Each year, I lead a group of Physician Assistant (PA) students from UT Southwestern to Sarstún, Guatemala—a remote coastal village accessible only by a long bus ride followed by a boat journey. I originally began participating in these trips as a PA student myself, and now serve as the lead PA and adjunct faculty mentor overseeing the clinical, educational, and logistical aspects of the experience.
During the trip, we provide much-needed primary care, women’s health, and basic surgical services to an underserved population with extremely limited access to medical care. We teach PA students hands-on clinical skills including patient interviewing, physical examination, diagnostic reasoning, procedural skills, and culturally competent care in a resource-limited setting. I also precept students in the operating room, where they learn principles of the sterile field, human anatomy, surgical decision-making, and operative technique, while gaining insight into how surgery is safely performed in low-resource environments.
This work creates both immediate and lasting impact. For the Sarstún community, our presence provides access to medical evaluation, treatment, education, and surgical intervention that may otherwise be unavailable. For patients, this often means relief from chronic conditions, earlier diagnosis of serious disease, and improved quality of life.
For PA students, the impact is transformative. Exposure to global health and surgical care early in training shapes them into more adaptable, empathetic, and socially responsible clinicians. Many alumni of these trips go on to work in underserved settings, public health, or global medicine, multiplying the long-term effect well beyond the single week in Guatemala.
This project benefits two primary populations: the residents of Sarstún, Guatemala, and Physician Assistant (PA) students in training. Sarstún is an extremely remote coastal community with limited infrastructure and minimal access to consistent medical or surgical care. Geographic isolation, transportation barriers, and resource constraints make it difficult for residents to seek care elsewhere, resulting in delayed diagnoses, unmanaged chronic disease, and preventable complications. This population is chosen because the need is profound, persistent, and underserved, and because consistent annual engagement allows for continuity of care and trust-building within the community.
Patients in Sarstún benefit through access to primary care, women’s health services, preventive care, and surgical interventions that may otherwise be unavailable. Importantly, we are able to provide laparoscopic surgical care, which significantly reduces postoperative pain, shortens recovery time, and lowers complication rates. Without access to laparoscopy, many of these patients would otherwise require open abdominal procedures, resulting in longer hospital stays, delayed return to work and family responsibilities, and increased risk of complications. Providing minimally invasive surgery in this setting meaningfully improves patient outcomes and quality of life.
PA students also benefit significantly from this project. By working directly with underserved patients in a low-resource setting, students develop strong clinical reasoning skills, cultural humility, and adaptability. They gain exposure to surgical principles, sterile technique, anatomy, and operative care in austere environments, while learning how advanced surgical techniques like laparoscopy can be safely and ethically implemented in resource-limited settings.
The expected impact of this project is both immediate and enduring. In the short term, patients in Sarstún receive access to comprehensive medical care, women’s health services, and advanced surgical interventions, including laparoscopy, which would otherwise be unavailable. This leads to improved clinical outcomes, reduced postoperative complications, faster recovery times, and meaningful improvements in patients’ quality of life. Ongoing annual engagement also allows for continuity of care, follow-up, and trust-building within the community.
Beyond direct patient care, the project has a lasting educational impact on PA students. Students gain invaluable experience in clinical reasoning, procedural skills, and surgical principles in a low-resource setting, learning to practice high-quality medicine without reliance on advanced diagnostics. They develop cultural humility, adaptability, and leadership skills that shape their approach to patient care long after the trip ends.
Upon returning, PA students are required to develop and present a global health reflection presentation to their classmates, allowing them to critically analyze their experience, share clinical and cultural lessons learned, and extend the impact of the trip to the broader PA program. Students carry these experiences into their clinical rotations and future careers, with many choosing to work in underserved, rural, or global health settings. Additionally, insights gained from delivering laparoscopic care in austere environments inform best practices in efficiency, safety, and innovation, which can be applied across diverse healthcare systems and clinical settings.




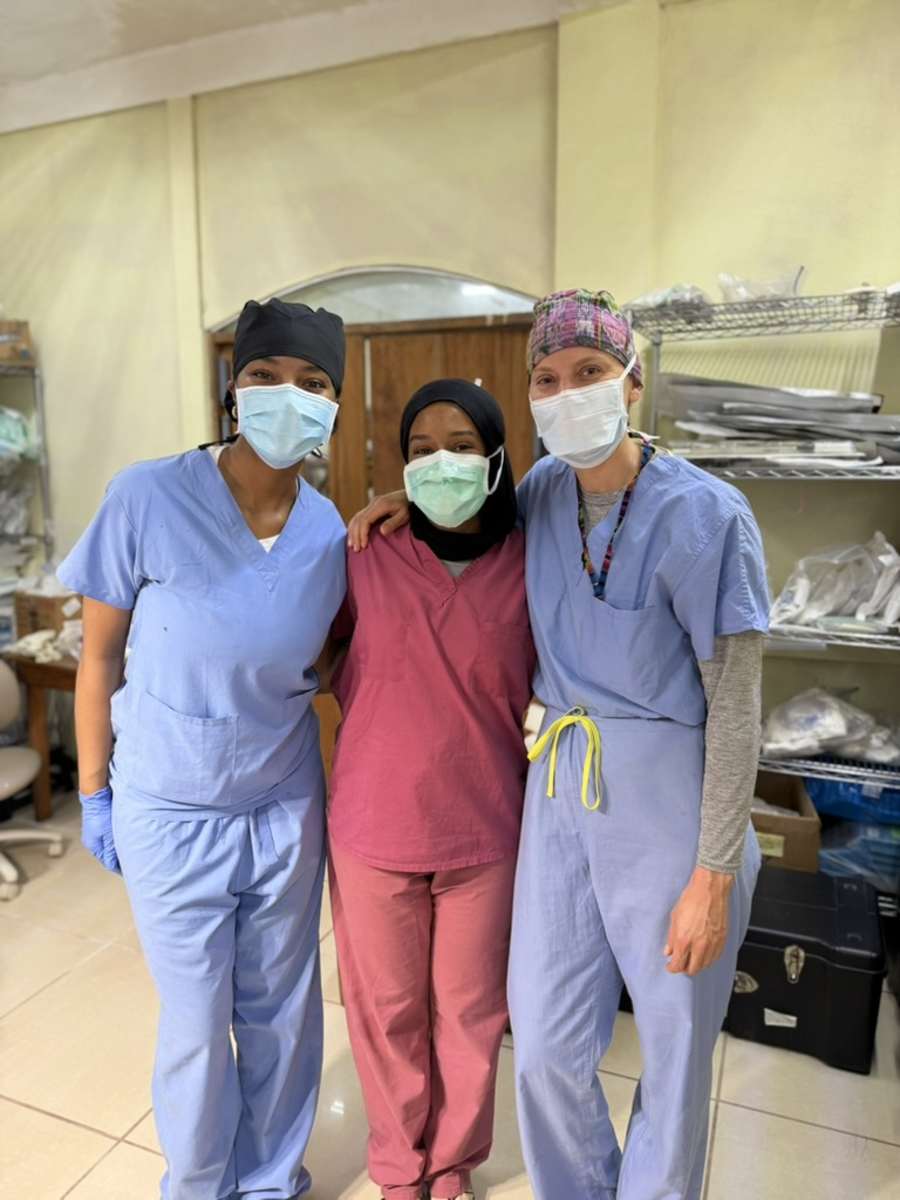











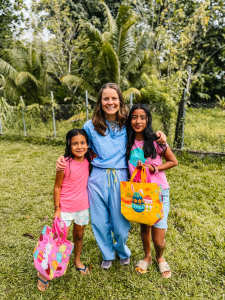
This trip to Sarstún, Guatemala impacted multiple groups in meaningful and lasting ways—most notably the local community, the PA students who participated, and the children of Sarstún who have become a special part of this experience for me.
Within the community of Sarstún and surrounding areas, we cared for 192 patients in clinic, performed 72 on-site laboratory tests, evaluated 18 patients for surgical needs, and completed 13 surgeries, in addition to prescribing 292 medications. These numbers reflect more than just volume—they represent individuals who often have limited or no access to consistent medical care. By providing both clinical and surgical services, including minimally invasive procedures that are not typically available locally, we were able to reduce suffering, improve recovery times, and address conditions that may have otherwise gone untreated.
The impact extended beyond patient care to the PA students who joined the trip. They were immersed in both clinic and surgical settings, many experiencing the operating room for the first time. This hands-on exposure allowed them to develop clinical skills, understand surgical workflows, and gain confidence in a way that cannot be replicated in a traditional classroom. Just as importantly, they witnessed the importance of adaptability, cultural humility, and service—lessons that will shape how they practice medicine in the future.
On a more personal level, the children of Sarstún continue to leave a lasting impression on me. Each year I return, I am greeted by familiar faces—young girls in particular who I have watched grow over time. Their excitement, resilience, and joy are constant reminders of the human connection behind this work. After long days in the operating room, spending time playing with them brings balance and purpose to the experience. These relationships transform the trip from a short-term mission into a meaningful, ongoing connection with the community.
Overall, this experience highlights the layered impact of global health work—improving access to care for patients, shaping the next generation of providers, and fostering genuine, lasting relationships within the community we serve.