What We Plan To Do:
1. Execute High-Volume Surgeries: We will conduct approximately 75-100 procedures, prioritizing life-changing surgeries such as cataract removal (to restore sight), hernia repair (to restore mobility and work capacity), and essential gynecological procedures (e.g., hysterectomies). We will also be prepared to execute cleft palate repair as needed.
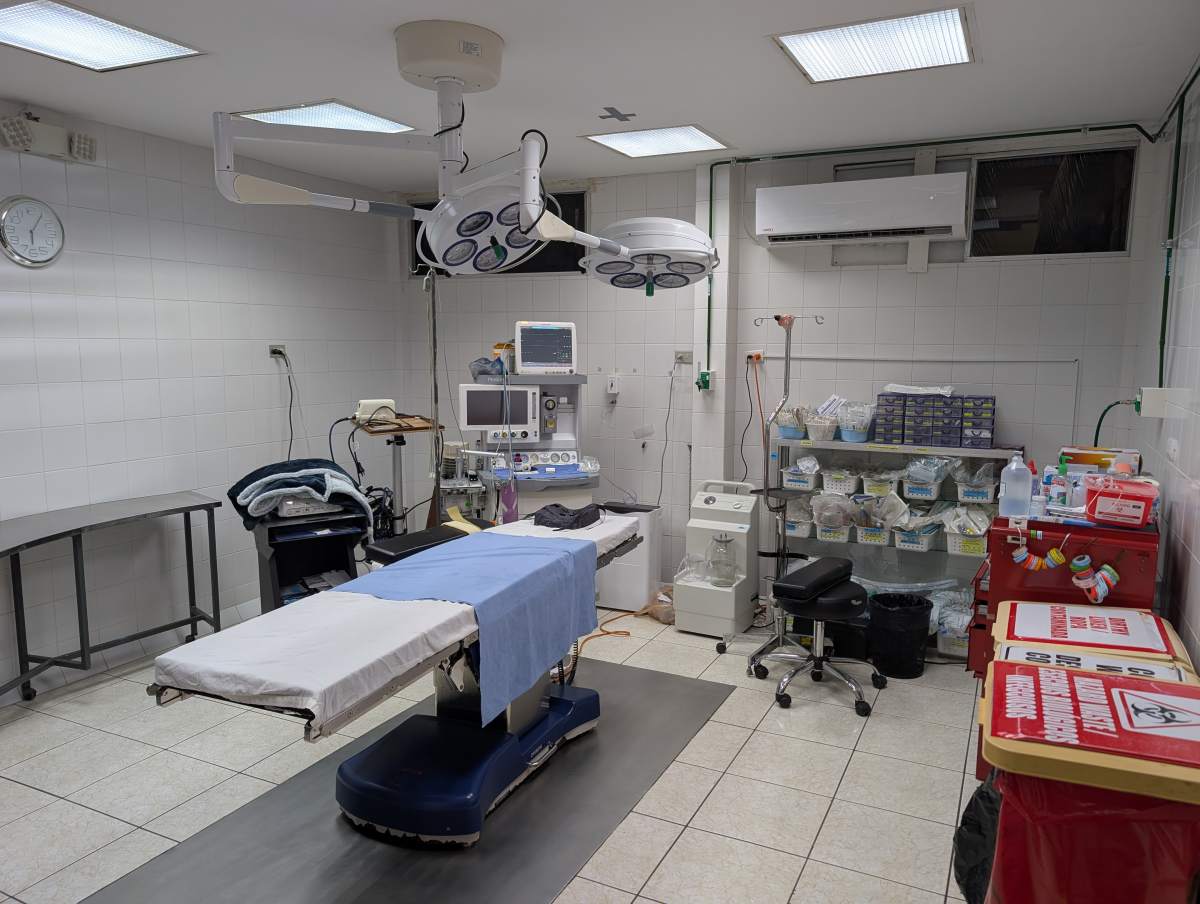
2. Ensure Safety and Protocol: Every procedure will follow rigorous international safety and sterilization protocols, utilizing the facilities at Clinica Ezell, which includes clinic exam rooms, a pharmacy, and a lab.
3. Comprehensive Patient Care: Our model includes full pre-operative screening, the surgical procedure, and post-operative observation and recovery care in the 50-bed ward, ensuring a safe discharge and a comprehensive pharmaceutical regimen.
How It Will Make a Difference:
This project directly addresses conditions that cause preventable blindness, chronic pain, and permanent disability, which prevent the rural poor from participating in the labor force. By providing these surgeries at no cost, we immediately restore function, mobility, and the economic viability of individuals and their families. This shifts the community focus from managing chronic disability to improving productivity and quality of life.
The primary beneficiaries are the underserved rural Mayan and Ladino populations of the area surrounding Clinica Ezell, who face significant barriers to specialized care. These patients are often isolated geographically and cannot afford the costs associated with facility fees, surgical supplies, or professional services required for these critical procedures.
Who Will Benefit:
1. Adults with Debilitating Conditions: Patients suffering from conditions like cataracts, which lead to functional blindness and social isolation, and hernias, which make manual labor—their primary source of income—impossible.
2. Women needing Essential Gynecological Surgery: Addressing chronic pain and risk through procedures like hysterectomies.
3. Children: Benefiting from highly specialized procedures like cleft palate repair, which improves speech, nutrition, and long-term social integration.
Why This Population:
This demographic represents the population most in need of specialized surgical intervention but with the least access to it. We target this population because these procedures are often considered "elective" but are truly life-restoring in a subsistence economy. By utilizing the existing Clinica Ezell infrastructure, we can efficiently reach and serve patients who have been screened and referred via our established network, ensuring we maximize impact where resources are scarcest.
We project completing between 75 and 100 life-changing surgical procedures, resulting in direct, measurable improvements in patient functionality.
1. Functional Restoration: The most critical impact is the restoration of vision (cataract surgery) and the capacity for physical labor (hernia repair), which translates directly to restored income-earning ability for multiple families.
2. Health Infrastructure Strengthening: We contribute significantly to reducing the regional surgical backlog, freeing up capacity in government facilities to handle true emergency cases.
3. Quality of Life: The reduction of chronic pain and disability allows individuals to re-engage fully with their families and communities, promoting holistic well-being.
How Learnings Carry Forward After We Return:
The project is embedded in the long-term presence of Clinica Ezell, ensuring sustainable impact:
1. Professional Training Exchange: Our surgical and anesthesia teams will engage in real-time knowledge transfer with the permanent local medical staff, specifically focusing on advanced surgical techniques and enhanced post-operative management protocols.
2. Protocol Refinement: We will audit and refine the facility's infection control, surgical checklist adherence, and sterilization procedures, strengthening the long-term operational integrity of Clinica Ezell for future teams.
3. Post-Op Continuity: Every patient will be entered into Clinica Ezell’s long-term follow-up system, guaranteeing continuity of care via the facility's permanent staff for wound checks, medication adjustments, and complication monitoring. The learning is institutionalized within the facility itself.

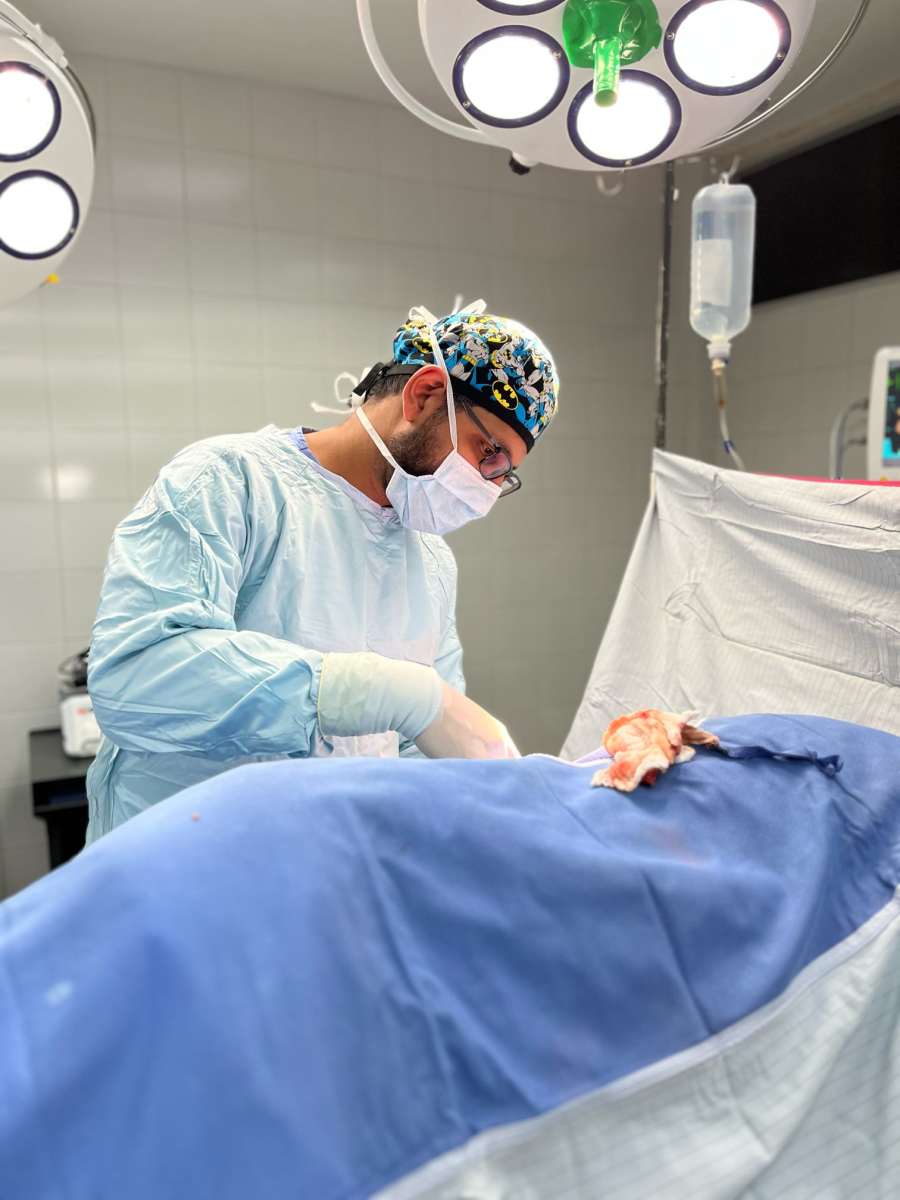








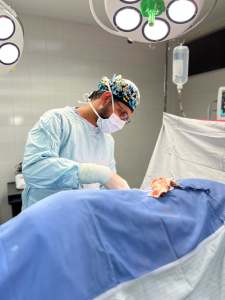




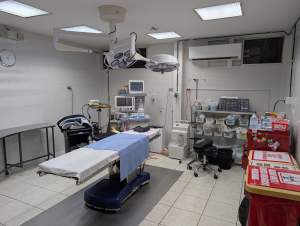





Mission Guatemala: A Lesson in Resourceful Compassion
My recent surgical mission trip to Guatemala was more than just a medical endeavour; it was a profound reminder of why we chose this profession. Operating in an environment where resources are scarce and the safety nets we take for granted are non-existent, we were forced to balance surgical precision with the harsh realities of global health inequity.
The Weight of Limited Follow-Up
In the U.S., we often practice "optimal" medicine, but in rural Guatemala, we practice "sustainable" medicine. The lack of infrastructure and the crushing weight of poverty mean that post-operative follow-up is a luxury many patients cannot afford. This reality dictates our surgical decisions in ways that are often heartbreaking:
Definitive vs. Conservative Care: We performed mastectomies for breast cancer cases where, in a resource-rich environment, we might have opted for a lumpectomy. Without reliable access to radiation therapy or oncology follow-up, the more aggressive surgery is the only way to ensure the patient has a fighting chance at survival.
Late Interventions: We encountered an 8-year-old boy with bilateral cryptorchidism—a condition that should be caught and corrected in infancy. Due to the lack of primary care, we had to perform an orchiectomy. It is a sobering reminder that "access" isn't just about having a surgeon available for a week; it’s about a lifetime of preventative care.
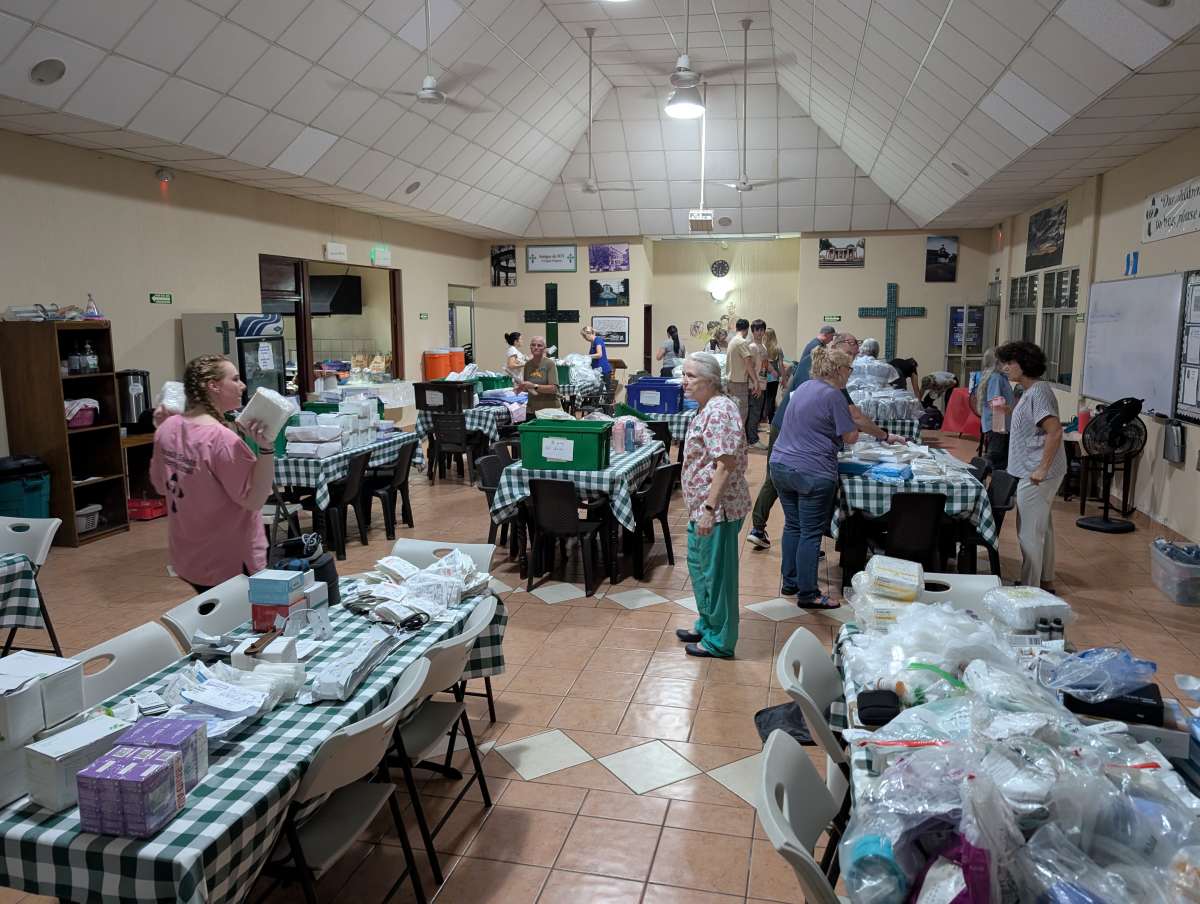
Resourcefulness and Reusing
The contrast in "waste" between American ORs and mission clinics is staggering. In a setting where every penny counts, we pivoted from the disposable culture of the West to a model of rigorous sterilization and reuse:
Supplies: Items like Bovie grounding pads, surgical gowns, and drapes—which are discarded after a single use in the U.S.—were cleaned, sterilized, and put back into service.
Sustainability: This wasn't about cutting corners; it was about ensuring that the next patient in line had the supplies necessary for their procedure.
Recalibrating Pain and Gratitude
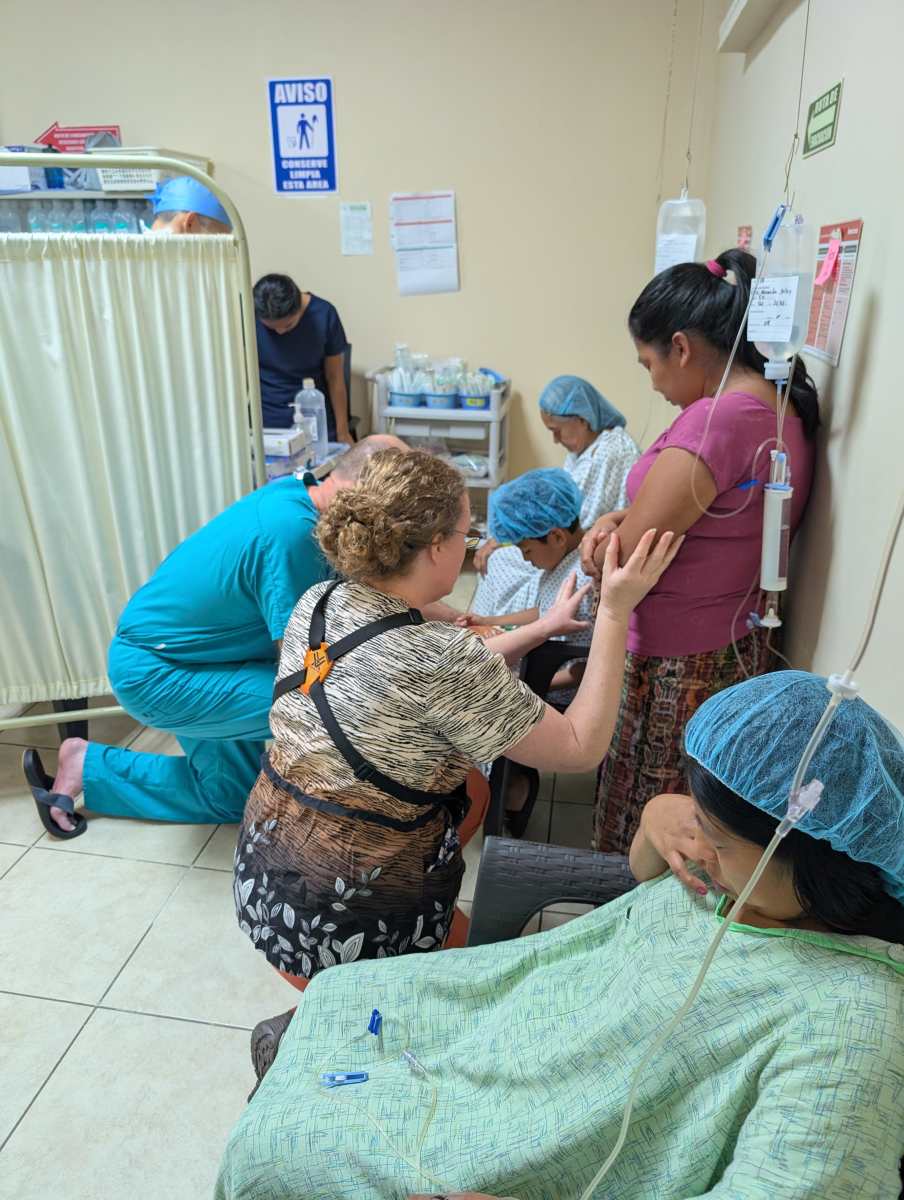
The cultural difference in the perception of recovery was equally striking. In the U.S., the expectation is often "zero pain," leading to a heavy reliance on opioids. In Guatemala, the majority of our patients recovered with nothing more than Tylenol or Ibuprofen.
Despite the physical toll, the spirit of these patients was humbling. Almost universally, the first words spoken upon waking from anesthesia were expressions of gratitude—thanking God and the surgical team. There were no complaints about the lack of "luxury" amenities; there was only the pure, raw relief of finally receiving help.
The Physician’s Responsibility
This trip reinforced a fundamental truth: our medical training is a gift intended for service. Whether we are working through local outreach programs in our own backyards or traveling across borders to underserved regions, we have a duty to bridge the gap in healthcare.
"The measure of our success wasn't just in the number of cases completed, but in the restoration of dignity and health to those the world has largely forgotten."