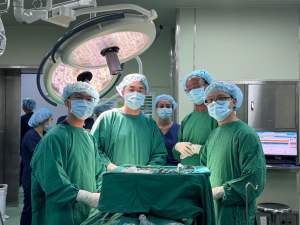
This trip is centered on sustainable change. Rather than a short-term mission model, our focus is on longitudinal relationships, education, mentorship, and skill exchange that will continue long after we leave. As a fourth-year plastic surgery resident currently dedicating a full year to research in craniofacial care at the University of Wisconsin, I am deeply committed to advancing both patient care and global surgical education. I will join a two-week capacity-building mission in Vietnam focused on complex craniofacial and microsurgical reconstruction. During the first week in Ho Chi Minh City at the National Hospital of Odonto Stomatology (NHOS) we will conduct screening clinics and deliver a week of lectures and operative cases on facial trauma, orthognathic surgery, mid-face advancement and distraction osteogenesis. In the second week in Hanoi, I will teach a microsurgery course alongside hand and breast reconstructive surgeons across multiple hospitals. My role will be both as educator and learner—teaching microsurgical techniques, rib and iliac crest harvests, and assisting in challenging cases, while learning how to deliver surgery in diverse resource environments and collaborating longitudinally with our Vietnamese partners. These partnerships are transformative. Each lecture, each dissection, and each shared case is an opportunity to expand what local teams can offer their communities—especially for children and adults who might otherwise go untreated due to complexity or cost. My contribution will be one small part of a collective effort to build a future in which Vietnamese surgeons have the tools, confidence, and community support to perform complex reconstructive and microsurgical procedures independently, sustainably, and with pride. The deeper impact lies in empowering local surgeons with the expertise to replicate and expand this care model, so that future generations can access life-changing surgery without reliance on outside teams.
We will serve both pediatric and adult patients in Vietnam who suffer from craniofacial deformities, traumatic injuries, and defects requiring reconstruction—conditions that profoundly affect function, appearance, and quality of life. Many of these patients lack access to specialized surgical care, particularly in complex craniofacial or microsurgical cases. As a result, these patients face functional challenges (e.g., airway, mastication, speech) and social stigma due to facial differences or untreated trauma. By combining direct surgical treatment with structured education, we aim to help these patients while simultaneously improving the capacity of their healthcare system to meet future needs. Additionally, the local Vietnamese surgeons, trainees, anesthesiologists and support staff are eager to expand their technical repertoire and take ownership of complex reconstructions in their communities.
The immediate outcomes of this trip will include successful surgical interventions for patients who might otherwise go without care, along with meaningful bidirectional teaching between our team and Vietnamese surgeons. The broader impact lies in its continuity—this trip is one of a series of ongoing collaborations between our institution and hospitals in Vietnam. These recurring exchanges build lasting relationships, reinforce previously taught skills, and track the progress of sustainable surgical capacity building over time.
By co-teaching the Hanoi microsurgery course, I will help strengthen the technical skill set of local surgeons and expand their ability to independently perform complex procedures. This shared experience fosters mentorship, confidence, and innovation, ensuring the impact endures long after our team departs. Through repeated engagement, these trips cultivate trust, shared expertise, and a collaborative network that grows stronger with each visit.
The expected outcome is not only immediate patient benefit but also the establishment of a self-sustaining microsurgery and craniofacial ecosystem in Vietnam—one where local surgeons have the training, resources, and partnerships to deliver world-class reconstructive care for generations to come.
This experience will also be profoundly formative for me as a trainee. Witnessing firsthand how complex reconstructive surgery is delivered in diverse environments will be both humbling and transformative. It will challenge my assumptions, deepen my adaptability, and broaden my understanding of how innovation thrives in resource-limited settings. Experiencing this level of collaboration and resilience will be a mind-opening moment in my journey—reinforcing my commitment to becoming an academic craniofacial surgeon who advances surgical science while building bridges across borders to expand access to life-changing care worldwide.