Over the course of five high-volume surgical days, our team will provide surgical care and education otherwise unavailable to those from the local community. Structured teaching sessions will focus on perioperative and operative management for head and neck patients. I will be supervised onsite by Dr. Mona Gangar, Dr. Bradley Schiff, and Dr. Vikas Mehta, all attending physicians at Montefiore with experience in international surgical outreach.
My responsibilities will extend before, during, and after the mission. Prior to departure, I will assist in acquiring product and financial donations, fundraising, and logistical planning. During the mission, I will coordinate daily activities to ensure safe and efficient use of operating rooms, oversee triage and surgical scheduling, and assist with both operative and perioperative care. I will also contribute to education through lectures and hands-on training for local providers. Following the mission, I will help ensure patients receive appropriate postoperative care and follow-up, and I will assist in reporting outcomes to sponsors.
The population served on this mission includes patients from Pakse and the broader southern Laos region, an area where access to specialized head and neck and craniofacial care is extremely limited. During the planning process, as with all of our mission sites, we have seen firsthand the severe financial constraints faced by the local community. Many patients are unable to afford travel to larger cities where advanced surgical services are available, leading them to live for years with conditions that are both functionally debilitating and socially stigmatizing—conditions that are often easily correctable with timely surgical intervention.
Our team specifically targets this population because they represent individuals with high unmet surgical needs and the least ability to access care through conventional pathways. By providing evaluations and surgery at no cost, along with financial assistance for transportation, lodging, and perioperative support, we aim to remove the major barriers that prevent these patients from seeking treatment.
We anticipate completing 80–100 surgeries during the mission week. Approximately one-third of these cases will involve children with cleft lip and palate—patients who often experience profound social stigma, feeding challenges, speech delays, and long-term psychosocial consequences. Other beneficiaries will include adults with benign and malignant head and neck masses, chronic infections, congenital lesions and facial deformities affecting breathing, swallowing, or appearance.
By delivering specialized care directly to this underserved region, we hope not only to transform immediate health outcomes but also to enhance long-term quality of life for some of the region’s most vulnerable and disadvantaged patients.
The expected impact of this mission extends far beyond the patients we treat during the week in Pakse. Champasak Provincial Hospital currently has four ORL physicians and several general surgeons who manage head and neck conditions but are limited to basic procedures due to constraints in training, equipment, and case exposure. A core component of our mission is capacity-building: local surgeons will actively participate in every operative case, allowing for hands-on training in more advanced techniques. This skills transfer is essential for creating sustainable, long-term improvements in regional surgical care.
In parallel, our team will contribute to the global health knowledge base through a structured research initiative led by two medical students assessing the feasibility and effectiveness of telehealth for postoperative follow-up after international surgical missions. They have developed the study design, secured necessary approvals, and prepared data collection tools. During the mission, we will enroll patients and establish a standardized telehealth follow-up schedule. Because continuity of care is a longstanding ethical challenge in global surgery, this project has the potential to demonstrate telehealth as a practical, scalable adjunct for safe postoperative monitoring. Current literature is limited, and our findings may help guide best practices for future mission teams.
Finally, this mission serves as an important training and mentorship opportunity. In addition to seasoned global health volunteers, our team also brings medical students, residents, and new volunteers. We aim to cultivate the next generation of global surgeons and healthcare advocates. Through direct exposure to the needs of underserved communities and the impact of collaborative care, we hope to inspire lifelong commitment to global health and ensure these efforts continue to grow long after our return.

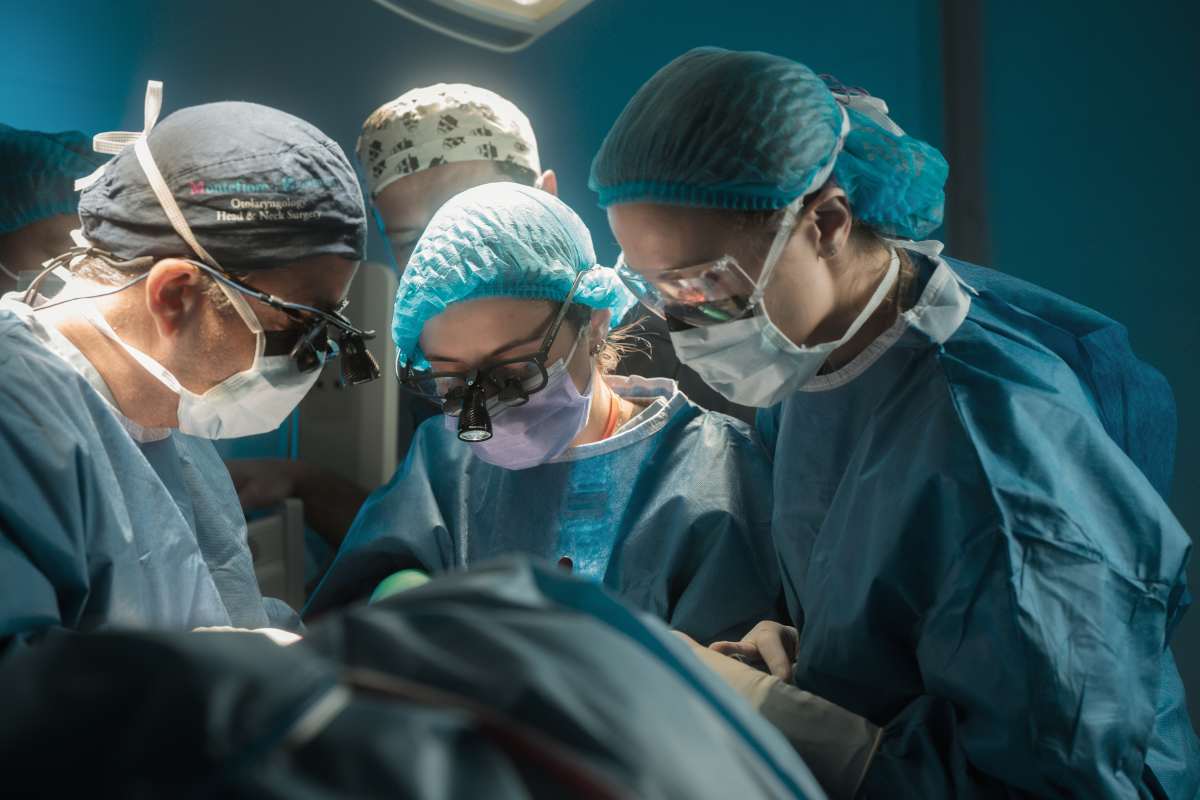



The laotian patients traveled hundreds of miles to recieve care from our team. Many were with their families and camped out at the hospital to be evaluated. Most were poor and many were illiterate. The patients were all deeply appreciative of our service.