I am a fourth-year Emergency Medicine resident completing a 3–4 week international elective in Kampot, Cambodia, focused on advancing emergency medicine education, curriculum development, and capacity building. This project aims to strengthen the local EM training program through bedside teaching, academic collaboration, and sustainable systems support—while deepening my own understanding of global emergency care and health equity.
My primary focus will be bedside and didactic teaching designed to enhance clinical skills and critical thinking among EM trainees. Through daily case-based learning and structured sessions, I will cover a range of high-yield topics—including POCUS, resuscitation, orthopedics, and cardiology, among others—emphasizing resource-conscious decision-making, teamwork, and communication in acute care. Trainee and faculty feedback will guide ongoing refinement to ensure relevance and sustainability.
Working alongside local faculty, I will support curriculum development by reviewing the existing one-year EM program and developing recommendations for expansion into a two- or three-year model. Drawing on U.S. and international frameworks, I will share adaptable templates for learning objectives, procedural logs, and assessment tools, and continue offering remote mentorship following the rotation.
To strengthen academic and research capacity, I will facilitate a workshop on research fundamentals and help identify feasible quality improvement or research projects aligned with local priorities, such as trauma outcomes or triage optimization.
This project combines clinical education, systems development, and collaborative learning to strengthen emergency care delivery in Cambodia, promote sustainability, and advance locally led EM training.
The primary population served by this project includes emergency medicine trainees, faculty, and, indirectly, patients receiving acute care in Kampot, Cambodia. Trainees in the local EM program will benefit from enhanced bedside teaching, structured didactics, and mentorship, gaining essential clinical skills and decision-making strategies in areas such as POCUS, resuscitation, orthopedics, and cardiology, among others. Strengthening the knowledge and confidence of these emerging clinicians will improve the quality and safety of emergency care across the region.
Faculty will also benefit through collaborative curriculum development, access to adaptable teaching materials and assessment tools, and guidance on sustainable program improvements. Empowering local educators promotes long-term capacity building and ensures improvements continue beyond the rotation.
Patients in Kampot are an indirect but crucial beneficiary population. By supporting the development of well-trained EM physicians and structured postgraduate training, the project will help provide more timely, evidence-based care for trauma, acute medical conditions, and life-threatening emergencies. Strengthening emergency care in a resource-limited setting has the potential to reduce morbidity and mortality and improve overall system resilience.
This population was chosen because Cambodia is a lower-middle-income country where EM is an emerging specialty and formal postgraduate training is limited. Targeting trainees and faculty ensures that the project’s benefits have a multiplier effect: trained clinicians educate others, lead quality improvement initiatives, and serve their communities.
By combining trainee support, faculty collaboration, and patient-focused outcomes, this elective aims to create sustainable improvements in emergency care and foster a culture of education, research, and continuous learning that benefits both the local workforce and the broader community.
This elective is designed not only to address immediate educational needs but also to create lasting impact for both the Cambodian EM program and my future work as an emergency physician. By engaging in hands-on teaching and collaborative curriculum development, the project will help enhance the confidence, knowledge, and clinical decision-making of EM trainees, while supporting faculty efforts to expand structured postgraduate training in emergency medicine.
Short-term outcomes include improved trainee engagement, strengthened clinical teaching practices, and the introduction of tools for ongoing assessment and skills tracking. The curriculum review and accompanying educational materials will provide a foundation for continued program growth, while early research and quality improvement discussions will foster a culture of inquiry and data-driven improvement.
The project’s impact will extend beyond the rotation through continued remote mentorship and collaboration with faculty in Kampot. The resources and frameworks developed can be shared for adaptation across other regional EM programs, supporting broader capacity building in Southeast Asia.
Personally, this experience will deepen my understanding of how emergency care systems evolve in resource-limited settings and strengthen my ability to teach, mentor, and lead in diverse environments. I plan to integrate lessons learned into my future career in academic and global emergency medicine—advocating for equitable, context-specific approaches to training and care delivery. By building relationships rooted in mutual respect and sustainability, I hope to contribute to long-term improvements in EM education and strengthen global partnerships that continue well beyond my time in Cambodia.
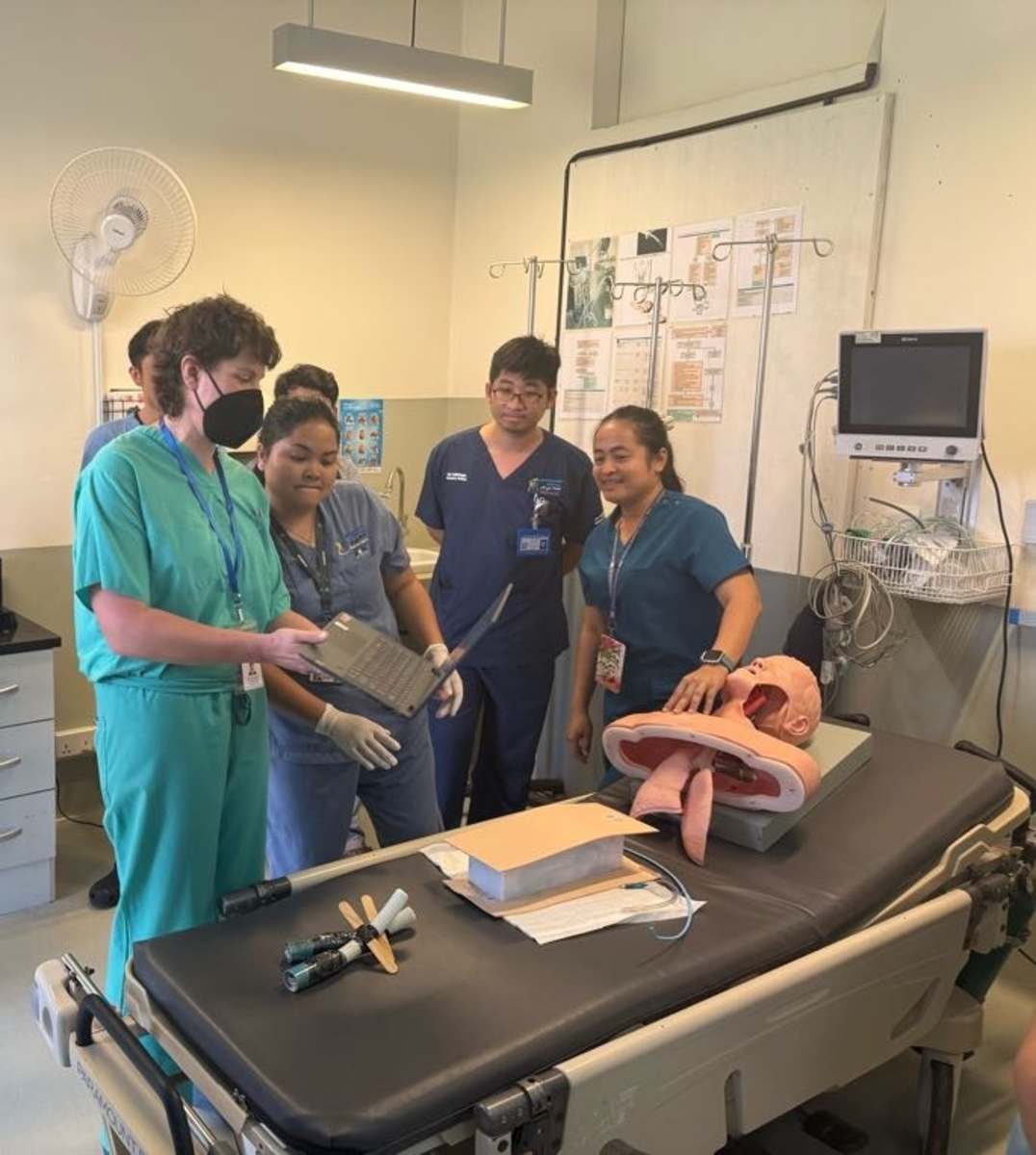
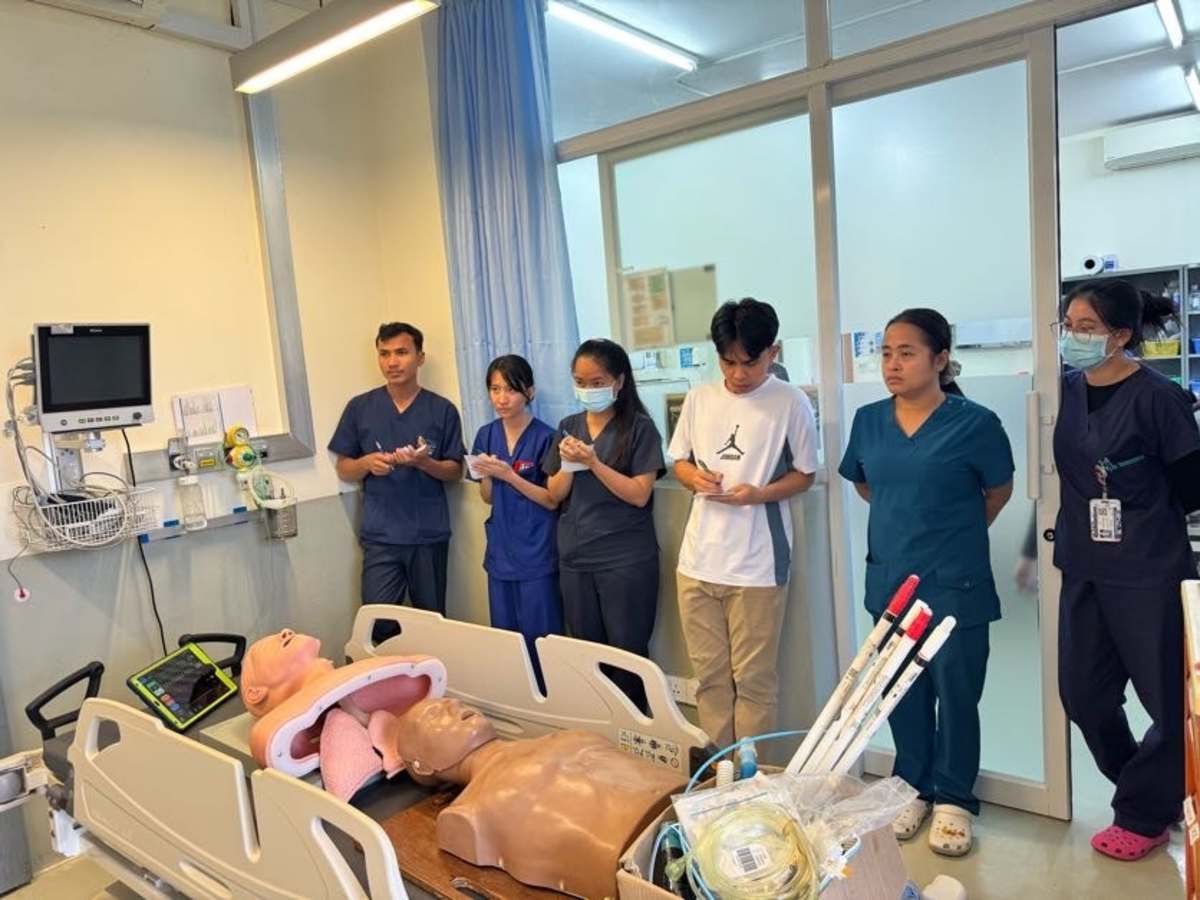
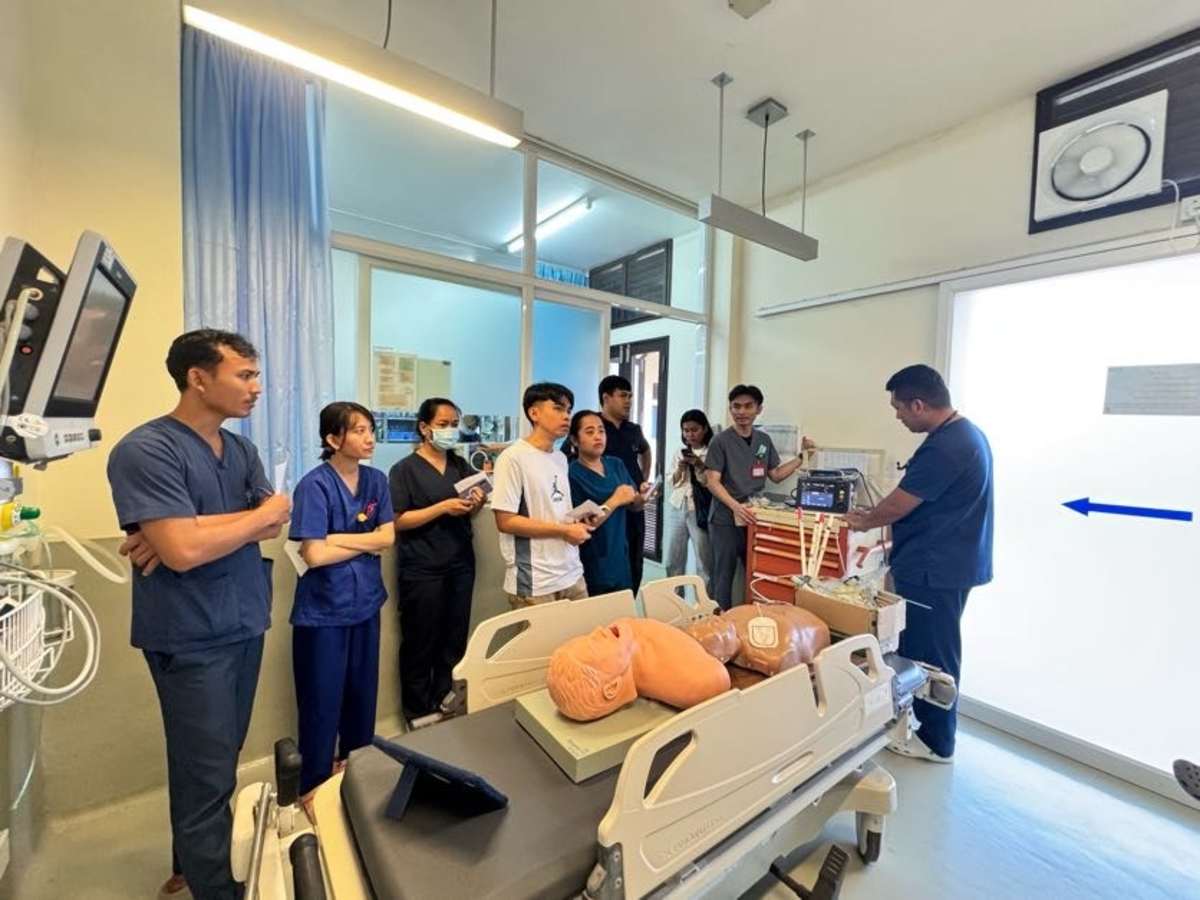
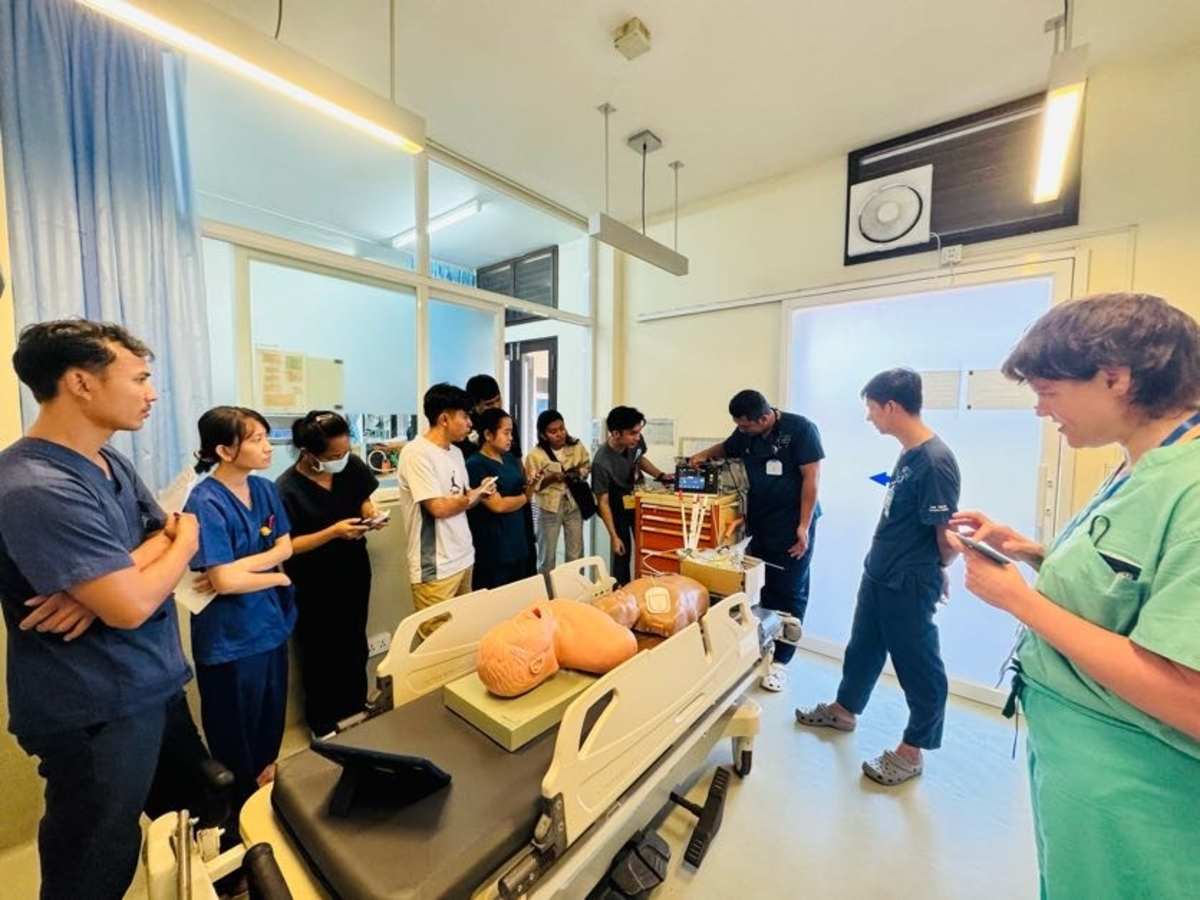
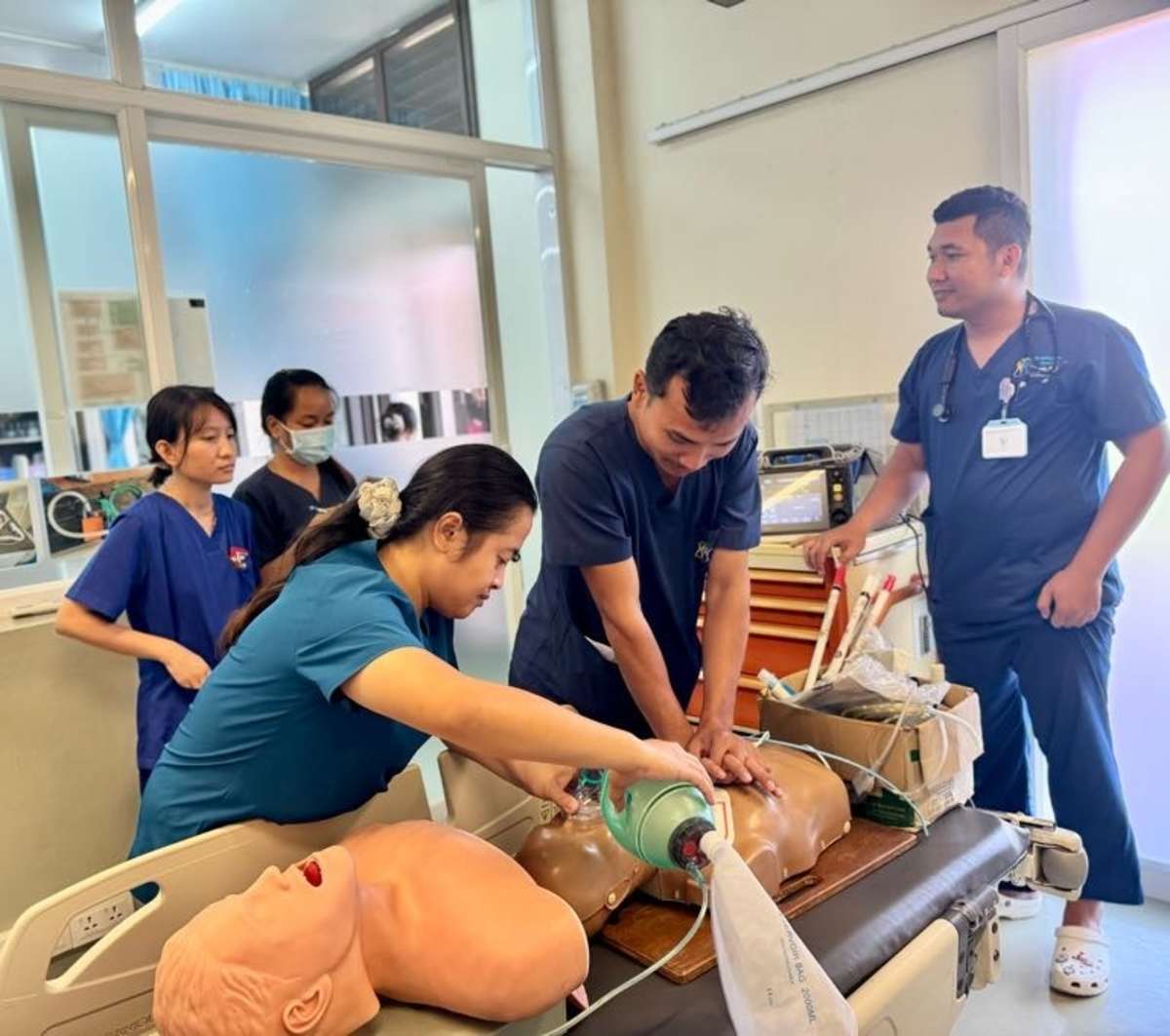

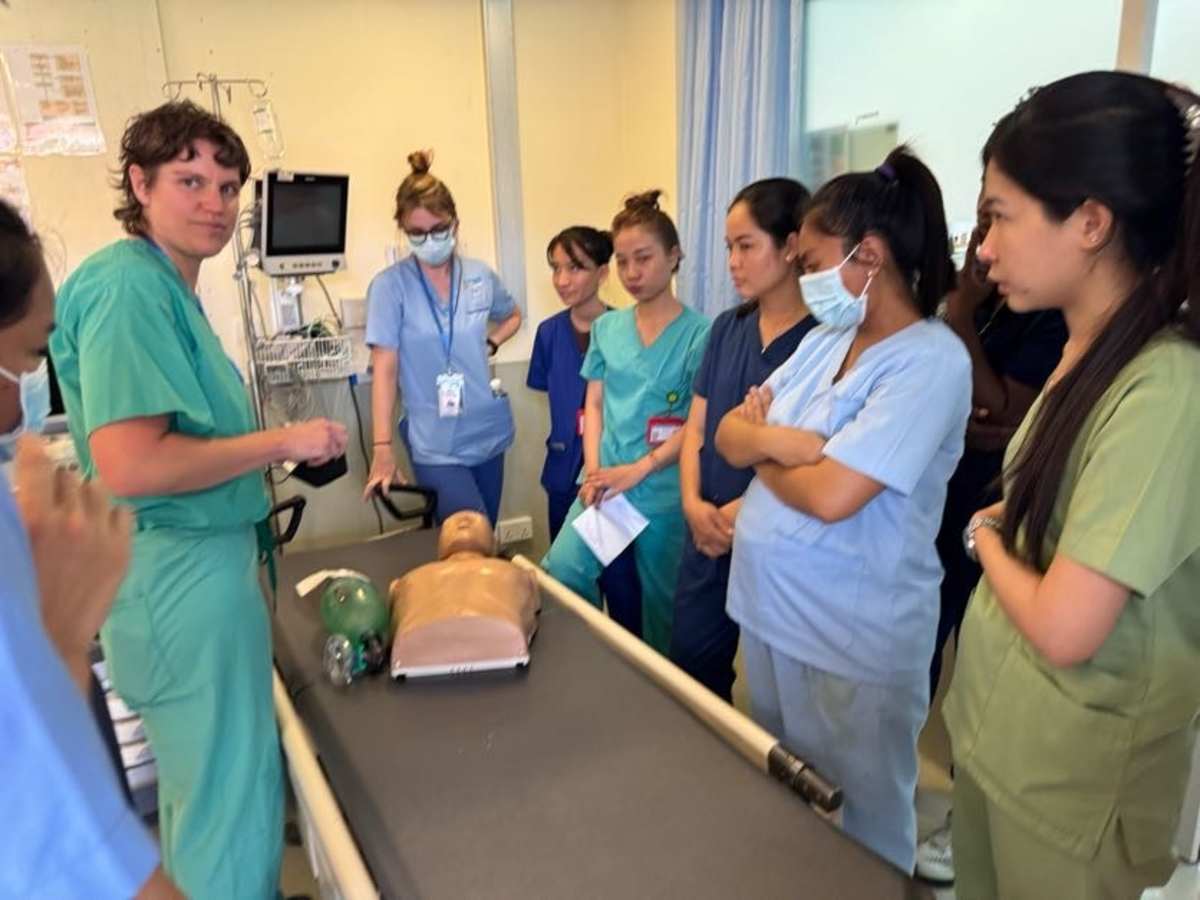
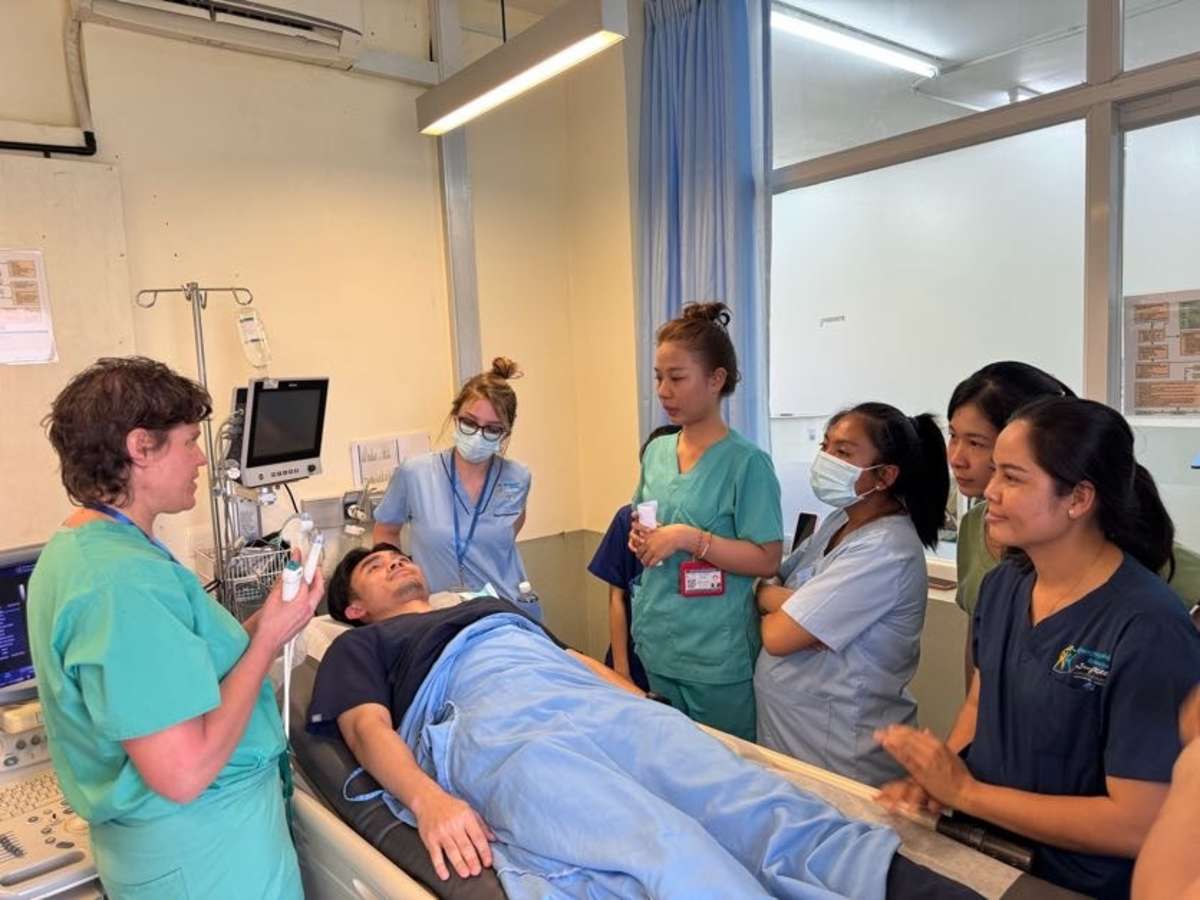
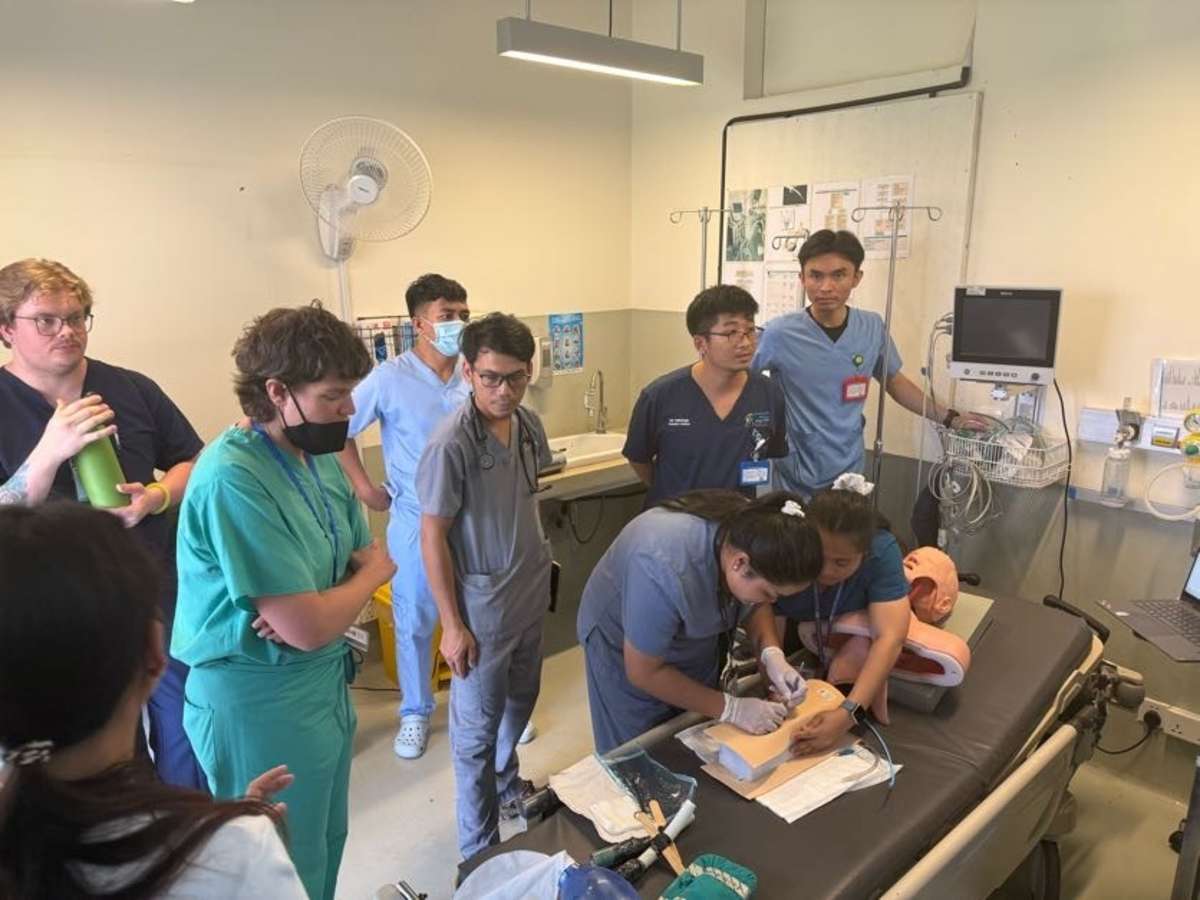

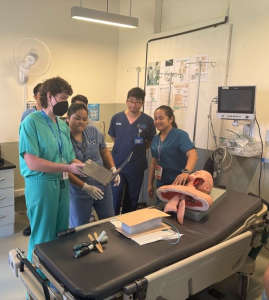


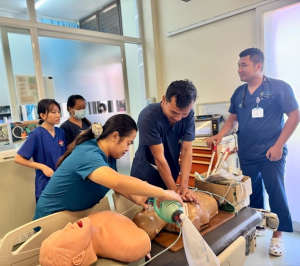

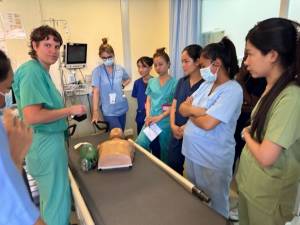
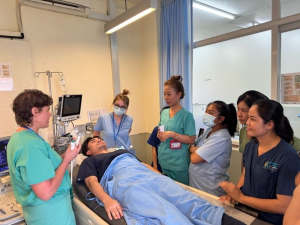


During my emergency medicine elective in Kampot, Cambodia, I had the opportunity to work closely with a diverse group of learners, including emergency medicine residents, internal medicine residents, and attending physicians. Through a strong emphasis on simulation-based education, I led sessions on cardiac arrest management, airway and intubation skills, non-invasive positive pressure ventilation, and point-of-care ultrasound, among other core topics. These sessions were designed to be practical, interactive, and directly applicable to the resource-limited clinical environments in which they practice.
Beyond bedside and simulation teaching, I contributed to ongoing curriculum development efforts for their evolving emergency medicine training program. The program is currently structured as a one-year training experience, with aspirations to expand into a two- or three-year residency. My work focused on helping build sustainable educational frameworks, incorporating simulation, structured didactics, and competency-based progression.
The impact of this experience extended beyond individual learners. By engaging both trainees and attending physicians, the goal was to support a broader culture of emergency care education and systems improvement.