This proposal outlines a targeted educational initiative to teach pediatric emergency medicine to emergency medicine and pediatric residents in Mozambique. Utilizing direct bedside supervision, weekly didactic and simulation sessions, the project aims to improve the quality of emergency care provided to children at Hospital Centrale in Maputo.
Mozambique struggles to provide effective emergency care for children due to resource and infrastructure limitations, as well as insufficient specialized training. Since 2017, only seven emergency medicine specialists have completed residency training. Hospital Centrale’s Pediatric Urgencies department sees over 200 patients a day and is the main referral center for high acuity pediatric cases, but lacks Pediatric EM subspecialists and has limited Peds ICU specialist availability. Residents care for most patients with minimal direct supervision. Pediatric emergencies significantly contribute to morbidity and mortality, yet formal pediatric emergency medicine education is scarce among providers. Building provider capacity is essential to improve outcomes and strengthen the health system.
The primary beneficiaries of this project are emergency medicine and pediatric residents in Mozambique, with secondary benefits extending to the pediatric patients in the Emergency department.
Mozambique ranked as one of the poorest countries in the world. This contributes to it's high pediatric mortality rate. The emergency department is one of the main access points to healthcare and supporting the education emergency medicine specialists is one of the key factors to improve the delivery of care to critically ill and injured children.
The expected impact: (1) improved clinical knowledge and skills to manage pediatric patients presenting to the Pediatric Urgencies, (2) potential reduction in pediatric morbidity and mortality, (3) system strengthening by building physician capacity and promoting the delivery of best practices while working in a limited-resource setting and (4) building interest in pediatric emergency medicine in hopes of developing this as a subspeciality in Mozambique.
This initiative will support a continued relationship with the Emergency medicine and Pediatric residency programs in Mozambique by the delivery of schedule virtual learning sessions and additional future in-person training sessions. The initiative also aims to develop research and quality improvement collaborations.


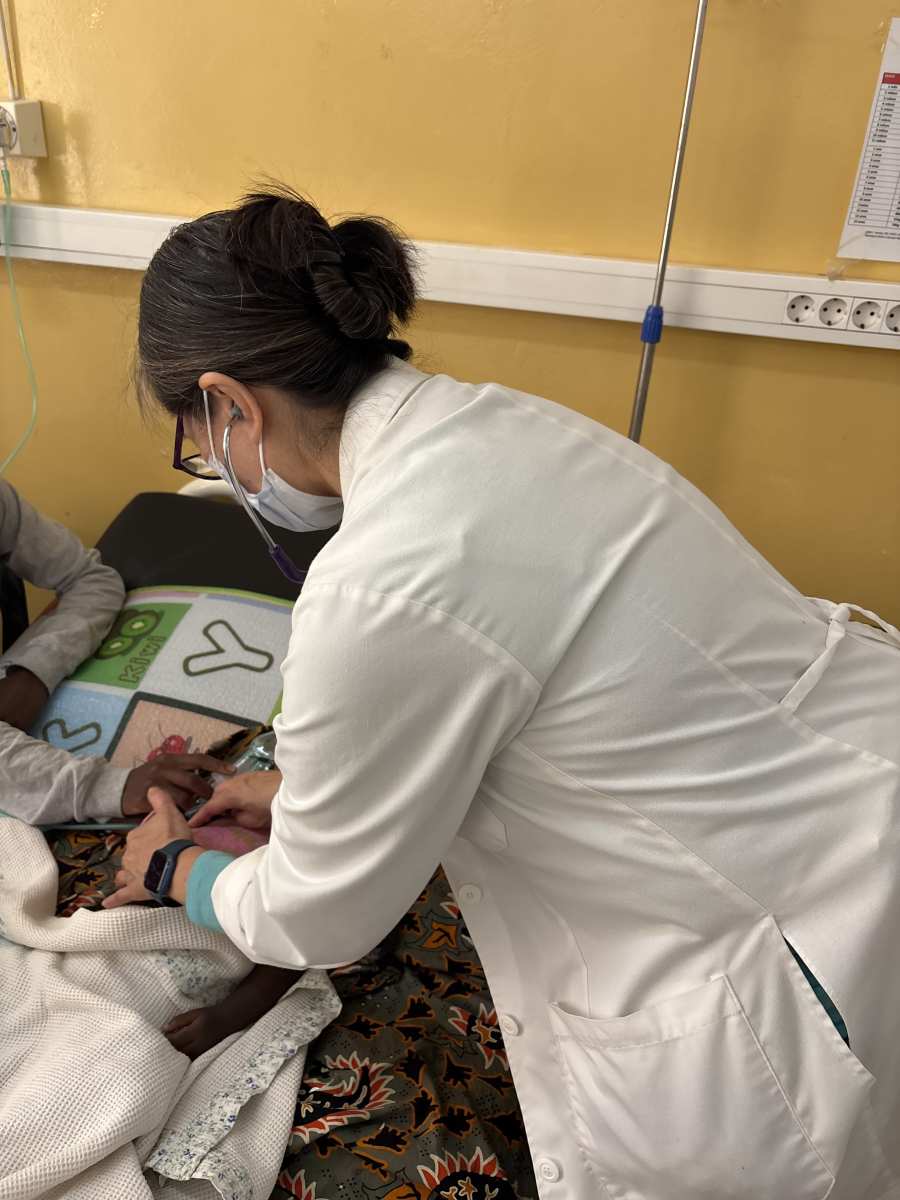



Bronchiolitis, asthma, and gastroenteritis were the most common conditions treated in the Pediatric ED at Mavalane Central Hospital. Without access to noninvasive positive pressure resources such as CPAP and high-flow nasal cannula, we taught the EM residents how to best utilize the resources they had to help manage the patients with moderate to severe respiratory distress. During one shift, we were called to help with an adult cardiac arrest in the adjacent room and quickly realized the staff had limited experience with resuscitations, so we followed up with hands on CPR training during the debrief the next day.
For the EM residents’ education day, we supplemented the didactic topics with low-fidelity pediatric simulation cases and it was a joy to see how the senior residents (who I first met when they started their training) have grown in their confidence in managing critically ill children.
We also began a QI project related to the ED management for patients presenting with DKA. This will be the first time a QI project will be done in the ED and we are hoping to teach the chief resident and the other residents involved the PDSA process so that it can be used for future projects.