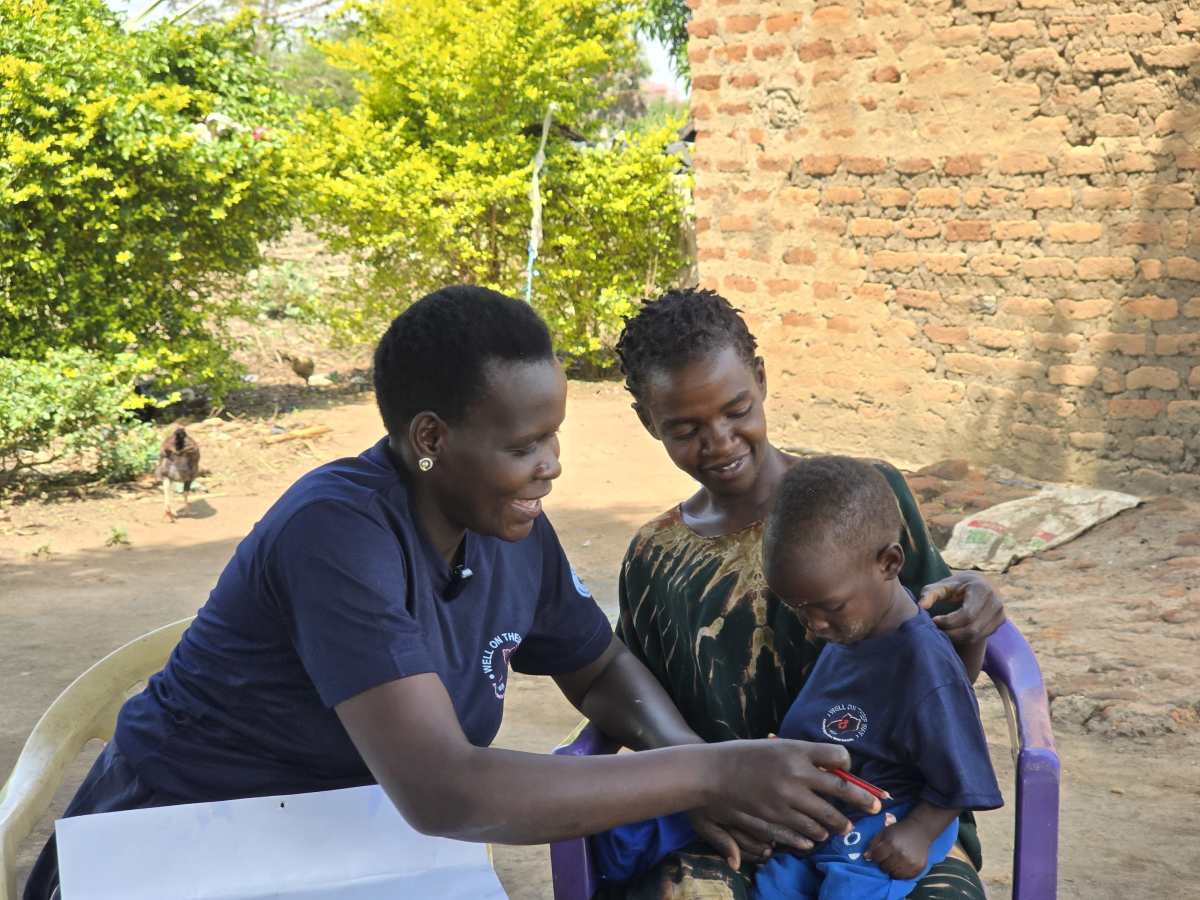
While on site, WOtW team members visited with VHTs in their homes, listening to the stories of the work they are doing and the impact of the training on their work. They took us to visit families in their village, demonstrating their teaching, and sharing stories of how they identified issues such as inadequate antenatal care and lack of immunizations and how they successfully counseled the mothers.
We also visited the homes of mothers who ran into complications such as pre-eclampsia and pre-term delivery, and talked about how they were successfully managed by WOtW trained nurses and midwives. It was so wonderful to be welcomed into these beautiful homesteads, to meet families, and to see so many healthy babies!
Last, we attended four VHT meetings, each attended by approximately 20 VHTs. We were honored to hear the stories of how their practices were impacted by the training they had received, to hear stories of their successes, and reports of their challenges such as walking long distances to visit their village members, road and path washouts due to rain, and the need for raincoats and boots. They requested that more VHTs be trained, which will lessen their workload and decrease the distance they must travel. We will try very hard to find the financial resources to accomplish this.
Obstetric POCUS training
A long-held dream of WOtW was able to be implemented during this visit thanks to a generous private donation AND to the travel support provided by the Doximity Foundation.
The program started months in advance of our onsite trip. Ten trainees (nine midwives and one clinical officer) were provided with two online courses, WPOCUS and GUSI, giving them essential knowledge. However, nothing replaces putting their hands on the probes and learning how to scan pregnant abdomens.
The onsite training started with didactic training, but quickly the learners were learning hands-on skills, initially with “phantoms” provided by Midwife Diana Dowdy, founder of WPOCUS, then with live models brought to the classroom, and most importantly, by traveling to multiple health centers in this very rural region, where pregnant mothers lined up to be scanned.
With less than two weeks available to provide this training, the training team focused on a few important skills:
• Confirming intrauterine pregnancy
• Identifying multiple gestation
• Estimating gestational age
o First trimester: Crown Rump Length
o Second/third trimester: Biparietal Diameter
• Assessing fetal heart rate
• Identifying placental location
• Identifying fetal position
• Assessing amniotic fluid
Typically WOtW volunteers pay their own travel expenses. When Dr. Meg Carmel (obstetrician/gynecologist), Dr. Matt Kane, and I learned that our airfare was going to be covered by Doximity Foundation, we donated an equal amount back to WOtW, using those funds to cover the travel expenses of three obstetric sonographers with years of experience. Amy Scheible, Jade Lavender and Raeanne Watson, joined Diana and Meg, resulting in a team of five trainers, allowing an excellent trainer:trainee ration of 1:2. This was critical to our success over a short period of time.
Despite the short training time, many abnormalities were identified, including one woman with an abdominal ectopic pregnancy – she was referred urgently for surgery, and the access to ultrasound most likely saved her life. Placenta previa, absent or low amniotic fluid, and twin gestation were identified several times, and appropriate management/follow up arranged. Having this tool in the future will definitely make a difference to health of the mothers and babies in Gulu District.
The trainees were highly engaged and worked very hard. Some were able to acquire the skills more easily than others. This is where the longstanding relationship between the Ugandan and US WOtW team members makes our training model positioned for long term success. The more successful trainees will mentor those who are acquiring skills more slowly, until everyone is up to speed. They will be supervised locally by two local gynecologists, Dr. JJ Lapat and Dr. Joshusa Washa, based in Gulu City, who are willing to generously donate their time and expertise to support this program.
What did the training mean to our trainees? Here are the words of Midwife Emily Atimango: “I had a hard time relating to the online training due to little knowledge. But when the trainers came around it was more or less the best moment for me because it felt like my mind was opened with just a click or like a radio station was tuned to a proper channel.” Midwife Susan Apiyo said, “Before this training, many assessments during pregnancy relied mainly on physical examination and the mother’s clinical presentation. Learning how to use ultrasound has opened a new window that allows me to see what is happening inside the uterus more clearly. It helps in determining the fetal gestational age, presentation position and general well-being of the baby, and identifying any potential complications earlier than before.”