Vanderbilt University Medical Center Department of Anesthesia has an ACGME-approved month-long rotation in Kijabe, Kenya that I will be participating in during March of 2026. There has been a long partnership between Vanderbilt and Kijabe Hospital that has emphasized the training and development of local providers in order to continue to provide care to the local population long after individuals from the University have left. This rotation allows for residents to participate in clinical care alongside Kenya registered nurse anesthetists (KRNA’s) in order to serve a severely impoverished community lacking easy access to high quality medical and surgical care. Kijabe Hospital is a 363-bed non-profit hospital in Kenya that has surgeons trained in all major surgical subspecialties. Our goal is two-fold, to help further the training of KRNA’s and students by providing supervision and education. And secondly, we are to take on direct patient care roles to help offload some of the clinical burden of the hospital. This will allow Kijabe Hospital to be able to serve even more patients as facilities and available providers are often the rate limiting steps to providing care for even more patients in need.
In Kenya, the ratio of physician anesthesiologists compared to the overall population remains extremely low with many facilities relying on nurse anesthetists as the primary anesthesia providers. By collaborating within these teams, I aim to further sustainable education and care delivery in a context where anesthesia expertise is particularly scarce but highly impactful. Additionally, a large percentage of the eastern African population have a profound lack of access to safe surgery and anesthesia. Some estimates suggest that nearly 93% of the Sub-Saharan African population do not have access to affordable or safe surgery and anesthesia. Kijabe Hospital shines as a beacon in an otherwise largely desolate healthcare landscape in the region. It is an advanced surgical hospital that cares for a significant portion of the Eastern African population who have complex medical and surgical needs. Additionally, it receives patient referrals from all over the region for higher levels of care. The local population served by Kijabe Hospital largely consists of the Kikuyu and Maasi population found in the Great Rift Valley provence in Kenya but draws from many more geographic areas due to the reasons listed above. These people who are burdened by the lack of access to healthcare, some of which may have never met a doctor, are the ones who stand to directly benefit from the continued partnership with Kijabe Hospital.
More important than my impact on direct patient care is that this experience will help further the training and education of local providers. This will allow them to continue to take care of their community long after my time in Kenya has ended and allow for the continued impact on thousands of lives in the future. Sharing our knowledge and teaching local providers will impact patients' lives for decades to come. This is the true legacy of this partnership.
Vanderbilt has a nearly 15-year history working with Kijabe Hospital helping to impact countless providers and patients over that period of time. I believe that the most influential part of this partnership specifically for the anesthesia department has been the involvement of residents and faculty in teaching at the nurse anesthetist school. This allows for us to pass along cutting-edge techniques, knowledge, and training to learners who do not have access to nearly the same level of training and educational wealth that we have access to here in the United States. I know that this will help translate into the local providers continuing to expand their knowledge base and skillset to continue to provide safe anesthesia for complex patients.
Upon returning to Vanderbilt, I plan to share insights gained from this experience through resident conferences and departmental global health discussions with the goal of inspiring additional residents to dive into global outreach. I know that this experience will have a profound impact on me personally and how I will choose to practice anesthesia in the future. I will likely walk away having personally learned more than I will be able to pass along to others. Here in the United States, we have no shortage of resources and, unfortunately, often are extremely wasteful with these resources. Practicing in a resource poor environment will likely change the way I practice anesthesia in terms of being efficient and conscious of the equipment and supplies I use to reduce my carbon footprint left in the operating room. This project will strengthen my development as a globally minded anesthesiologist dedicated to advancing equitable healthcare. This trip will serve as the first, of hopefully many similar future endeavors that I will embark on over the course of my career as an anesthesiologist. Ultimately, I am confident that this experience will help me take better care of my future patients no matter where in the world they may be.
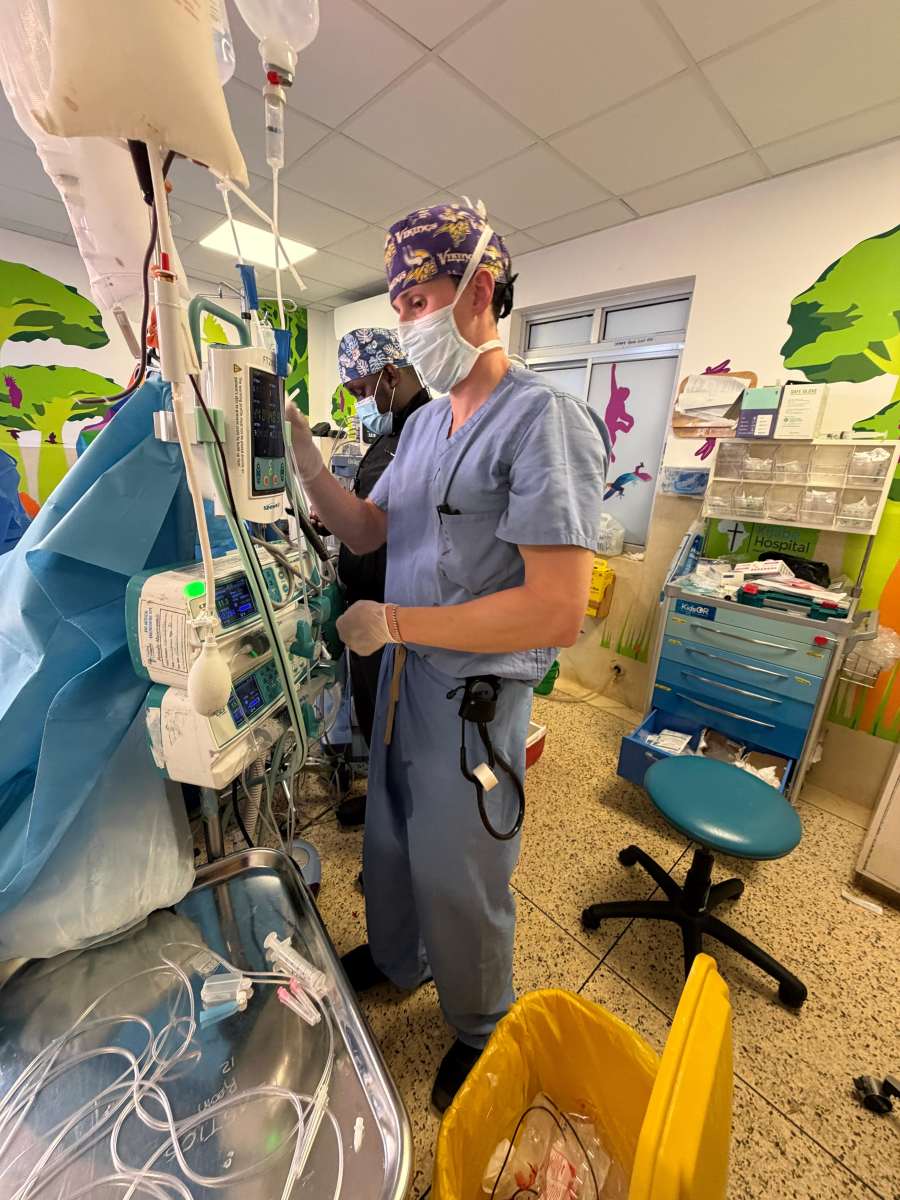




My month in Kijabe, Kenya, was defined not by the volume of cases I participated in, but by the depth of impact each patient encounter carried. Practicing anesthesia in a resource-limited setting fundamentally reshaped my understanding of perioperative care and the profound consequences of access—or lack thereof—to timely medical intervention.
Many of the patients I encountered presented with advanced pathology that would be rare in a well-resourced system. Surgical diseases often progressed unchecked for years due to barriers such as cost, distance, and limited healthcare infrastructure. As a result, cases that might be elective elsewhere became urgent or even life-threatening. Large abdominal tumors, neglected fractures, and advanced infections were not uncommon. Each patient carried not only a medical diagnosis but also a story of delayed care shaped by systemic limitations.
One particularly striking group of patients were those undergoing surgery for large, longstanding masses. These patients frequently adapted to their conditions over years, continuing to work and support their families despite increasing physical burden. By the time they reached the operating room, their physiology was often significantly compromised. Providing anesthesia in these situations required careful planning, vigilance, and adaptability, especially in an environment where advanced monitoring and subspecialty backup were limited. Yet, the postoperative transformations were remarkable—patients who had lived with debilitating conditions were suddenly able to move, breathe, and function with newfound freedom.
Pediatric patients formed another vulnerable population. Many children presented with congenital anomalies or untreated conditions that had progressed due to delayed diagnosis. Myelomeningocele and severe hydrocephalus cases were almost a daily occurrence. Providing anesthesia for these patients required not only technical skill but also a heightened sensitivity to the emotional weight carried by their families. Despite language barriers and cultural differences, the trust placed in the medical team was profound. The resilience of these children and their families was both inspiring and sobering, reinforcing the privilege and responsibility inherent in providing care.
A central focus of my time in Kijabe was working alongside Kenya Registered Nurse Anesthetists (KRNAs). These providers are the backbone of anesthesia care in many parts of the country, often practicing independently in challenging environments. The patients we cared for were directly impacted by the knowledge-sharing and collaborative approach we fostered. Teaching was not a one-directional process; it was an exchange. While I offered perspectives on perioperative management, crisis resource management, and evidence-based practices, I learned equally valuable lessons in resourcefulness and adaptability. The KRNAs demonstrated an ability to deliver safe and effective anesthesia with limited tools, relying on strong clinical assessment and experience.
The impact on patients extended beyond individual cases. By investing in the education and support of local providers, the benefits of this work will continue long after my departure. Each skill reinforced, each concept clarified, contributes to improved care for future patients. Regardless of geography or resources, patients entrust anesthesia providers with their lives at their most critical moments. In Kijabe, that trust often existed in the context of significant uncertainty, yet it was given freely and without hesitation. Bearing that responsibility in a setting with fewer safety nets heightened my awareness of the core principles of anesthesia: vigilance, preparation, and compassion.
Ultimately, the patients I encountered in Kijabe were not defined solely by their medical conditions, but by their resilience, dignity, and hope. Their lives were impacted not only by the surgeries performed, but by the collective effort of a team committed to providing care in the face of limitations. This experience reinforced my commitment to advancing equitable access to safe anesthesia and deepened my appreciation for the profound difference that dedicated providers can make, regardless of setting.