Prior to the trip, my responsibilities will include procuring licensing in the Philippines, assistance with fundraising, equipment-gathering, and packing supplies. During the trip, I will be planning the operating room schedule, operating as the resident surgeon on all cases, and training local operating room staff and nursing students for procedures performed/relevant perioperative care. This will be under the supervision of the senior surgeons, Dr. Christopher Klem and Dr. Kelly Anderson. This trip makes the most difference to patients with disfiguring salivary gland neoplasms that are aesthetically obvious and for patients with large goiters leading to compressive symptoms. The goals are to improve quality-of-life for these patients and diagnose any malignancies that need further treatment. It also provides the local hospital team with opportunities to learn how to take care of complex cases such as these. It will also make a difference in my own education, as an aspiring Head and Neck Oncologic surgeon starting a fellowship next year and as someone interested in providing global health services/education in my future. Learning about various medical infrastructure setups in other countries also helps to improve our own and foster ongoing community development. The trip additionally provides mentorship to teenagers considering the medical field for a career, as they have the opportunity to participate in the perioperative care, as well as observe the surgical procedures being completed.
The Aloha Medical Mission/Scholastic Sisters Bacolod sponsoring program hosting surgeons at Valladolid District Hospital targets medically underserved patients in Negros Occidental in the Philippines so that they can receive Otolaryngologic care, dental care, and general surgical care. The Otolaryngology/Head and Neck Surgery team screens and treats patients there with salivary and endocrine neoplasms over the course of two weeks. During this time, the Head and Neck team alone screens up to 60 patients and completes an average of 25 cases over a week and a half. The entire team (including dental and general surgery) screens 450 patients and operates on over 100 patients. This particular region of the Philippines is known for a high poverty incidence at nearly 25%, poor access to healthcare in addition to basic needs such as electricity, and medical burden to the system from agricultural work. Many of the population are sugar farm workers that otherwise do not have the means to pay for medical care and often have advanced disease at the time of presentation.
As stated, the expected impact is to provide needed care for patients living in this catchment area to improve their quality-of-life and ability to continue work and provide for their families. There would also be ongoing educational benefit by teaching local operating room staff about surgical instruments, surgical steps, and patient safety. Nursing students will be involved in the care of these patients, which will increase their educational yield and nursing experience overall.As medicine is a field of lifelong learning, it is also a field of lifelong teaching and building sustainable treatment algorithms, which I believe can be done on an impactful scale when abroad. As a chief resident now in Otolaryngology/Head and Neck Surgery and one continuing to Head and Neck Oncologic Surgery/Microvascular Reconstruction fellowship next year, this experience in the Philippines will advance my training and prepare me for my chosen career path. As a military physician, I can apply this experience to future deployment and even life outside of the military, as I hope to become further involved in global healthcare projects.
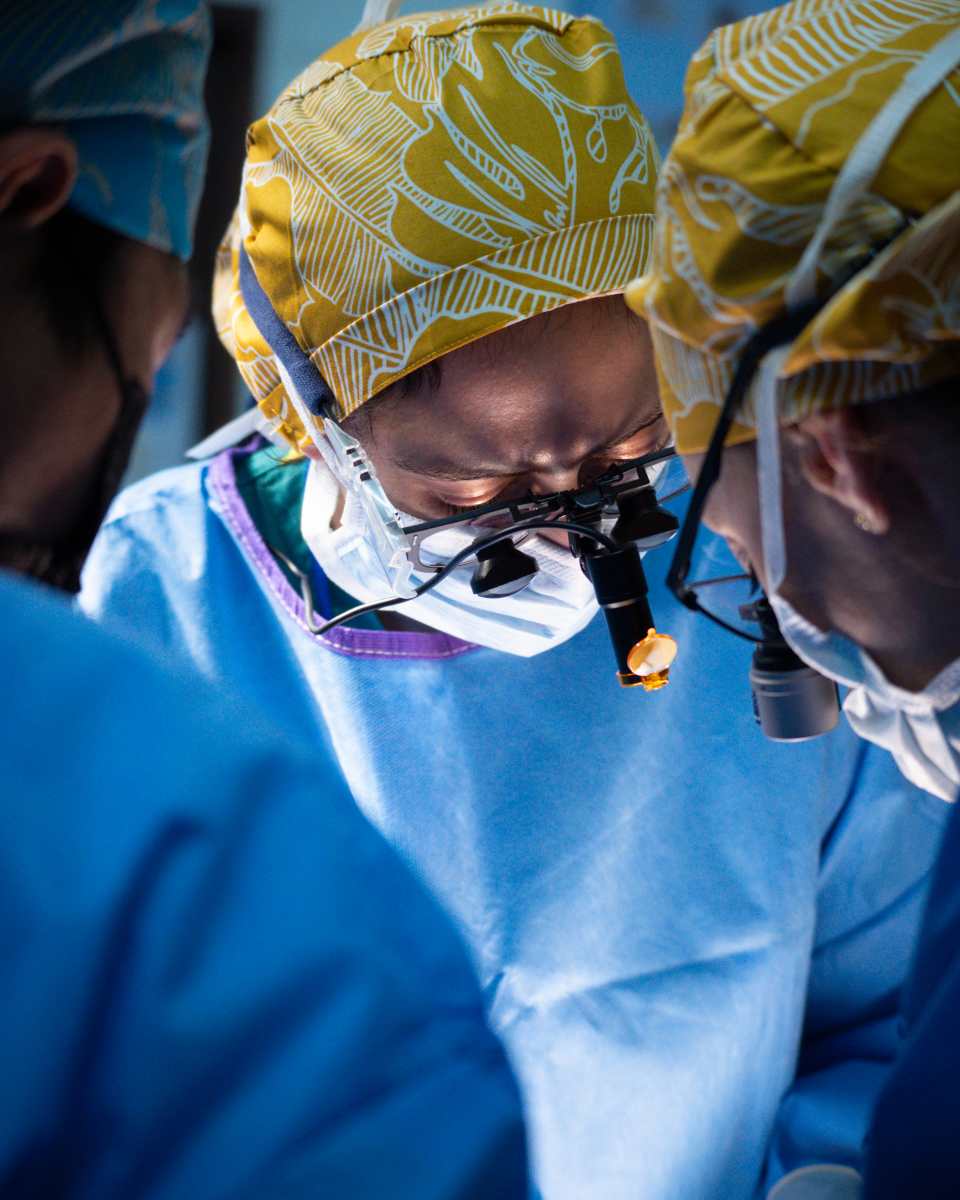


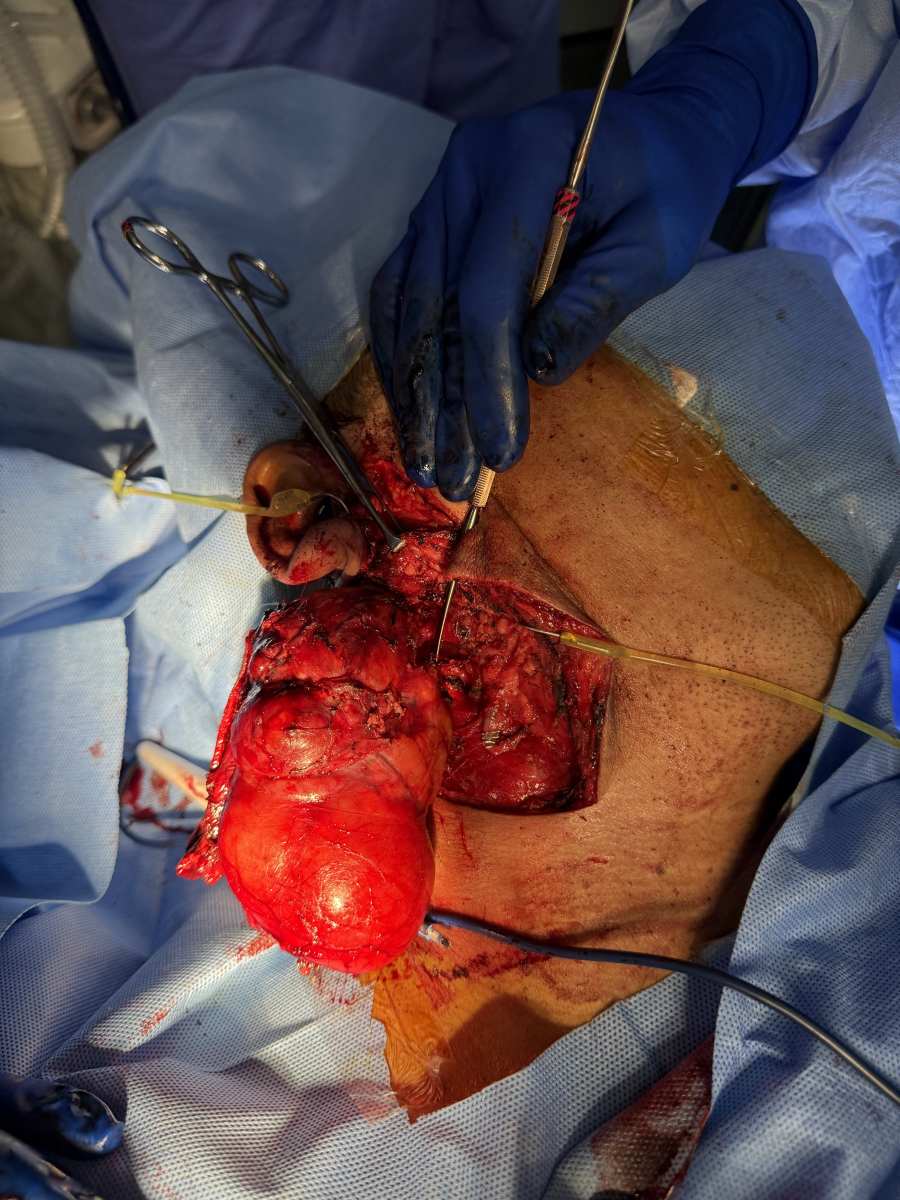




The head and neck division of this mission screened nearly 50 patients for thyroid surgery and salivary gland neoplasms. Ultimately, 28 patients underwent surgery over the course of 5 days. Their procedures were quality-of-life improving, subjectively. Many had perceptual disfigurement as a result of salivary gland masses or goiters. Many complained that it interfered with their daily labor jobs. Our mission included pediatric patients - some of the strongest children I have ever seen. The warm reception at Valladolid Hospital and the hospitality and gratitude of the staff and the patients were eye-opening and affirming of the impact our team carried. The medical mission was also a valuable experience in operating in low-resource environments and in learning the logistics of all parts of a medical mission. Our teams included nursing staff, local scrub technicians, local nurses, anesthesiologists, and nurse anesthetists. We admitted our patients pre-operatively and at least overnight to ensure clinical continuity and monitor for complications. Most patients were able to return home on postoperative day 1. The local nurses had the opportunity to scrub into cases with us and participate in learning on rounds. Overall, the mission not only impacted the patients we treated - instead, it fostered a broader scale of learning in a personal sense. It fostered development of the local nurses and built long-lasting relationships with the local teams supporting our effort. It encouraged multidisciplinary collaboration. I hope to participate in this effort for years to come. I take with me stories of resilience, perseverance, and gratitude.