In March, I will travel to Vietnam as part of a surgical outreach team providing direct clinical care to underserved patients through a combined outpatient clinic and operative experience. Our team will evaluate local patients with a wide range of reconstructive and functional needs, coordinate surgical planning, and perform necessary procedures that may otherwise be inaccessible due to geographic, financial, or system-level barriers. This trip will allow us to deliver immediate, high-impact care for individuals who often face prolonged delays or complete lack of access to specialty surgical services.
The most important component of this project, however, is that it is built around developing a sustainable system of care. Rather than providing one-time interventions, our program prioritizes collaboration with local healthcare professionals to strengthen long-term capacity. This includes working alongside local physicians and staff, supporting shared operative and clinical decision-making, and building systems that can be continued and expanded after our team leaves. We aim to contribute to continuity of care through structured follow-up planning, knowledge exchange, and clinical workflows that help support future patient evaluation and treatment.
This experience will make a difference by improving patient outcomes both immediately and long-term: providing life-changing reconstructive surgery to patients in need while also supporting a framework for ongoing access to surgical care within the local community. It will also strengthen my development as a surgeon committed to ethical global health partnerships, sustainable care models, and service-driven leadership.
This project will directly benefit patients in Vietnam who have limited access to specialty surgical care, particularly individuals from underserved or resource-limited communities where barriers such as cost, transportation, and shortage of subspecialty providers can prevent timely treatment. Many patients present with conditions that significantly impact daily function, health, and quality of life, yet are highly treatable with appropriate surgical evaluation and intervention. Through a combined clinic and operative experience, we will serve local patients who may otherwise face long delays or may never have the opportunity to receive reconstructive and functional surgery.
This population is prioritized because the burden of unmet surgical needs is high, and disparities in access to surgical care can have lifelong consequences. In many cases, treatable conditions may progress over time, leading to worsening disability, chronic pain, inability to work, social stigma, and preventable complications. Providing care in this setting has the potential to create immediate, meaningful impact for individuals and families.
Importantly, this project is designed not only to provide care during the trip, but also to strengthen sustainable access to treatment for this community. By collaborating with local healthcare teams, supporting shared clinical decision-making, and contributing to systems that enable continuity of care and future treatment planning, we aim to help expand long-term surgical capacity beyond our visit. Ultimately, the patients we serve—and the local clinicians supporting them—will benefit from both direct surgical care and a stronger foundation for ongoing, accessible treatment within the region.
After returning, I plan to carry these lessons forward in my training and future practice by continuing to pursue sustainable outreach partnerships, incorporating efficient and equitable care strategies into my daily clinical decision-making, and sharing insights with colleagues and trainees to strengthen service-driven, high-impact surgical care.
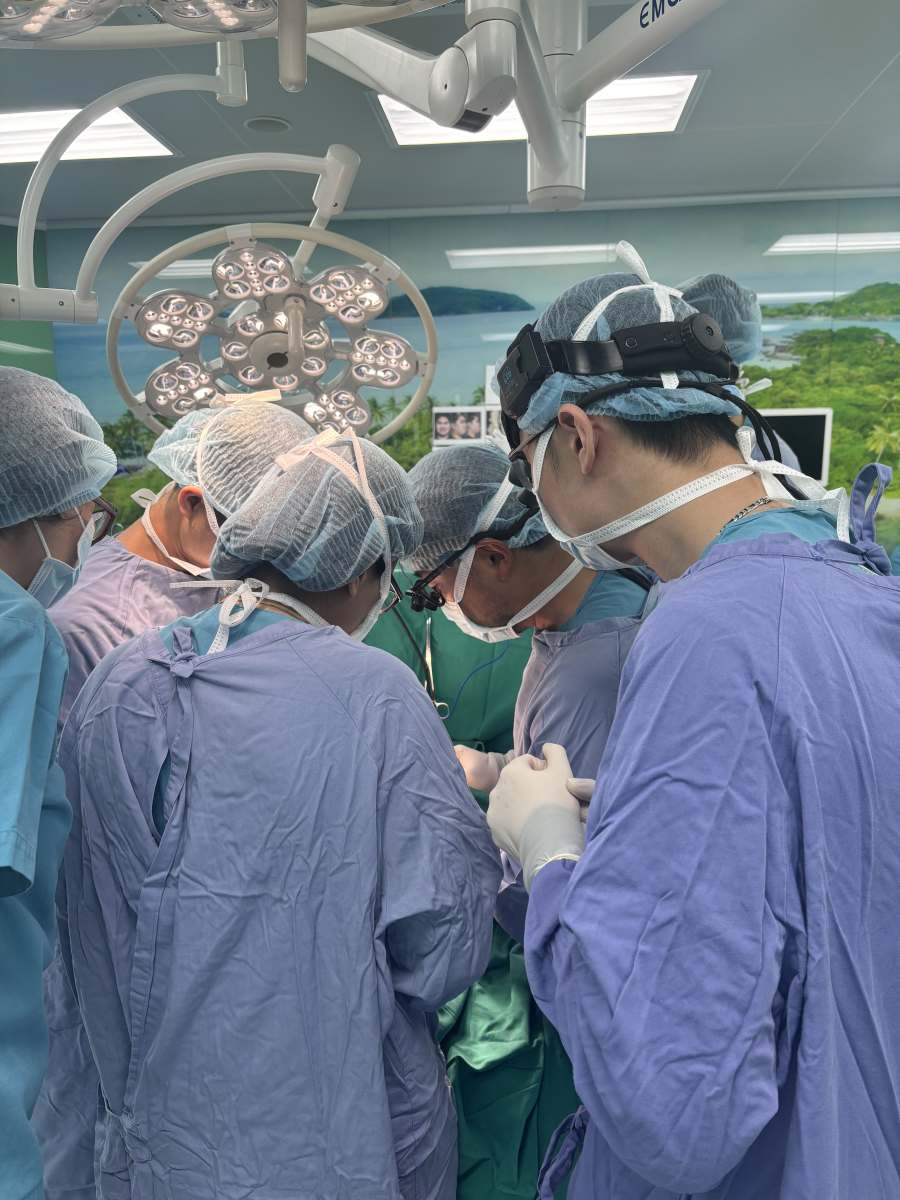









My four days of clinical observation across Hanoi were among the most formative of my residency. At the National Children's Hospital, I was struck by the volume and acuity of pediatric patients, many presenting with conditions that had gone untreated far longer than I'm accustomed to seeing, a sobering reminder of what access to care actually means. Two days at Hong Ngoc pushed me to watch more carefully and assume less. A high-volume private environment where surgical efficiency and adaptability were on full display. Viet Duc University Hospital, one of Vietnam's most respected surgical institutions, was a fitting close: complex cases, calm hands, and a teaching culture that reminded me why I chose this field. Across all four days, what humbled me most was witnessing surgeons build careers of genuine impact with a fraction of the resources I'll have and doing it without complaint, with excellence, and with clear devotion to their patients.