As minimally invasive techniques and point of care ultrasound (POCUS) continue to advance operative course and procedural techniques for patients around the world, training paradigms internationally have not allowed for this advancement unilaterally. Image guided procedures, reduce morbidity and mortality. However, many low and middle income countries have limited or complete lack of Radiology or Interventional Radiology services.
In 2017 there was no single interventional radiologist in Tanzania. Meaning a population equivalent to that of California and New York combined was without access to a broad range of treatments. In the past 5 years, the Tanzania IR Initiative has championed this lack of access by establishing East Africa’s first IR training program, training the first generation of interventional radiologists in the country. Now, as the initial trainees reach attendinghood, and new graduates enter the program – we must begin to expand the population which can be served by these procedures.
Pediatric Interventional Radiology serves a unique role around the world, at the intersection of Pediatric Surgery and Interventional Radiology, the specialty offers minimally invasive solutions to the wide pathologies of children. Whether this entails abscess drainages from acute appendicitis or sclerotherapy of a vascular anomaly from genetic disposition, comfort and confidence in treating kids by IR is required. Providing the training program with a Pediatric IR intensive focused on vascular anomalies as well as general maladies, we will advance IR in Tanzania to offer comprehensive pediatric care.
Tanzania is a country in need of Pediatric IR, while it has approximately 60 million people in the population, the median age is 18, and 44% of the population is under 14. Additionally, certain pathologies such as vascular anomalies which can be functionally restrictive, and cosmetically disfiguring often are best served by endovascular treatment during childhood. By training the trainees, and expanding comfort and knowledge with these patient populations and pathologies, we can change the course of children in Dar es Salaam and beyond, through trainees who will return to their home countries (Rwanda, Nigeria, etc.) after training.
In offering the advances pediatric IR provides in high income countries to East Africa, the impact will be many-fold. Countries like Tanzania, with young populations, have large gaps in the pediatric care offered, and it behooves trainees in minimally invasive procedures to become comfortable in pediatrics. I want to support and expand these efforts, starting with the untapped potential of radiology trainees in Tanzania; the benefits of providing Pediatric IR training in Tanzania is a small first step to comprehensive pediatric care.
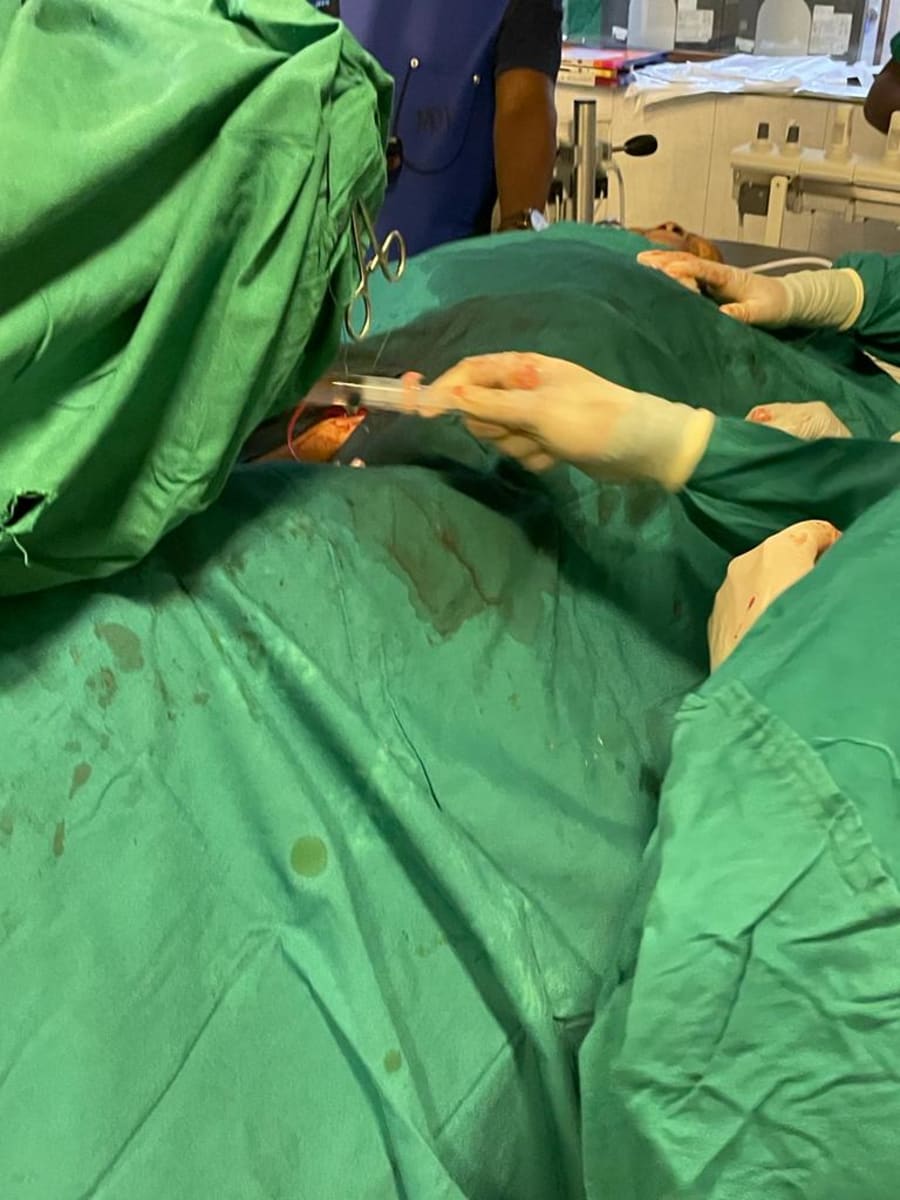






In conjunction with the Vascular Anomalies camp run by OMFS and IR at Muhimbili National Hospital in Dar es Salaam, we were able to use invitation to enhance the local expertise with further training and techniques. This camp is essentially the only option for vascular anomalies in pediatric patients for the country, as such there are high volumes of patients to be seen and immense pathology. During my stay we were able to safely accomplish the first retroorbital sclerotherapy in Tanzania (per reports) as well as more than 30 sclerotherapies. This work would have been impossible without the Doximity grant and Road2IR, I will be honored to return next year and continue this life changing work.