As a specialty certified pediatric anesthesiologist, I will be working in a regional pediatric hospital of Luang Prabang to teach principles and techniques of pediatric anesthesia to local nurse anesthetist students that are selected each year the Health Volunteers Overseas (HVO) program in Laos. The nurse anesthetists will remain in Laos to practice after their training is complete.
My responsibilities will include providing lectures, supervising in the operating room and teaching hands-on pediatric skills. The operating rooms are used every day for scheduled and emergency cases. Very few local anesthesiology providers have specialty training in pediatric anesthesia. Frequently, local adult anesthesiologists from the neighboring hospital visit Laos Friends Hospital for Children (LFHC) to increase their pediatric exposure and I would teach them pediatric anesthesia skills as well.
The local population of Luang Prabang, Laos, will benefit from this project. I have always had a strong interest in learning about other cultures through travel and service since I was a teenager. Prior to medical school I lived in South Korea for a year and a half and greatly enjoyed learning about their culture and medical practices. Since finishing medical training I have wanted to return to Southeast Asia to use my skills a physician to serve others abroad.
The HVO program in Luang Prabang, Laos, was established over three years ago and is oriented towards pediatric subspecialties. It operates year round with a variety of volunteer health care professionals rotating through for two weeks to one year rotations. The hospital is run by local health care professionals and the HVO volunteers work alongside them to assist with education and training and to introduce up-to-date medical practices.












Upon arrival in Luang Prabang airport, I was met with beautiful mountains, friendly people and a quiet peacefulness. Situated on the peninsula between the Mekong and Nam Khan river, Luang Prabang is known for its numerous Buddhist temples and monasteries. It is common place to see orange clad monks of various ages walking around the city. Lao Friends Hospital for Children (LFHC) is located on the outskirts of town immediately adjacent to the Provincial adult hospital and easily traveled to by tuktuk (motorized rickshaw) or bicycle.
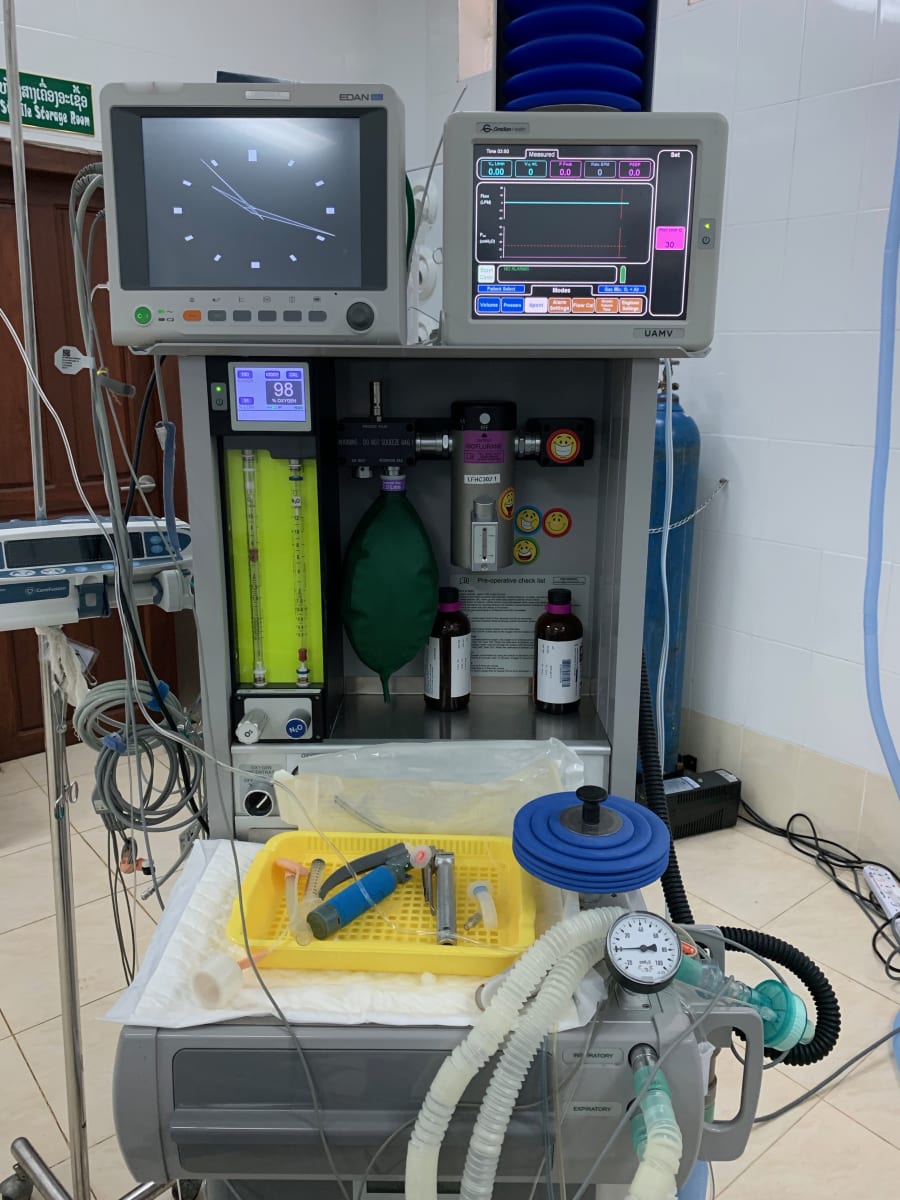
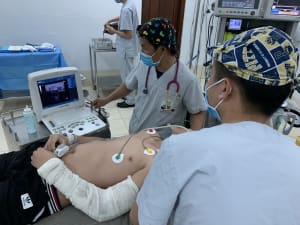
On my first day, I was greeted with a warm welcome by the hospital director and given a tour of the hospital which consisted of an inpatient ward, NICU, emergency room and a single operating room whose outer area served as both the preoperative and PACU area. What immediately struck me was how open everything was. There were no individual rooms and the waiting areas were all outside, in the open air with only a roof overhead. Due to the year round warm temperature, there is no need to have extra walls to protect oneself from the elements.
The operating room staff consisted of five people: three nurse anesthesia students, a circulator/scrub tech/sterilization processor and a first assist/operating room manager but no permanent anesthesiologist. There is a paucity of anesthesiologists in Laos, let alone pediatric anesthesiologists, and the students at LFHC are dependent on anesthesia volunteers for their training. That is exactly where the Health Volunteers Overseas project comes in. The overall goal of the LFHC project is to educate nurses to acquire the knowledge and skill to become nurse anesthetists. Established in October 2015, the nurse anesthetists complete a 2 year program with the majority of their training at LFHC except for a few months in Cambodia and Thailand. My role was to teach pediatric anesthesia focused lectures and clinical training.
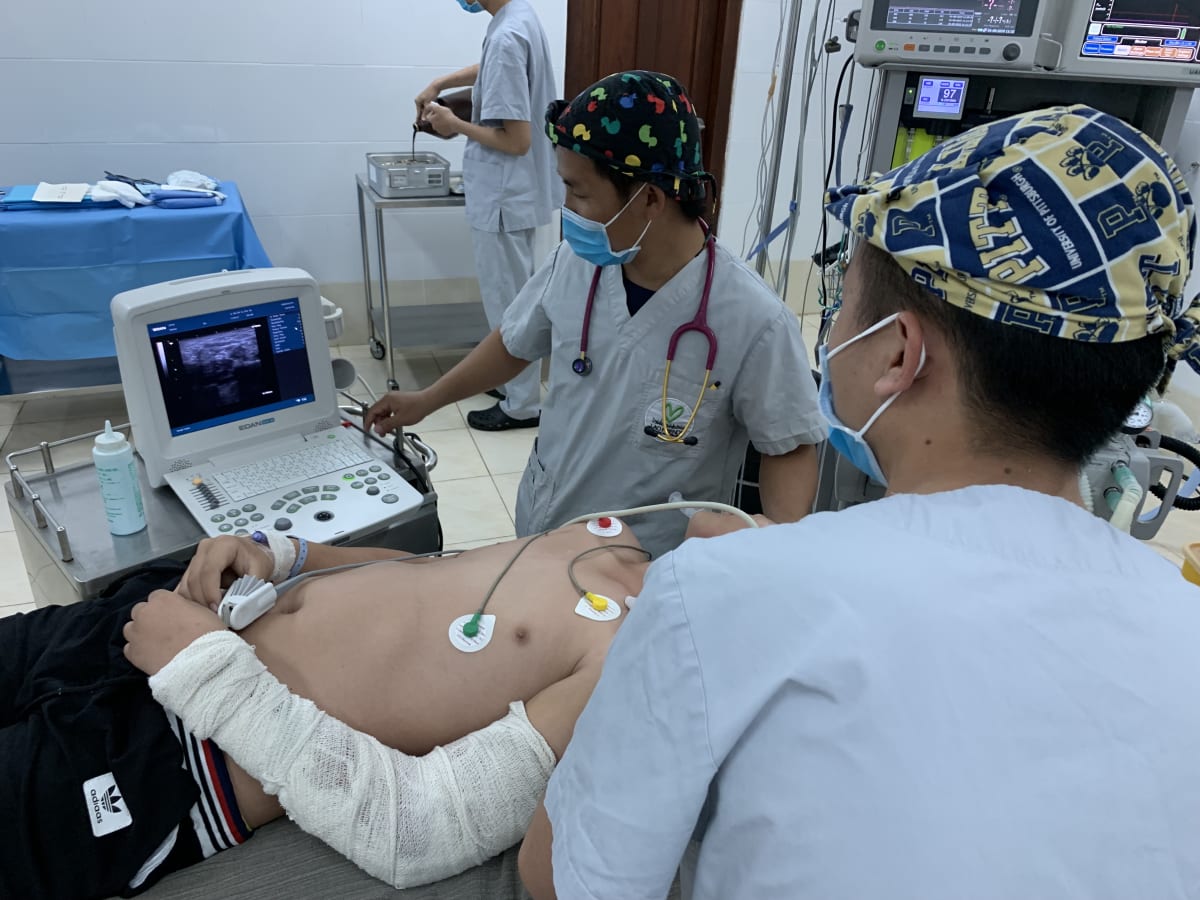
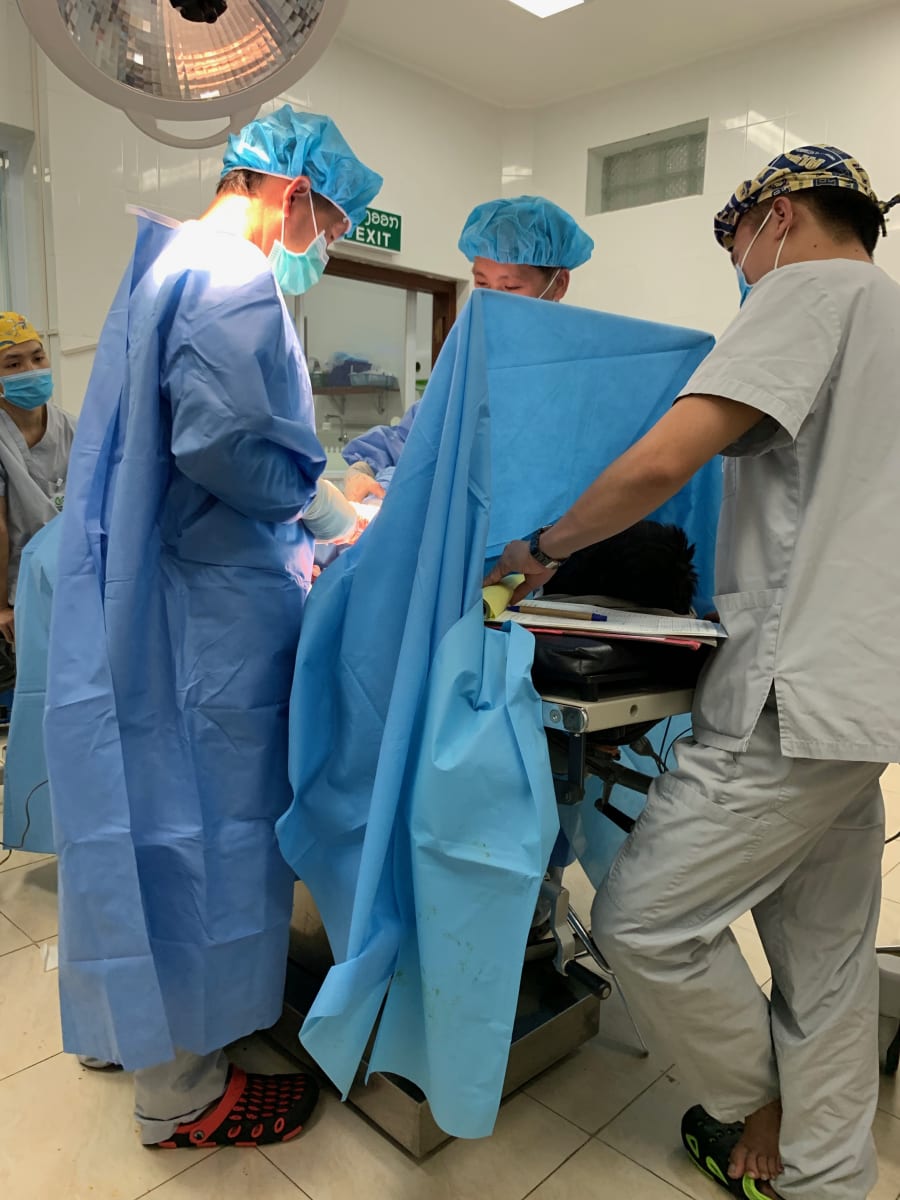
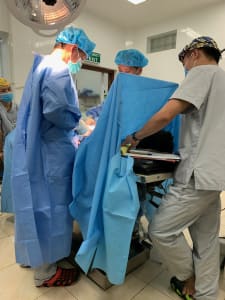
The nurse anesthesia students come from a variety of backgrounds from buffalo farmer to descendant of Hmong shaman; however, all have to obtain a nursing degree and display English proficiency prior to starting anesthesia training. Each day I worked with them I was struck by how hardworking, self-motivated and compassionate for children they were. We worked through a variety of cases to include ovarian teratoma, bowel obstructions, appendectomies, machete injury and numerous orthopedic surgeries. We used regional blocks when possible to avoid general anesthesia since availability of volatile agents is limited. I was amazed when a 5 year old patient was coaxed through a supraclavicular block with minimal IV sedation!
The students met each challenge head on with a “of course I can do that” attitude – unafraid to try something new they just learned from me or in a book. By the end of my stay, I realized I learned just as much from them as they learned from me. Thank you Dox Foundation for helping make this trip possible.