This is a Visiting Educator Trip, with a primary focus on providing education for local medical practitioners. The goal is to assist the local team in providing needed medical care in their country. I participated in a similar trip in November, 2025 to the same site. At that time our team was able to begin modeling some of the processes which are considered important in ensuring patient safety (Surgical Safety Checklist, and Patient Identification) On this trip I would like to continue to model these processes in conjuction with others on the trip. Additionally I hope to present the concept of Early Warning Systems to identify patients who are at risk for medical deterioration before the actual deterioration becomes urgent or irreversible. The host surgeon has indicated that at this site they are experiencing unanticipated losses of patients who seemed stable at the time. They are looking for ways to prevent this. Many countries have been using an early warning system and have found it to be helpful in preventing unexpected deaths in post surgical and intensive care units. These systems have been trialed in clinical settings, and found to be successful lowering unexpected deaths. I would like to introduce both the concept and the actual systems which are in use (MEWS, PEWS, qSOFA and others). Additionally I would like to reinforce the concept of preoperative screening for elective surgeries, with the goal of identifying patients who are at risk for poor surgical outcomes and may require special interventions or precautions if surgery is considered.
The prime beneficiaries of the project would be the patients. Patients in burn care units and intensive care units would benefit from early detection of deteriorating status, and prompt preventative intervention. Patients being considered for elective surgery will benefit from standardized patient screening to determine what preoperative interventions could increase their chances of safe and successful surgery.
The practitioners targeted will be physician/surgeons, fellows in training, medical interns and residents and nursing staff.
The goal is to model and encourage the use of patient screening and specific monitoring to allow early intervention in case of deteriorating medical status and to prevent problems during elective surgery by careful preoperative screening.
We hope to identify committed medical practitioners locally who can carry on the processes which are introduced. The concepts are not difficult, but do require a local "champion". We expect to include the current trainees as they will be able to include screening and monitoring systems as they continue in practice. It is anticipated including these processes in a graining program that there use will become more standard.Including the nursing staff will encourage them to be part of the medical team and will hopefully increase their comfort in advocating for their patients.












ReSurge Medical Teaching trip to Uganda (ST3 trip) March 1-7 2026
First of all I would like to thank the Doximity Foundation for supporting ReSurge International in their effort to expand surgical capacity in low resource countries. ReSurge has moved from “giving fish” by taking teams into low resource countries to perform surgeries, to “teaching how to fish” by supporting training programs in those countries. The countries with whom we work have dedicated and very competent people, but struggle with “not enough” . Not enough funds, not enough schools and training programs, not enough surgeons, not enough specialists, not enough nurses. By underwriting the travel costs for many medical professionals, the Doximity Foundation helps ReSurge to support training programs across the globe.
I first went to Uganda in November 2025. The trip was short, just five days, and I wondered what I could do in that amount of time. It was a wonderful introduction, but was an introduction. It took me the entire time to begin to understand the work flows, the goals and the hopes of our hosts. I volunteered to return in March 2026 with hopes of taking a few more steps.
This was an interesting trip. My flight from San Francisco to Dubai (the first leg of the journey) was interrupted (while we were in the air about 3 hours from Dubai) by the closure of the Dubai air space. That necessitated a U turn to land Munich, and a scramble to find an alternate flight to Uganda. The same situation meant that our two surgeons and two anesthesiologists, who flights left a day after mine, were essentially grounded and unable to participate in the mission. That left us with two of the ReSurge staff who were coming to work with our hosts on next steps, two recovery room nurses, one operating room nurse, a nurse educator in burn care, a hand therapist and myself, a pediatrician. Fortunately our hosts had their local team of plastic and reconstructive surgeons, anesthesiologists and some nursing staff.
Our first day was spent examining the patients who had gathered from around the country, and planning the surgery schedule. These exams are necessary to ensure that the surgery planned is one that will provide the maximum benefit to the patient with the least risk, taking into account surgical expertise, equipment and supplies available , and the patients goals and needs. The following days were full of the surgeries themselves, as well as talks on subjects that our hosts had requested, and ward rounds. As a pediatrician, my position was supportive, but a little nebulous. There was no Pediatric Department in the hospital where the burn center was (Kiruddu National Referral Hospital) , so I spent my time interacting with the surgeons, the anesthesiologists and the interns on the ward, as well as with the nursing staff in the general ICU unit (as opposed to the ICU room on the burn ward).
What was our impact, and who did we personally impact ? There is not an easy answer. It is difficult to point to what one achieves on such a trip. Change comes slowly, and suggestions for new work flows, new safety measures and improvement in infection control need to be made very tactfully. After all, these are clinicians who spend every day doing what is possible when the burdens of illness and injury are large, and the resources limited. We spent time sharing: Finding out what the processes and care plans our hosts use, and modeling ones we have found useful, and learning from one another. We also tried to model the team concept of mutual respect, and valuing input from all team members. 70 years of a ridged colonial system had bequeathed a hierarchy system and barriers are still being dismantled. We hope that our examples will seed some ideas. As one intern pointed out…”you are a fully trained pediatrician, and you talk to me, an intern” She was rather astonished, but gratified. Patients were also surprised, at times, to have us take time to answer questions, to help them solve minor problems. Not that the host physicians were not equally concerned and helpful…it simply had not occurred to the patients to ask.
The burden of burns in Uganda is staggering. The very simple homes in the villages and suburbs often have an open fire where food is cooked, and over half of the burns are a result of upsetting a container of boiling liquid, or of falling into a cooking pot, or into the fire itself. Children from ages two to five are at the greatest risk. 80% of burns occur in children less than 10 years.
Once a burn occurs, the first treatment used by parents and caretakers are often aloe, cooking oil or urine. Only when the burn does not heal, or the child gets sicker after sustaining the burn, do the families, who can ill afford the costs and time to travel, seek medical care. frequently in a small regional hospital. Almost 400 children a year end up coming, or being referred to Kiruddu Hospital, and often days after the burn.
The best outcome for burn injuries requires prompt and specific care, with appropriate fluid management, infection control, and early grafting, all of which are not easily accessed by the majority of the population. The staff at Kiruddu must try with limited resources to do what is possible to optimize care when the patients arrive.
Then there is the equally great burden of trying to help patients with debilitating burn scars. Scar tissue of any kind is particularly strong, and without splints, compression garments and constant and specific exercise, the healing burn wound is pulled into and fixed in very abnormal positions. A burned upper arm is often pulled down and fixed to the chest, so that the person cannot lift or move the arm. Burns of the palm are pulled into a “mitten deformity” or are actually fused to the forearm, rendering the hand useless. Chins are pulled to the chest, and the entire face is distorted. Skilled surgeons work to correct these deformities, often in stages. In three hours they can release fingers from their bent position, place a skin graft over the defect created, and splint the hand in a more normal position. If all goes well, and the graft heals well, and the parents help the child to exercise the hand, the child will be able to pick up a pencil and eventually write, they will be able use the hand to open a bottle, to sew, to type and to attend school and learn a trade. Had they had access to immediate and more comprehensive care, the deformity could have been largely prevented.
What was our impact? There were baby steps : a new work flow to shorten times between surgeries, tips on bandaging fresh burns so that more movement was possible during the healing, validating a mother’s care for her burned infant so that she could keep up with needed exercises. We tried to introduce an early warning system so that patients who were not doing well could more easily be identified on a busy ward. I continued to fill out and model the patient information sheets, to give the anesthesiologist the information needed for safe anesthesia. And in the background we formulated dreams: educational programs and governmental inititiatives which could address the causes of burns and barriers to early care. And overall we tried to support our hosts in what they do and keep the patient and their well being as our focus.
I certainly came away, once more, with admiration for our hosts and their dedication in the face of overwhelming need and minimal resources. And I was impressed with patience with which the people waited, and hoped. And the smiles…so many smiles!
Photos: from L: Team members with our hosts…myself on R
A patient getting a dressing change in the waiting room
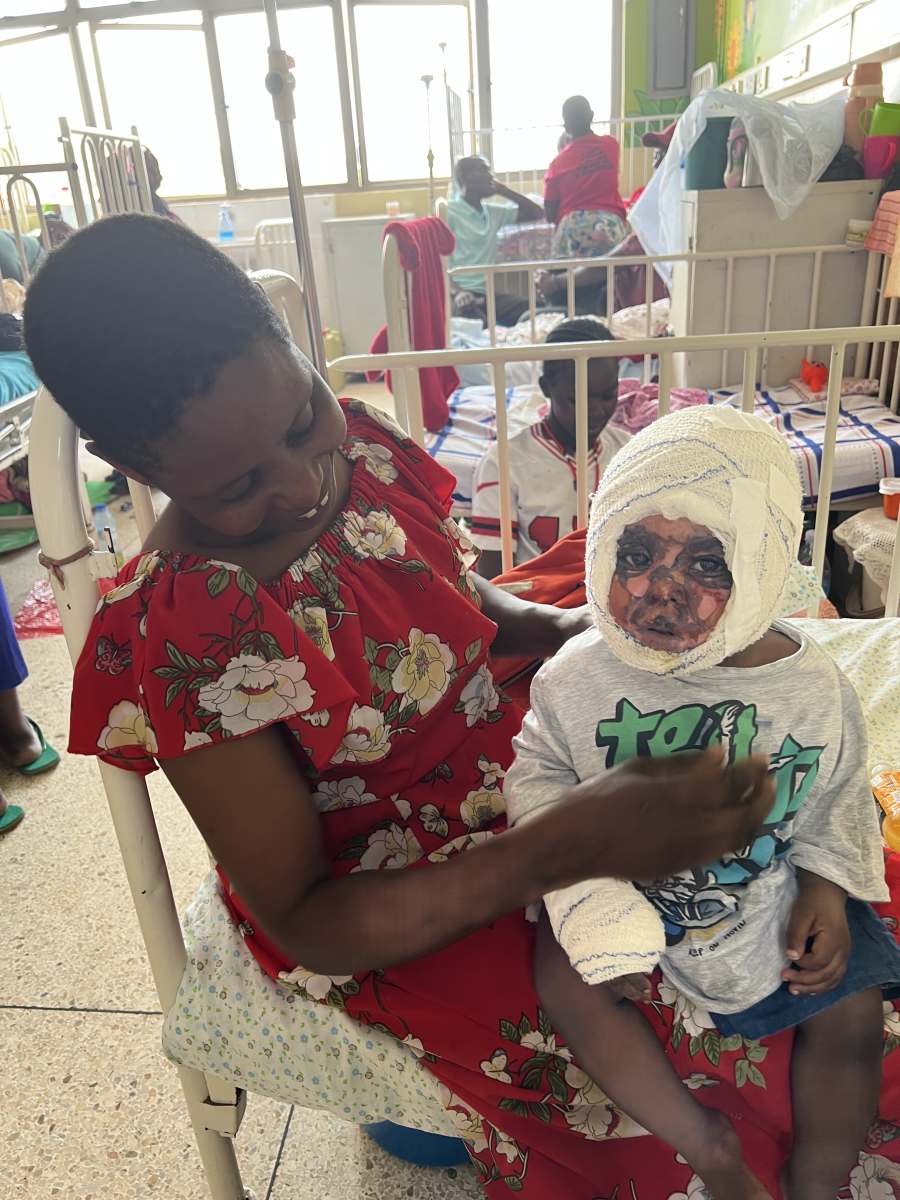
Mother and child
Bedside rounds, intern presenting
Talk on Sepsis
Patients on the ward, folding bandages