The purpose of the mission is to provide outpatient surgical care to indigenous Mayan children in the northwest section of the country. They have significant barriers to health care which impacts their short and long term health potential. We work in conjunction with the American College of Surgeons, Partner for Surgery and Asociación Compañero para Cirugía (ACPC) to facilitate access to our care for 75-100 patients, aged 0-18 in 1 week.
Indigenous Mayan residents in the northwest section of Guatemala. They have barriers to health care which include location, finances and language.
Similar to previous years, we expect to carry out successful surgeries for 75-100 Guatemalan children, who would otherwise not have access to these life changing surgeries and care. We anticipate this care to have life long benefits to these patients and their community.











Guatemala Surgical Mission
For the second consecutive year, I had the distinct privilege of traveling to Antigua, Guatemala to provide outpatient surgical care to indigenous Mayan children. These communities face significant barriers to healthcare, including geographic isolation, financial limitations, and language differences.
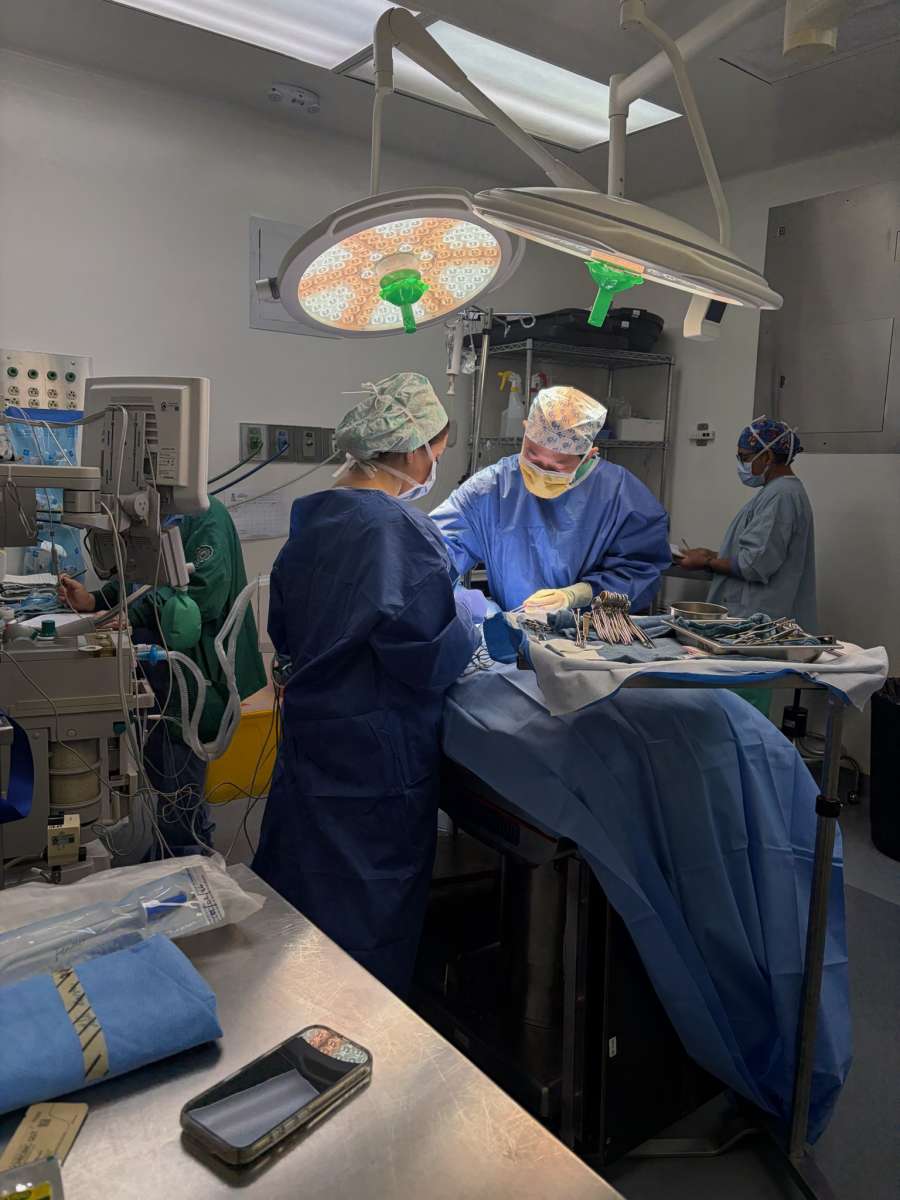
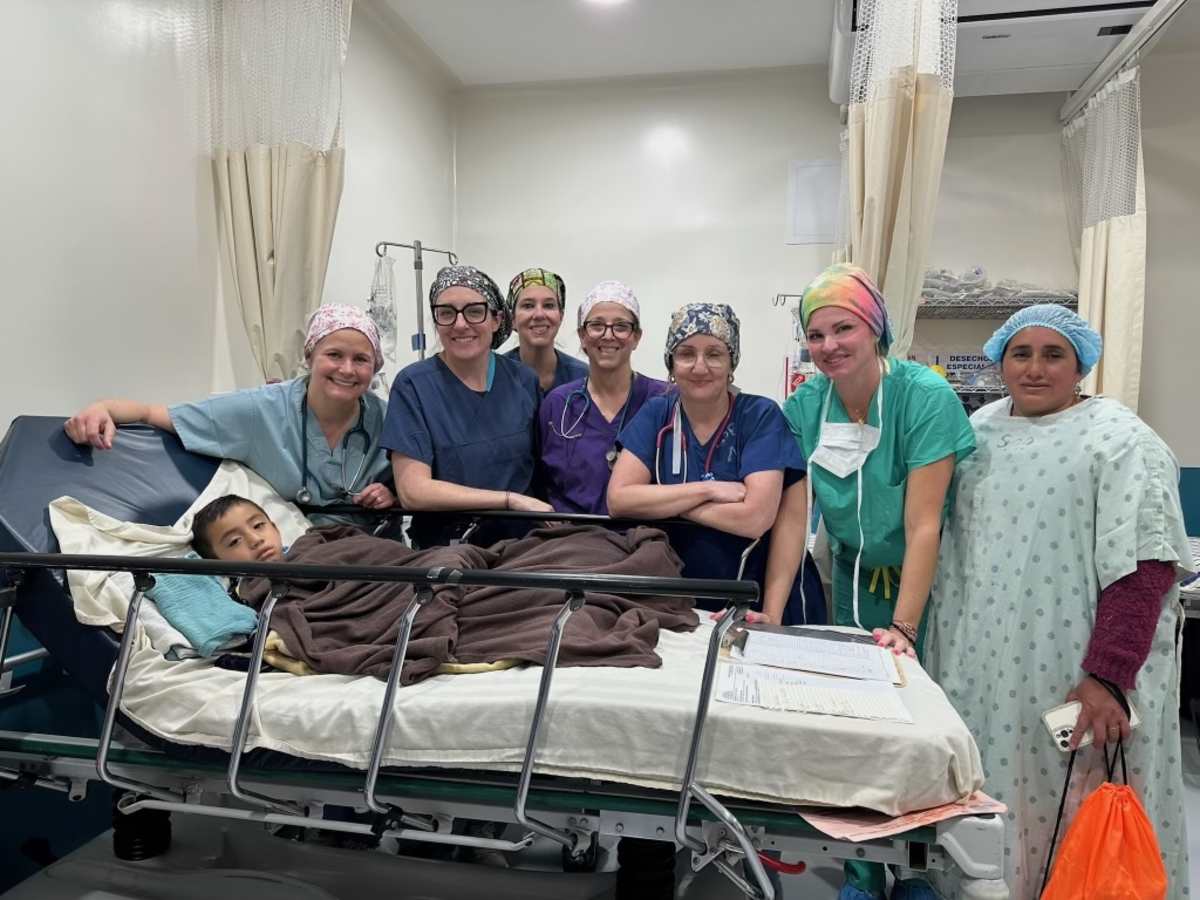
In partnership with Partners for Surgery, a nonprofit organization dedicated to connecting rural populations with essential medical care, our team—comprised of five surgeons and 17 additional colleagues in anesthesia, nursing, and advanced practice roles—completed 67 pediatric surgeries over seven days at Hermano Pedro Hospital.
Our first day was devoted entirely to clinic and triage—by far the longest and most demanding day. We evaluated more than 80 children with surgical needs, conducted comprehensive medical and anesthesia assessments, and scheduled five full days of operating room cases. Surgical procedures ranged from cyst excisions, inguinal and umbilical hernia repairs, orchiopexies, frenectomies, pilomatrixoma removals, and phimosis repairs. Our patients ranged in age from 5 months to 17 years- quite the scope!
The diversity in age, physiology, and developmental stages made postoperative care both intellectually stimulating and deeply meaningful. Supporting children as they emerged from anesthesia—comforting them through fear and uncertainty—was a profound privilege. Most recovered smoothly with minimal pain management needs. One child, however, experienced an unexpected and significant bronchospasm requiring postoperative respiratory support and airway management. Fortunately, within 36 hours he had improved remarkably and was discharged home with close outpatient follow-up. While most patients were able to return home the day after surgery, one child required a longer stay due to persistent drainage following cyst removal and placement of a Penrose drain.
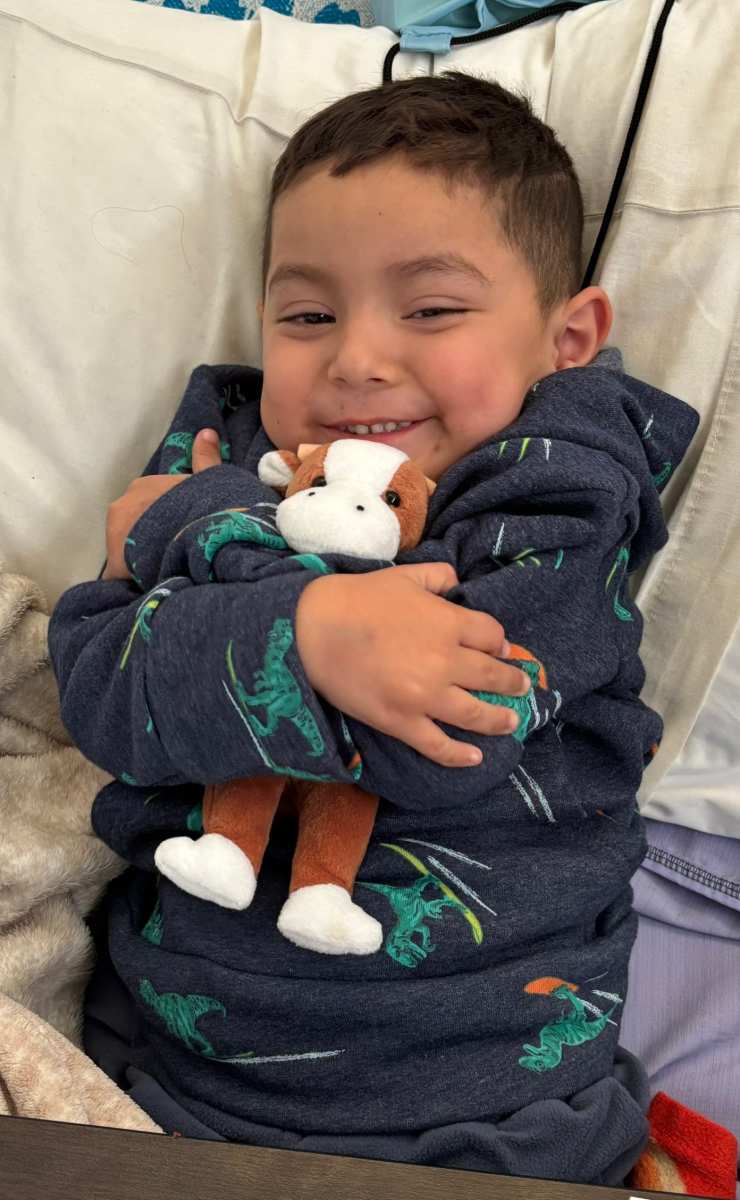
The gratitude of the children and their families is extraordinary. Many travel more than 18 hours to access care. Beyond addressing immediate surgical needs, these procedures help restore physical well-being and expand future opportunities for community welfare and employment. Despite language barriers, meaningful bonds form quickly. In the PACU, we were able to offer small toys, clothing items, and snacks—simple gestures that brought immense joy. The families’ appreciation, often for things we might take for granted in the United States, makes the experience deeply humbling and profoundly rewarding.
Despite long and demanding days, our team was able to experience the beauty and culture of Antigua. Each morning, we were greeted by the majestic Acatenango Volcano. We explored the historic Convento Santa Clara ruins and hiked to Cerro de la Cruz for panoramic views of the city. The vibrant central markets, rich Guatemalan coffee, and exceptional local cuisine made the experience even more memorable.
I look forward to returning each year for as long as I am able to serve.