I founded the Alliance for International Medicine in 2015 after observing on a number of medical missions that there was virtually no coordination or support with local healthcare workers, and difficulty providing any sustainability of quality healthcare in our absence. Our organization therefore provides surgical and anesthesia equipment, training, and medical care in resource-restricted countries. In 2018 we trained the anesthesiologists and surgeons in Piura, Peru in advanced laparoscopic techniques and ultrasound guided regional anesthesia in a hospital that has limited to no access to opioids. We have tracked our outcomes with a 96% success rate in attempted regional anesthesia blocks, and are presenting our findings at the Yale Global Health and Social Innovation Conference this April. Dr. Richards will be filing a separate travel request discussing his success in laparoscopic training.
Having implemented our program in Regional and Santa Rosa hospitals in Piura, Peru, we are now hoping to return the first week in June to introduce more blocks (abdominal and chest wall blocks), open up a new program in Sullana 30 minutes north of Piura in a hospital for the poor, and provide both new ultrasound machines to compliment the previous machines we donated, and to train their bioengineer people in equipment maintenance. My colleague, Dr. Nate Richards, donated two laparoscopic trainers with our last visit, and will be building on that experience. We are continuing to develop our internet training portal where our international colleagues can train online before and after our training. We are expanding to Ghana where Nate and I lectured and partnered with four hospitals last year.
We know from our data that ultrasound-guided regional anesthesia can provide excellent pain relief to patients who have virtually no access to opioids after painful surgeries/traumatic injuries. Their success rate of over 96% in attempted blocks in over 100 patients in six months will hopefully be accepted for publication soon. On this trip we are going to work towards developing block teams in Piura, and a Palliative Care Service, and start the basic program in Sullana. We have data models we are studying, and I am submitting our data to be published this year. We are also going to start tracking hospital savings through decreased length of stays, earlier return to work, and decreased medical costs as regional anesthesia can be provided very inexpensively as long as the ultrasound costs are covered. We have been paying for all these costs ourselves, and currently looking to raise more money, just formed a board of directors, etc...Training continues through our internet education portal, teleconferencing, and annual visits. We believe in long-term sustainability, and we are already seeing Piura become a Center for Excellence in Peru for ultrasound guided anesthesia!
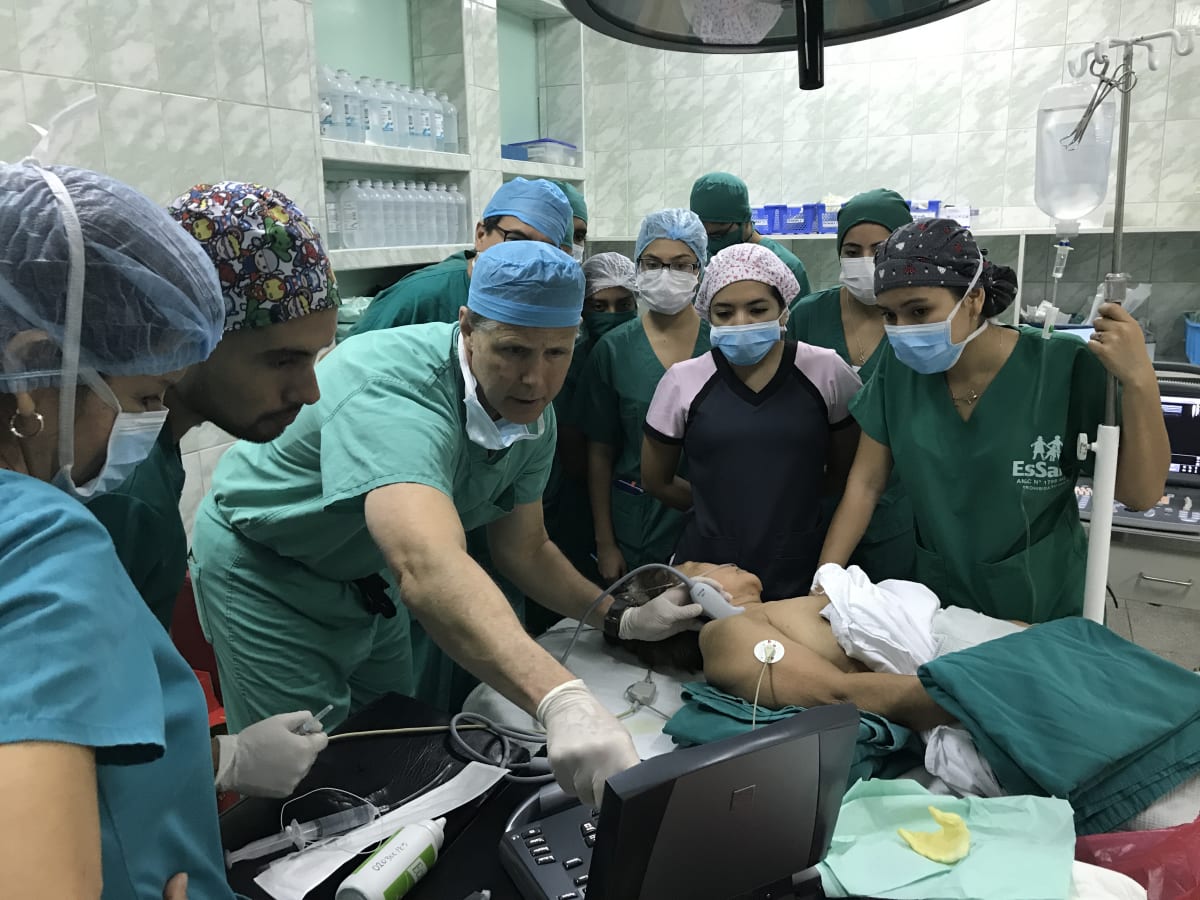




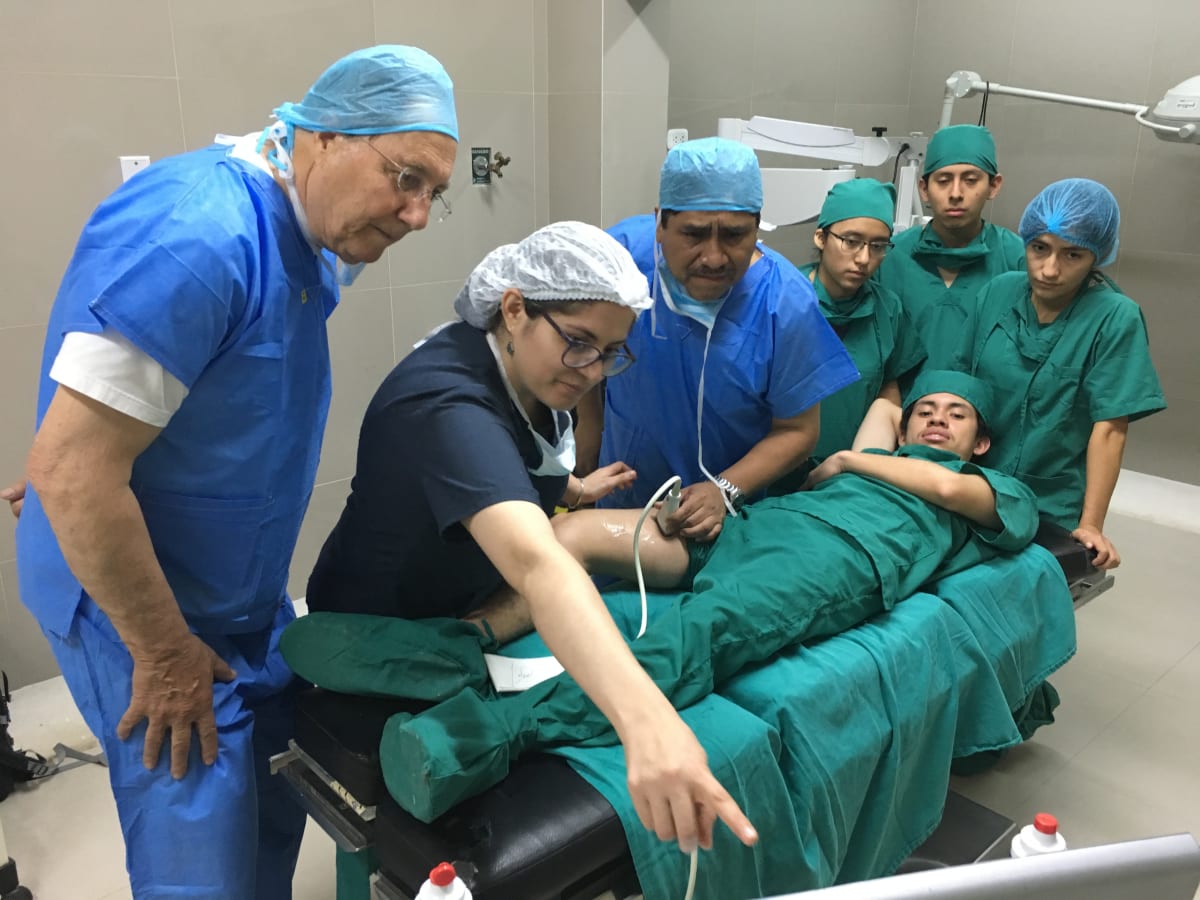









The Alliance for International Medicine returned to Piura, Peru to continue our mission of teaching ultrasound-guided regional anesthesia (UGRA) in hospitals where they have limited access to opioid pain medications. After our initial training trip in 2018, we collected 15 months of data showing our colleagues had a >93% success rate in administering UGRA in upper extremity, lower extremity and abdominal surgeries. On this visit we introduced more advanced UGRA techniques, including catheter placement and the organization of regional block teams. We were also able to expand our program to a third hospital. Thus far, our organization has donated 4 ultrasound machines and over $100,000 in supplies, and continue to mentor and teach our colleagues who are rapidly becoming self-sufficient. We are also expanding to teach lung ultrasound and cardiac ECHO, as many of these hospitals no longer have x-ray film and limited diagnostic imaging capability.
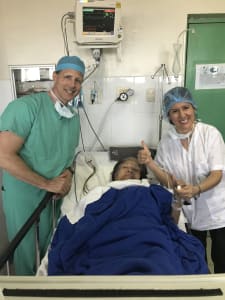
These photos reflect some of the people whom we were able to help—a 60-year old woman with an humeral fracture after an interscalene block and open repair; and a 12-year old girl who in this photo is less than 24-hours out from multi-injection TAP blocks and laparoscopic splenectomy, and has only taken two Tylenol. While the pain control is important, it is also resulting in shorter hospital stays and a more rapid return to work. For countries where patients can save for years to afford surgery, this cost-savings comes back to them, in addition to the ability to return to their employment or school at a much earlier date. More importantly, the physicians who we trained in Piura are now establishing UGRA as a regional standard of care, and are expanding and deepening their expertise to teach and train others in their communities.
We would like to thank Doximity for their financial support of our ongoing mission. Because of their generous donation, we were able to transport and donate more medical supplies than anticipated, which not only impacted patient lives during our visit, but will continue to bless the entire community with improved healthcare for years to come.