In January to February 2020, I will be volunteering at Kijabe hospital in Kijabe, Kenya for a period of 4 weeks. At this site, I will be interpreting a variety of x-rays, CT’s, and MRI’s. Given the complex pathology at the site and absence of local diagnostic radiologists, we hope to help the hospital physicians with ordering and interpreting images. In addition, I will be performing some image-guided procedures, such as ultrasound guided paracentesis and thoracentesis. Attending radiologists from Wake Forest Baptist Medical Center will be available for supervision of our image interpretations and procedures.
In addition, we will be teaching x-ray, CT, and ultrasound protocols to the technologists. We will be providing an educational powerpoint to explain the nuances of each protocol and the rationale of each sequence. We hope to improve the method of obtaining imaging at the site, which will hopefully continue the work to standardize imaging. We also hope to provide a template for future examinations.
Lastly, we will provide a series of educational presentations to the housestaff and attendings. Specifically, we will provide educational presentations regarding cross-sectional imaging, such as CT’s and MRI’s. We will provide a detailed talk with expected normal anatomy and a variety of pathology, typically ones seen in the region. As my interest is in abdominal imaging, I will provide an educational exhibit on abdominal CT. My colleagues will likely provide exhibits regarding pediatric and neurologic anatomy and pathology.
The local patient population at Kijabe hospital include the Kikuyu, the Masai, and Sudanese people in the area. Patients are generally from an impoverished background and have to pay out of pocket for care. We expect to provide direct radiology interpretations and education not only to the hospital physicians but also directly to patients. In concert with the local physicians, we will discuss diagnosis, prognosis, and treatment plans. We hope to provide accurate diagnosis to their ailments and provide minimally invasive diagnostic procedures that may not be otherwise available.
Our long-term goal is to provide year round radiology service for Kijabe hospital. In our time there, we will continue to build on the work performed by Wake Forest residents and attendings who have participated in the past 5 years. In addition to image interpretation, procedures, standardization of imaging techniques, and improved image quality, we hope to provide radiology resident and attending coverage at Kijabe hospital to several months per year. We have been working with the program director and chairman at Wake Forest Radiology to provide a formal global health rotation in our residency with our emphasis on Kijabe, Kenya. Following graduation of residency, I hope to return to Kijabe, Kenya to aid other residents as a supervising attending. We hope to use the experience from our former residents and fellows to build a group of radiologists able to serve as adjunct radiology faculty in Kenya.



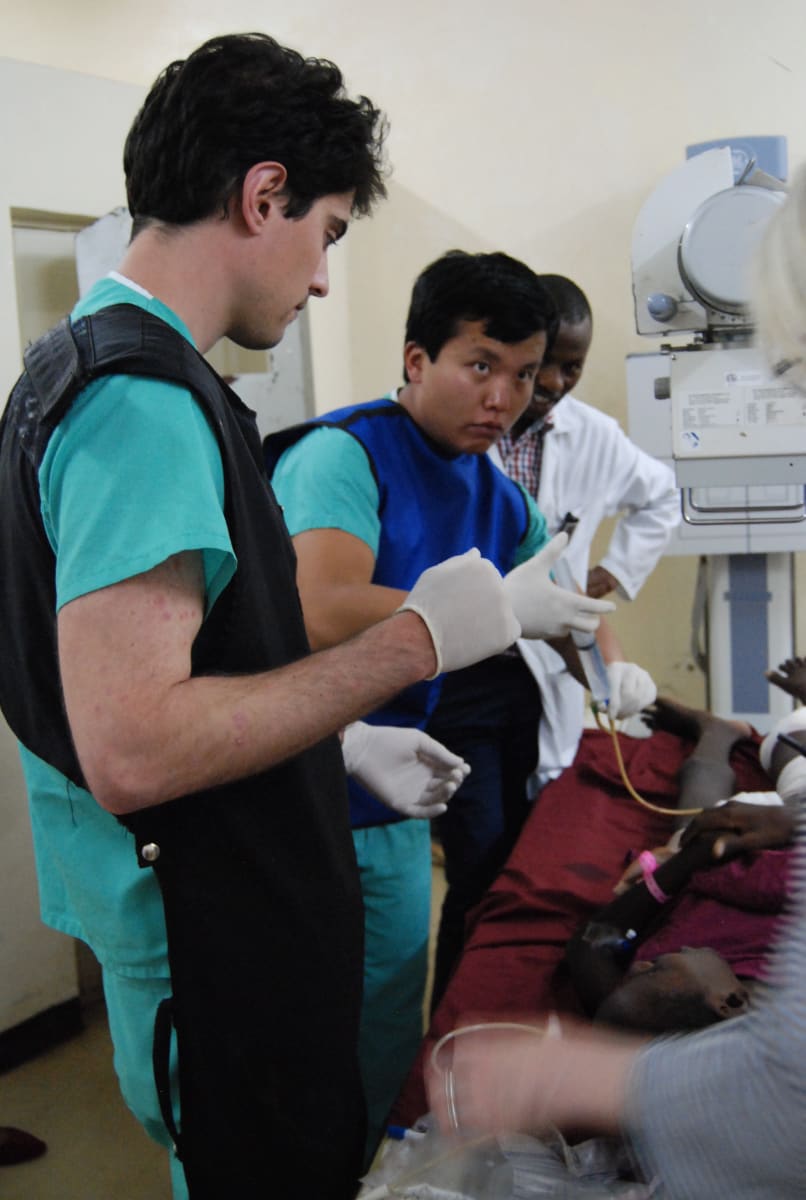





Wake Forest Radiology- Kijabe Hospital, Kijabe, Kenya
In January-February 2020, our team of radiologists traveled to Kijabe, Kenya. This trip has been an amazing opportunity to teach and to learn. Two other senior radiology residents and I (also a senior radiology resident) composed of the primary team serving Kijabe Hospital.
While the imaging modalities are similar compared to the US, including X-rays, CT, and ultrasound, we had the opportunity to work with a wonderful and dedicated group of technologists. Every single day, we worked with technologist on CT protocols, reading and reporting CTs, as well as brief tutorials and explanation on the rationale of the examination. As Kijabe hospital lacked a dedicated radiologist, we had numerous interactions with technologists everyday, when we were able to teach and solidify the knowledge base of the local technologists.
In addition, we had numerous consultations from inpatient and outpatient providers at the hospital. The providers had numerous studies including X-rays, CTs, and MRI examinations performed at outside hospitals requesting our formal reads and reports. These interactions are nearly a thing of the past in the US, however, in Kijabe, in-person consultations are very much a part of our daily work. I truly enjoyed helping providers troubleshoot through these examinations.
Starting on our first day, we were tasked with educating residents in our reading rooms. We had a rotating group of 7-8 family medicine residents, who are expected to read their own imaging examination when they become attending physicians. They were highly interested in everything that we taught. Our curriculum included a background review of anatomic findings on X-ray, CT, and ultrasound. Following anatomic review, we then explored pathological findings on these modalities. We also provided the residents with reading material, including electronic textbooks for them to review. Overall, I was very pleased with their progress during the month that we spent in Kijabe. The family medicine residents were able to progress to the knowledge level of a junior US radiology resident, which was very rapid indeed!
We gave a series of lectures to the rotating interns of the entire hospital. These lectures were meant to introduce basic anatomy concepts as well as often seen findings of pathology in imaging examinations. We based our lectures on the needs of the interns, who specifically request pediatric lectures, musculoskeletal lectures, and chest radiograph lectures. I introduced the Socratic Method to our lectures, requesting individual interns to answer in a hot seat scenario and make the diagnosis. Overall, this had a great impact boosting the confidence of the interns, as most of them gave the correct answers to nearly all of my questions!
One of the most poignant areas was fluoroscopy. Typically at Kijabe, no radiologist is available to perform fluoroscopic procedures. During my time there, I performed several complex fluoroscopic procedures, including one on a patient who suffered a gunshot wound. I performed fluoroscopic examinations of the urethra, bladder, and rectum. Eventually, I had found the fistula from the bladder to the skin responsible for the patient’s frequent symptoms of infection and sepsis.
Fluoroscopy was only the tip of the iceberg for complex pathology. Every day we dealt with trauma, complex infection, advanced tuberculosis, end-stage AIDS, and other pathologies not typically seen in the US. While hectic, the best part was delivering the appropriate diagnoses to the clinicians and directing them towards the right path of treatment.
My entire team (my co-residents) and I deeply appreciate the help that the Doximity Foundation provided for our mission trip.
My name is Pengcheng Zhang. I am currently a fourth year radiology resident (post-graduate year 5) at Wake Forest Baptist Medical Center. This mission trip was a first for me. I plan to use my experiences going forward as an abdominal radiology fellow at UCSF and as a practicing radiologist.