This project will implement Phase 2 of a targeted point-of-care ultrasound (POCUS) training program at Hospital Nacional Juan José Ortega de Coatepeque, Guatemala. Building on the pilot with medical students, Phase 2 expands to internal medicine clinicians, equipping them with skills to identify pleural effusions and ascites—critical markers in conditions such as dengue hemorrhagic fever, cirrhosis, and pneumonia.
The intervention consists of a standardized workshop followed by longitudinal mentored scanning, structured image review, and case-based discussions. Participants will gain confidence in probe handling, image acquisition, and bedside interpretation, while selected local champions will receive advanced training in teaching methodologies to sustain the program.
By embedding Spanish-language, open-source materials and a train-the-trainer model, this project strengthens diagnostic capacity, improves equity in care delivery, and lays the foundation for scalable curriculum integration across Guatemala and similar resource-limited settings.
The primary beneficiaries are internal medicine clinicians at Hospital Nacional Juan José Ortega de Coatepeque, a rural public hospital serving a large catchment area with limited diagnostic resources. These providers currently rely on physical exam and plain radiography, with no radiologist on site, leaving critical gaps in timely diagnosis and safe procedures.
By equipping internists with POCUS skills, the project directly addresses their expressed interest and capacity for training, while indirectly benefiting the thousands of patients they serve—particularly those with tropical infectious diseases, cirrhosis, cancer, and respiratory illnesses. Local champions identified during training will extend the impact by teaching future cohorts, ensuring sustainability and broader reach.
The project is expected to:
• Improve clinician confidence, knowledge, and skill in pleural effusion and ascites detection.
• Strengthen bedside diagnostic capacity, reducing delays in recognition of severe conditions such as dengue hemorrhagic fever.
• Establish a cadre of local champions trained to sustain and expand POCUS education.
• Generate Spanish-language, open-source materials for dissemination across Guatemala and similar contexts.
Learnings will carry forward through scholarly dissemination (abstracts, manuscripts, bilingual reports), integration into local curricula, and ongoing mentorship. The train-the-trainer model ensures that after the project concludes, local clinicians will continue teaching and refining POCUS skills, embedding sustainable diagnostic equity into routine practice.






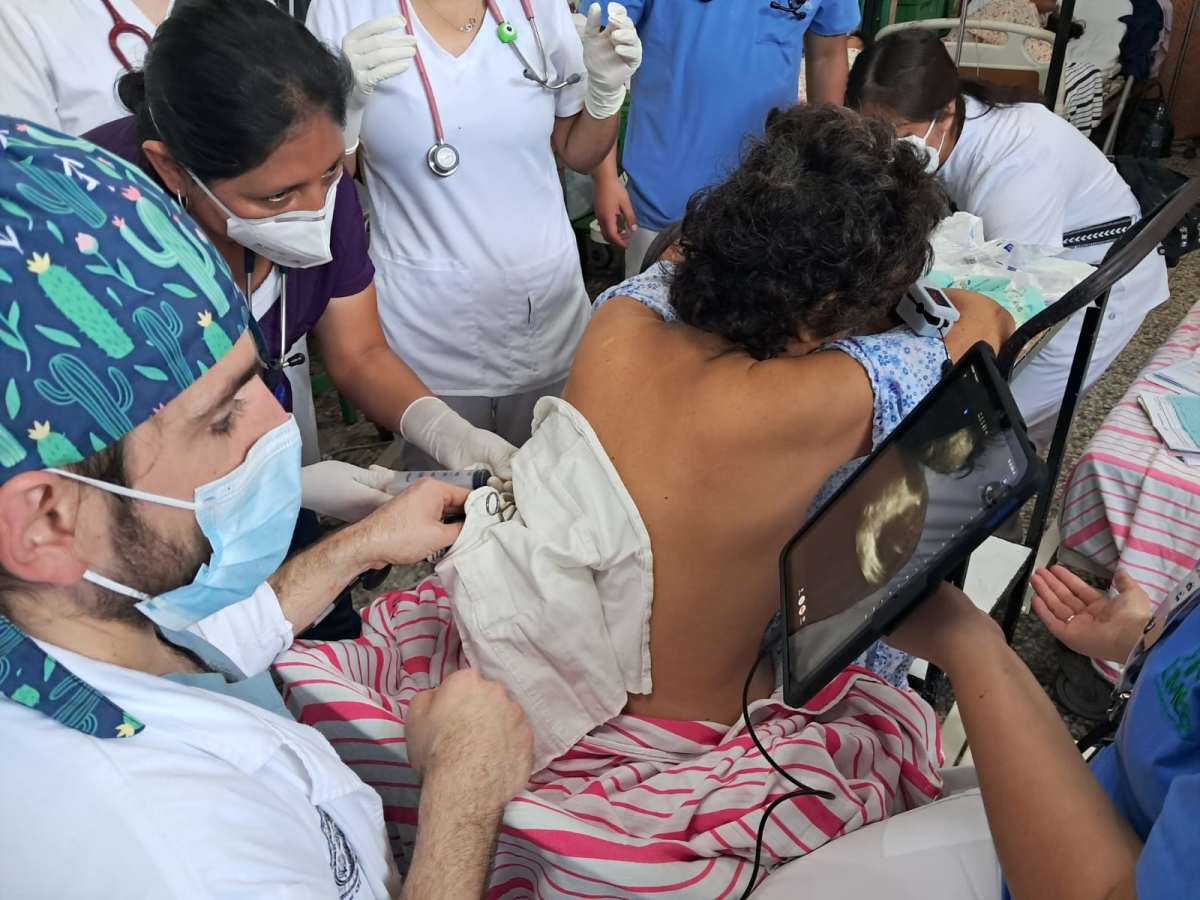






This project directly impacted both clinicians and patients in a rural public hospital in southwestern Guatemala, where access to diagnostic imaging is extremely limited. At Hospital Nacional Juan José Ortega de Coatepeque, internists and medical trainees care for a large population of patients with conditions such as dengue hemorrhagic fever, advanced liver disease, pneumonia, and cancer, often with only a physical exam and a single X-ray machine available, and no permanent on-site radiologist.
The primary group impacted were internal medicine clinicians and final-year medical students, many of whom had never received formal ultrasound training. Despite this, they demonstrated remarkable motivation and commitment to learning. Before the program, most had little to no experience with ultrasound, yet they were eager to build new skills that could immediately improve patient care. Through a combination of a short hands-on course, bedside teaching, and ongoing mentorship, I saw rapid growth in both confidence and clinical ability. Learners progressed from never having held an ultrasound probe to independently identifying pleural effusions and ascites and integrating these findings into real-time decision-making.
One of the most meaningful impacts was the development of local “champions”, trainees who not only adopted POCUS quickly but began teaching their peers. This shift (from learner to teacher) was powerful. It reflected not just skill acquisition, but a deeper sense of ownership and professional identity. As described in our ongoing evaluation, learners expressed excitement about making faster, more accurate diagnoses and a strong desire to continue practicing and teaching others . In a setting with limited faculty and resources, this peer-driven model is essential for sustainability.
The impact extended beyond clinicians to the patients they serve. In a hospital where advanced imaging is often inaccessible or unaffordable, POCUS became an immediate and practical tool to guide care. Clinicians were able to more confidently identify fluid in the lungs or abdomen, make decisions about procedures such as thoracentesis and paracentesis, and recognize severe illness earlier. In some cases, this meant expediting transfer for higher-level care; in others, it meant avoiding unnecessary delays or unsafe procedures. Patients who would otherwise face diagnostic uncertainty benefited from faster, more informed clinical decisions at the bedside.
Importantly, this was not a one-way teaching experience. The clinicians and students I worked with brought deep clinical insight, adaptability, and a strong commitment to their patients despite significant resource constraints. Their enthusiasm—often staying after long shifts to continue scanning and learning—was a clear reminder that the success of global health work depends on local motivation and partnership, not external direction.
Finally, the broader community stands to benefit as this work continues. By training local clinicians and embedding a “train-the-trainer” model, the impact is designed to extend far beyond the initial cohort. These clinicians will go on to teach future students and colleagues, expanding access to diagnostic tools in a region where such resources are scarce. In this way, the project contributes not only to individual skill-building, but to a growing foundation of local capacity and more equitable care delivery.