Partnering with the Medical College of Wisconsin, anesthesia residents of the University of Iowa will travel to Columbia to provide anesthesia for over 100 procedures, primarily pediatric cleft lip/palate repairs. This mission will provide necessary medical care otherwise unavailable to these communities.
This mission primarily serves pediatric patients and their families unable to obtain needed surgeries otherwise. While multiple ENT and plastic surgeries are performed, one of the primary goals is to perform cleft palate repairs so that these children may be able to grow, eat, breathe, and speak more easily. We will spend several days setting up a clinic to triage patients according to urgency of procedure. This will help patients who don’t have access to advanced care. Through the Medical College of Wisconsin, we also have established relationships with the preexisting providers in this area, so we can ensure the upmost quality of care and safety for our patients.
Through this mission, we will provide needed surgeries to over 100 patients. We will also participate in reciprocal education with providers there - bringing our anesthetic techniques and knowledge there while also learning from their practices. This will hopefully advance care, improve patients’ lives, and allow our own providers to grow in multicultural medical practice.

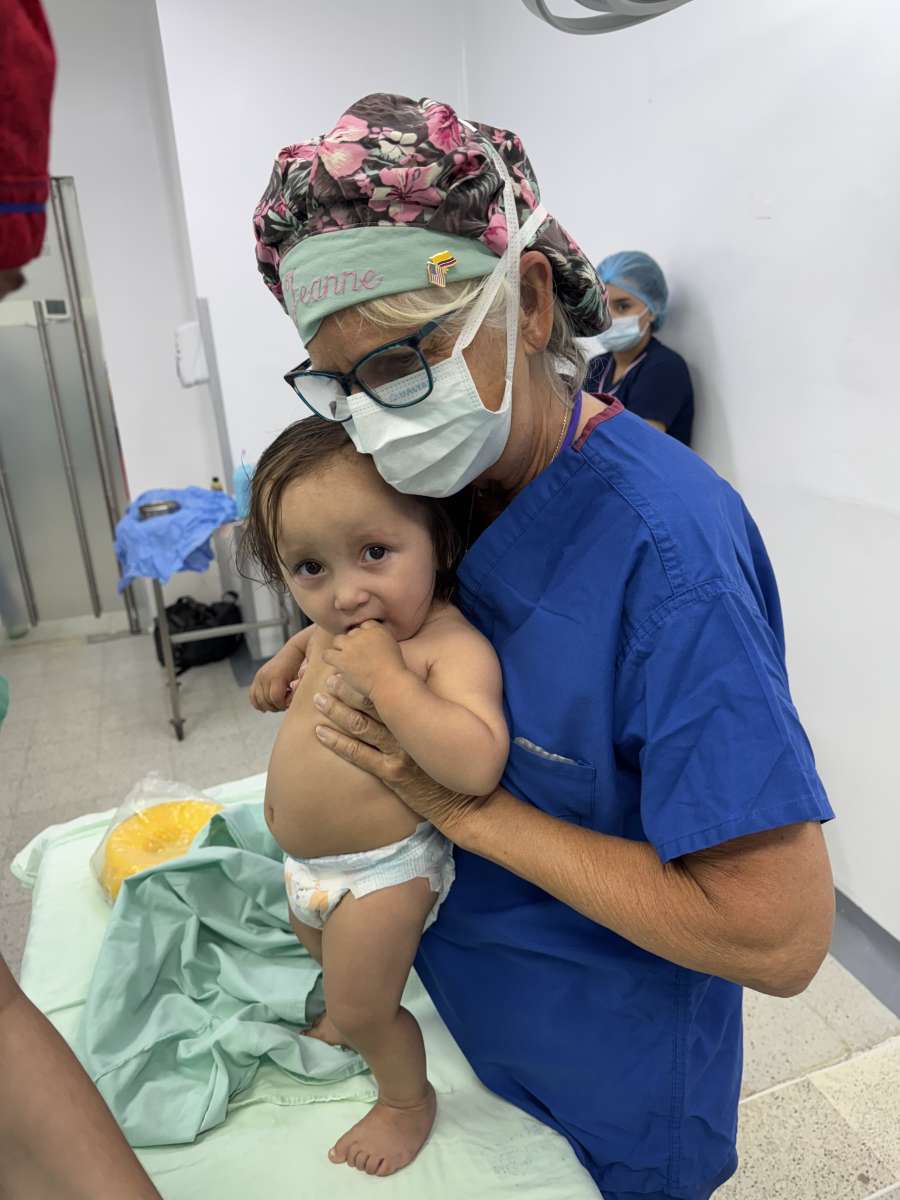






For 38 years, the “Wisconsin Medical Mission” has returned to Bucaramanga, Colombia with a singular purpose: to provide reconstructive surgical care to children and families who otherwise would go without it. This year, we had the privilege of joining that longstanding effort, serving as the anesthesia team for approximately 70 plastic surgery cases over two intensive weeks. What we experienced was more than a surgical trip—it was a reminder of the profound impact that coordinated, compassionate, and safe perioperative care can have on entire families and communities.
Although Colombia has a national insurance system, access does not always equate to availability. Many of the children we cared for had waited years for procedures that, in other settings, would be performed in infancy or early childhood. Several families traveled more than 15 hours by bus to reach Bucaramanga, carrying not only their children but also hope for a different future. In the span of a two-day screening clinic, we evaluated over 150 patients to build a safe and efficient two-week, three–operating room schedule. From this group, more than 70 children ultimately underwent surgery.
The cases were as complex as they were meaningful. Burn contracture releases allowed children to extend elbows and knees that had long been fixed in painful positions. Syndactyly repairs separated fused fingers, creating the possibility for improved hand function and independence. Cleft lip and palate repairs restored the anatomical foundation for speech, feeding, and social integration. Behind each diagnosis was a child who would now be able to grasp a pencil, articulate words more clearly, or eat without difficulty. These functional changes ripple outward—improving educational opportunity, social development, and family well-being.
As anesthesiologists, our responsibility was to ensure that each of these transformative procedures was delivered safely. Pediatric anesthesia in a mission setting requires vigilance, adaptability, and teamwork. We collaborated closely with local surgeons, nurses, and anesthetists, aligning on protocols, equipment, and recovery processes. Despite differences in resources and workflows, our shared commitment to patient safety created a seamless perioperative environment. Every child received thoughtful preoperative evaluation, tailored anesthetic planning, vigilant intraoperative monitoring, and attentive postoperative care.
Importantly, the exchange was mutual. We learned about the Colombian healthcare landscape, referral pathways, and the realities of delivering specialty care within a national insurance framework that still leaves gaps in access. Local providers shared insights into regional pathology patterns, cultural considerations, and long-term follow-up challenges. In turn, we exchanged perspectives on pediatric airway management, multimodal analgesia strategies, and perioperative safety systems. This bidirectional education strengthened not only individual practice patterns but also the broader partnership that has sustained this mission for nearly four decades.
The impact of the trip cannot be measured solely in case numbers. It is reflected in parents who wept with relief after seeing their child’s repaired smile, in children flexing newly separated fingers for the first time, and in the trust placed in us by families who traveled across the country for care. For two weeks, through careful planning and collaborative effort, we were able to help restore function, dignity, and possibility.
Participating in the 38th year of this mission reinforced a simple truth: safe anesthesia is not ancillary to surgical care—it is foundational. By providing it, we helped make transformation possible for more than 70 children and their families, and in doing so, we were transformed ourselves.