My project aims to strengthen the foundational capacity of the mental health infrastructure at the Georgetown Public Hospital Corporation (GPHC), building directly upon the five-year strategic partnership established by Northwell's Center for Global Health.
As a psychiatry trainee, I will dedicate my time to two high-impact areas:
Sustaining the ECT Service: I will provide co-clinical support and ongoing bedside mentorship for the newly launched ECT service at GPHC. This involves working alongside the local specialists Northwell has already trained to ensure the safe, effective, and continuous delivery of this life-saving treatment for patients with severe, treatment-resistant conditions (such as severe depression, psychosis, and catatonia). My role will focus on reinforcing protocols and maximizing utilization.
Launching Addiction Medicine Training: A critical part of the Northwell/Guyana strategy is the development of local capacity to treat substance use disorders. I will assist in developing and delivering focused training and didactic sessions on evidence-based addiction medicine practices. By equipping GPHC physicians, residents, and staff with these skills, we address a major public health burden identified by the Ministry of Health.
This project makes a difference by moving beyond temporary aid to focusing on permanent, sustainable capacity building. By reinforcing two advanced services—ECT and Addiction Medicine—we directly address the treatment gap for Guyana's most vulnerable patients, ensuring that the legacy of the trip is not short-term support, but a strengthened, self-sufficient mental health system.
The population served comprises the citizens of Guyana, specifically those utilizing the nation's largest public hospital system, the Georgetown Public Hospital Corporation (GPHC). My project focuses on patients with the highest burden of severe and untreated psychiatric illness.
I am targeting three primary beneficiary groups:
Patients with Treatment-Resistant Psychiatric Illness: This population has historically been denied access to essential treatments like ECT due to resource limitations. My project ensures the stability of this service, directly benefiting individuals suffering from severe depression, bipolar disorder, and psychosis who have not responded to traditional medication or therapy. By working at the GPHC, which receives complex cases from all regions, the project’s impact extends even to those from remote areas who travel great distances (sometimes two-day journeys) for care.
Individuals with Substance Use Disorders: Guyana faces a significant challenge with substance abuse. By implementing addiction medicine training, the project establishes a new line of evidence-based care for a vulnerable population that often lacks adequate resources for management and recovery.
Local Clinicians and Healthcare Professionals: The core of Northwell’s mission is partnership and mutual benefit. The ultimate beneficiaries are the local GPHC physicians, residents, and staff. By receiving co-education and mentorship in advanced psychiatry, their clinical skills are elevated, creating a sustainable local workforce that will serve countless patients long after my rotation concludes.
This population was chosen because improving mental health is a recognized national priority in Guyana. Furthermore, as an English-speaking country with a strong cultural tie to New York (e.g. Little Guyana in NYC), this partnership allows Northwell to gain crucial cross-cultural understanding that enhances the care provided to our diverse community back home.
The expected impact of this trip is the sustainable enhancement of psychiatric care at GPHC and a profound increase in my cross-cultural clinical competence.
In Guyana (Immediate & Medium-Term Impact):
ECT Service Continuity: The primary expected outcome is the successful continuation and expanded utilization of the ECT service, cementing it as a foundational resource for treatment-resistant patients in Guyana.
Establishment of Addiction Protocols: We will establish standardized, evidence-based protocols for managing Substance Use Disorders, setting the foundation for a permanent addiction medicine educational curriculum at GPHC.
Empowered Clinicians: Local providers will gain increased confidence and autonomy in administering advanced psychiatric treatments, leading to better patient outcomes and a stronger local mental health workforce.
Carry-Forward Learning (Long-Term Impact):
Cultural Competence in New York: My experience will offer invaluable insights into the cultural factors, health beliefs, and stigma surrounding mental illness and substance use in the Guyanese context. I will return to Northwell better equipped to provide sensitive, culturally tailored care to the large Guyanese immigrant population in New York.
Curriculum Development: I will collaborate with the Center for Global Health to document the developed training materials and protocols, making them available for all future residents and clinicians involved in the Guyana partnership.
Telemedicine Strategy: I will identify opportunities to leverage Northwell’s robust telemedicine capabilities to support GPHC clinicians remotely after the trip, ensuring that specialized consultation and mentorship continue, aligning with the Center for Global Health's long-term strategy for bolstering secondary-care systems.









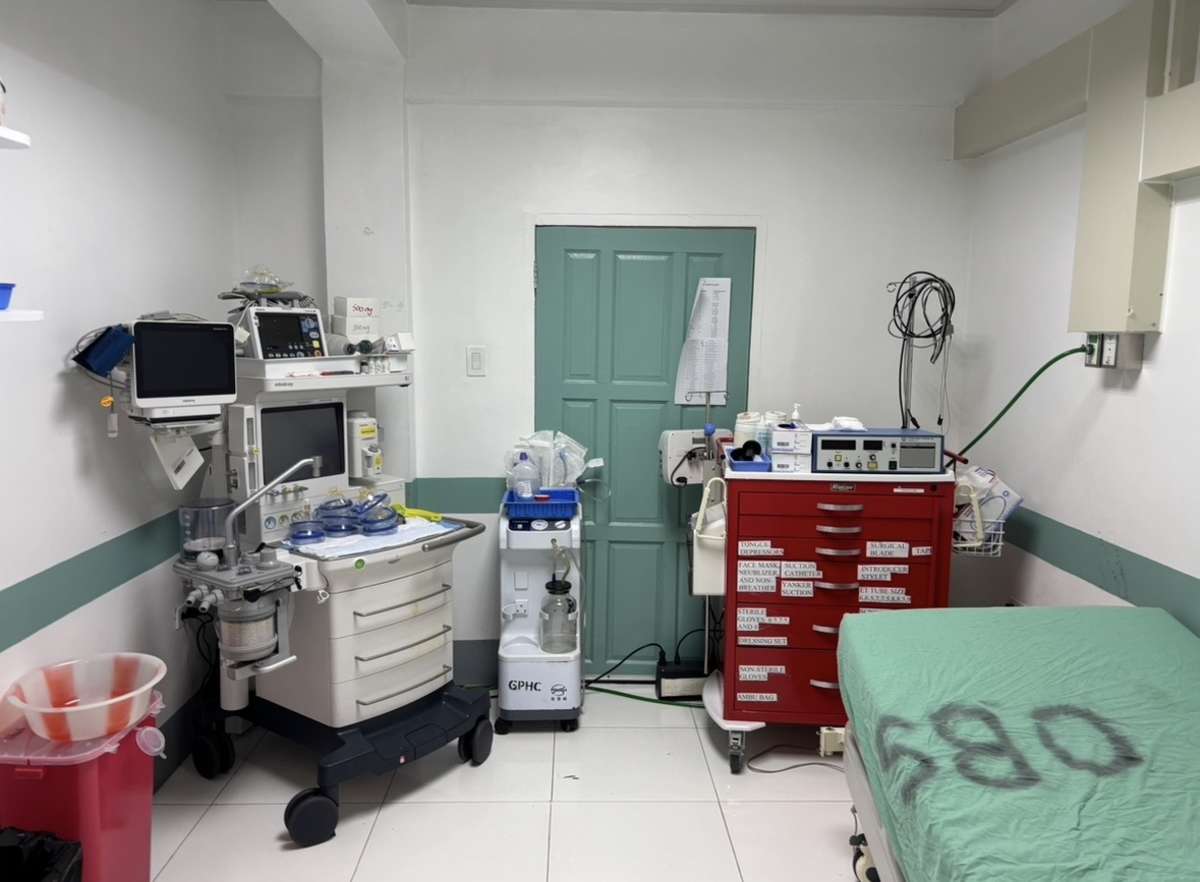

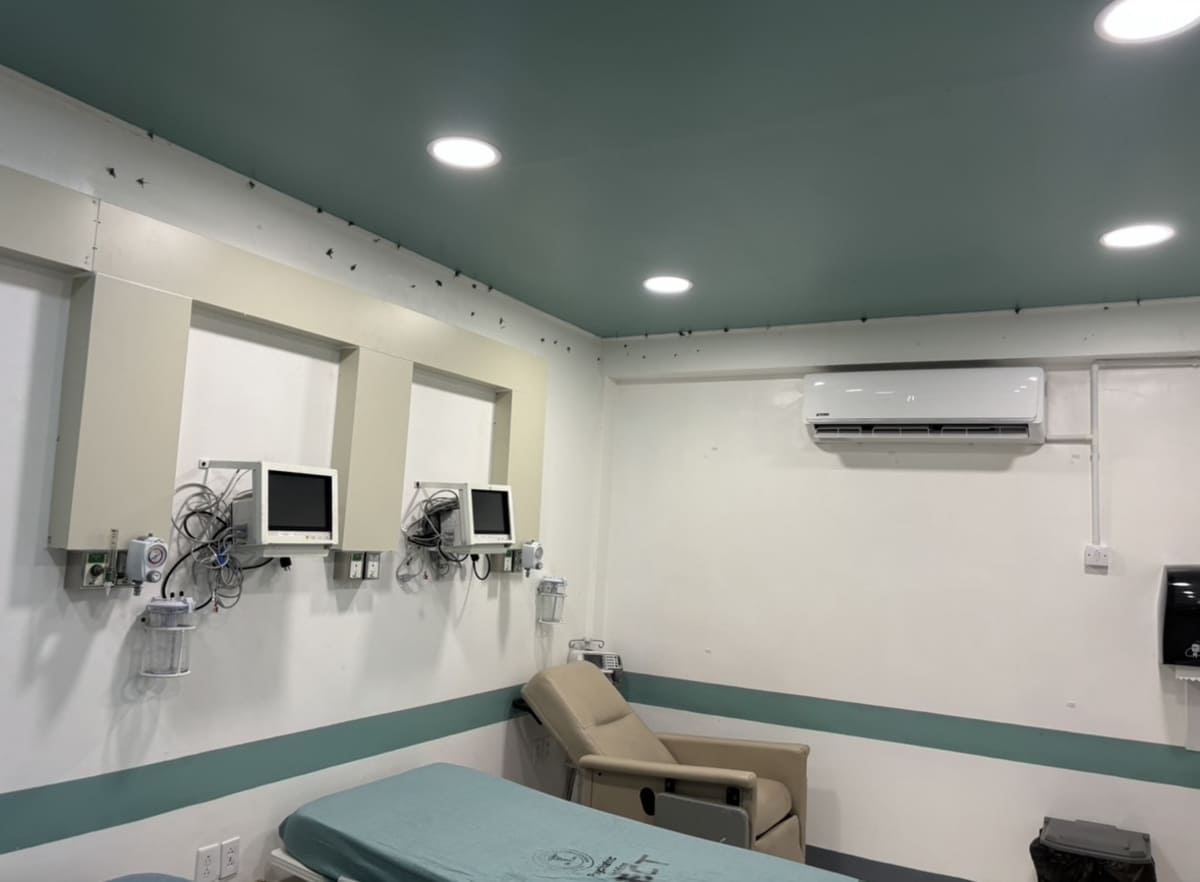










The impact of a global health mission is often measured in statistics—patients seen, medications dispensed, or hours logged. However, my recent trip to Guyana with Northwell Health’s Center for Global Health revealed a much deeper, more intricate tapestry of influence. To understand who was impacted is to understand a symbiotic ecosystem of learning, healing, and structural growth. From the individual patients in the wards to the institutional framework of the Guyanese healthcare system, and even to my own evolving identity as a physician, the impact was profound and bidirectional.
The Impact on Myself and Fellow Residents: A Shift in Perspective
Perhaps the most immediate impact was the fundamental shift in how I, and my fellow residents, perceive the practice of psychiatry. In the United States, we often view psychiatry through a highly standardized, Western lens, governed by strict diagnostic criteria and an abundance of resources. Stepping into the Guyanese clinical environment forced us to confront the reality that psychiatry is one of the most "culturally bound" fields in medicine.
Being immersed in a new setting allowed us to see how mental health is shaped by local socio-economic factors, spiritual beliefs, and community structures. We were challenged to practice "cultural humility" rather than just "cultural competence." We learned that a treatment plan is only as effective as its relevance to the patient’s lived reality. This trip stripped away the safety net of high-tech diagnostics and forced us to rely on our clinical acumen, our ears, and our empathy. The impact on us was a total recalibration of our clinical instincts, making us more resourceful and adaptable physicians.
The Patients: Direct Clinical Intervention and Connection
At the heart of this mission were the patients. My work spanned the entire spectrum of psychiatric care: the high-intensity environment of the Emergency Room, the complex management of the inpatient psychiatric units, and the nuanced, long-term focus of outpatient clinics for both children and adults.
In the ER, the impact was often immediate—stabilizing individuals in acute crisis and providing a bridge to safety. In the inpatient wards, the impact was seen in the meticulous development of treatment plans where we collaborated with local staff to optimize medication regimens despite a different formulary than what we use at Northwell.
Working with the outpatient child and adult populations was particularly moving. In these settings, the impact was found in the human connection. For many patients, having a dedicated team spend time exploring their history and validating their experiences provided a sense of dignity that is often lost in overburdened systems. We weren't just "treating symptoms"; we were working to improve the quality of life for individuals who often face significant stigma regarding mental health. Every treatment plan we conducted was a collaborative effort to provide the best possible care within the local context.
The Local Clinicians: A Global Classroom
The impact on the Guyanese attendings and residents was defined by professional camaraderie and the exchange of knowledge. This was not a one-way lecture; it was a vibrant, bidirectional dialogue. We spent hours discussing the similarities and differences in our diagnostic and treatment guidelines.
We brought insights into the latest Northwell protocols and Western psychiatric trends, while the Guyanese clinicians taught us the art of "resource-limited psychiatry." They showed us how to be effective when you don't have access to every second-generation antipsychotic or every imaging modality. We navigated the complexities of managing chronic mental illness in a setting where social determinants of health—like transportation and food security—are often the primary barriers to recovery. This exchange empowered both sides, fostering a global network of psychiatric professionals who are now better equipped to handle diverse patient populations.
The Hospital and the System: A Commitment to Sustainability
The Northwell-Guyana partnership is designed for longevity, and the impact on the hospital facility itself is a testament to that vision. Unlike "voluntourism," which can be transient, Northwell’s Center for Global Health is deeply integrated into the care of the facility.
Our presence helped identify critical gaps in resources, from specific medication shortages to the need for updated clinical spaces. Because Northwell remains involved with ongoing funding and infrastructure support, our trip served as a "needs assessment" that will inform future investments. We weren't just there to provide temporary relief; we were there to help strengthen the foundation of the hospital. By identifying these needs and working toward systemic solutions, we contributed to an evolution of the hospital’s capacity to provide high-quality psychiatric care long after our plane left the tarmac.
Conclusion: The Ripple Effect
The people impacted by this trip represent a circle of care that spans thousands of miles. The patients received focused, compassionate evidence-based care; the local residents and attendings gained a global perspective and shared their local expertise; the hospital moved a step closer to institutional excellence; and we, the Northwell residents, returned home with a profound understanding of the universalities and the unique cultural nuances of the human mind.
In Guyana, I learned that while the biology of mental illness may be universal, the path to healing is deeply local. The impact of this trip was not just in the treatments we prescribed, but in the bridges we built—between cultures, between systems, and between people. It was a reminder that global health is not about "saving" a community, but about joining one.