To improve the delivery of respiratory care at Adama Hospital Medical College (AHMC) in Adama, Ethiopia, by training ICU nurses in Mechanical ventilation management.
Aim 1: Conduct a mixed-methods assessment of current respiratory care practices and needs at AHMC with a quantitative and qualitative evaluation of leadership and staff barriers and facilitators to improving respiratory care
Aim 2: Develop a locally appropriate curriculum for increasing ICU nurse competency in RT skills using an existing RT education module on mechanical ventilation
Aim 3: Pilot and evaluate a respiratory care training curriculum
Aim 4: Conduct needs assessment for tele-ICU intending to provide and train highly skilled health care providers to manage critically ill patients using ongoing training programs in respiratory care for a future project
AHMC is currently one of the UMN partner global health sites led by on of the study co-investigator, and this project will help strengthen our existing partnership and commitment.
I am the main program director in this project and during my stay in Ethiopia, I will be involved in the data collection for the needs assessment portion as well as implement to course online and hands on portion in two different travel times.
We hypothesize that implementing a short respiratory care training focused on mechanical ventilation (MV) for ICU nurses will improve nursing knowledge in the operation and management of MV, increase confidence in the performance of these activities, and decrease MV-related complications to an intubated patient at AHMC.
This project will allow us to expand our project to more ICU nurses and potentially lead to the development of an RT program and ultimately build capacity in respiratory care in Ethiopia and sub-Saharan Africa and improve patient outcomes.
Several factors have been attributed as drivers of respiratory disease in Africa, including the lack of healthcare workers trained in managing respiratory diseases. According to the WHO (2016), about 20-40% of the wastage in the international health system is due to workforce inefficiency and weaknesses in health workforce power. Studies have shown that RT care yielded a cost reduction and reduced the growing health disparity between the richest and poorest globally. A survey of hospitals in Nigeria estimated the proportion of registered respiratory physicians to the national population as 1 per 2.3 million individuals. Educational programs may help build capacity in respiratory care in low to middle-income countries.
Ethiopia has few non-physician clinicians (e.g., nurses) with respiratory therapy skills and only one respiratory therapy training program. This lack of respiratory-trained personnel increases health disparity1,3, adds to the work burden on physicians and nurses1, and increases healthcare costs.5
Approximately 80% of Adama Hospital Medical College (AHMC) ICU patients in Adama, Ethiopia, require mechanical ventilation. However, there is a gap in respiratory therapy skills due to a lack of respiratory therapists. Physicians who perform most mechanical ventilation management at AHMC have varied training (e.g., anesthesiology, general practitioners, or emergency medicine doctors) without subspecialized training in pulmonary or critical care. Nurses perform other respiratory care (e.g., administering nebulizers, suctioning, physiotherapy) but are not trained in mechanical ventilation management. Adding RT duties to nurses and physicians without proper training is more likely to lead to healthcare disparity, increase staff burnout, further healthcare worker shortage, and increase healthcare costs.
This work will improve health equity by increasing access to quality respiratory care for mechanically ventilated patients in the AHMC ICU. It will help maintain the workforce by enhancing satisfaction among providers and, if implemented broadly, has the potential to lower the cost of respiratory-related diseases. This project will inform a large-scale program of implementing an RT curriculum in small increments, starting with mechanical ventilator training for ICU nurses, then developing respiratory care training for nurses across the hospital to develop a respiratory therapy program in Adama. Larger-scale studies will allow evaluation of the cost benefits and effects on key outcomes (ICU length of stay, ventilator days) to assess care quality. This project will further collaboration between the UMN and AHMC collaborative. Lastly, we hope this project can be used as a model to improve respiratory therapy education internationally in low- and middle-income countries.
Our innovative project will bring international standard respiratory care education and care to staff and ICU patients at AHMC. Through this program, Ethiopian healthcare workers will gain improved respiratory therapy skills. By supporting an education program developed with a partnership between Ethiopian and U.S. experts, our goal is to help build capacity in respiratory care and bring about sustainable change to the daily standard of care for the patients at AHMC.

















I was in Adama before, once to start the collaborative work between Adama Hospital Medical Center (AHMC) and the University of Minnesota on my current project. This time, I was here to begin working on the project born at that first visit, which aims to develop and implement training ICU nurses on mechanical ventilation and beyond.
As I arrived in Adama, Ethiopia, the vibrant colors and bustling streets welcomed me to the city and the coffee I couldn’t stop talking about . Despite being born and raised in Ethiopia, this was my first real exploration of the city, and I was eager to see what it offers.
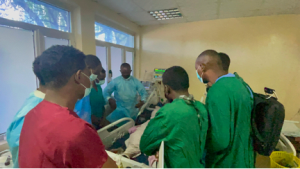
On the first day at AHMC central ICU, I had the privilege to round with Dr. Dawi, an anesthesiology-trained ICU physician I highly respect, and residents. The morning went smoothly until Dr. Dawi received an urgent call about a 10-month-old child arrested. Without hesitation, the team rushed to the scene.
As we arrived, I witnessed the incredible collaboration of healthcare teams. Despite the limited resource, the healthcare professionals worked tirelessly to resuscitate the child not once but twice. I saw the dedication and passion in the eyes of everyone involved. Sadly, the child’s condition was critical, and his chances of survival were slim without immediate surgical intervention. This sobering reality hit hard, and I couldn’t help but wonder how different the outcome would be if the necessary resources were available.
As the day continued, I observed the daily routines of the hospital, the long lines of patients waiting for treatment, and the overworked healthcare staff doing their best to help everyone in need. I couldn’t help but admire the resilience of the doctors and nurses in the low-resource setting and their unwavering dedication to their community.
Every morning I make my way to the hospital on a Bajaj, a three-wheel motorcycle that is a popular mode of transportation in Adama.
The team and I from the University of Minnesota and other volunteers have partnered with AHMC to create and implement mechanical ventilatory training courses for ICU nurses. If I am not rounding in the ICU, I spend most of my time distributing surveys and hearing about healthcare workers' experience in caring for patients with respiratory illnesses. I was grateful to have the ICU head nurse, Sultan, accompany me to every hospital floor to help distribute and collect the surveys. Sultan was incredibly knowledgeable and collaborated with me to give a detailed explanation of on goal of our project. I was pleasantly surprised at how willing everyone was to fill out the survey, and we had almost all of them returned by the end of each day.
As I went around nearly every hospital department, I was struck by how large the facility was. I had the opportunity to interview a NICU nurse who was genuinely excited about the upcoming training on mechanical ventilation. She took me on a tour of the NICU and showed me a bubble CPAP machine made from a used water bottle.
The depth to which the tubing was immersed underwater determined the pressure generated in the infant’s airways. The nurse also explained Downe’s score system to me, which guides how they administer oxygen supplement devices to infants. If a score of 8 or higher is reached, it is an indication of intubation, which is not currently an option at the hospital. There are two functional and one non-functional mechanical ventilator in the NICU, but the ability to use those machines effectively is limited without a neonatologist on-site.
As I spent more time there, I noticed the staff's challenges, especially with mechanical ventilation. One of the most glaring issues was the need for well-trained nurses to manage the ventilators. Without respiratory therapies to assist, it was almost impossible to implement mechanical ventilation in infants successfully. Moreover, I realized a significant need for proper infrastructure to deliver this care effectively.
But that wasn’t the only problem. In the central ICU, The ABG (arterial blood gas) machine, essential in determining the proper ventilator settings, had malfunctioned for years. This posed a significant challenge, especially when making critical decisions regarding patients who required ventilator settings changes or intubation/extubation decisions. Despite this, I was amazed at the skill and expertise the healthcare providers had developed, even without such a critical diagnostic tool. They had to rely on clinical and objective data to make informed decisions.
There were still limitations to the alternatives available. For instance, VBG (venous blood gas) was available, but the cost to the patient was a significant challenge, limiting the amount of work-up a patient could receive. Additionally, most ventilators' ETCO2 (end-tidal carbon dioxide) monitors were not functional.
I saw firsthand the challenges healthcare providers face when making critical decisions without the proper diagnostic tools. One night, I was in the ICU with one of the ICU physicians, Dr. Dejene, when we faced a challenging situation. Even after trying to tackle it with a long-distance call with a USA-trained respiratory therapist, who happened to be my husband, we were forced to adjust our clinical approach when deciding which mode to place a 10-year-old child is due to a lack of a functioning ABG machine and ETCO2 monitor.
Challenges faced by developing countries such as Ethiopia, where respiratory care training is not readily available, with currently only one location in the city that offers a master’s program in respiratory therapy training, highlight the scarcity of this type of training in the country.
However, there is a glimmer of hope on the horizon. Volunteers like my husband, who works at children’s hospitals in Minnesota, and Respiratory therapy instructors from the University of Minnesota/Mayo clinic are due to arrive in the upcoming months as part of our project to improve respiratory care in Ethiopia. As part of this project, a well-thought-out online course on the management of mechanical ventilation is near completion, followed by hands-on training for ICU nurses and other healthcare providers at AHMC. This training will help advance the knowledge and skills of providers currently managing mechanical ventilators.
To conclude my trip this time, I was fortunate to have the opportunity to lecture on various types of Shock to a predominantly medicine resident audience. As someone who has traveled to Uganda and Ethiopia during my global health international rotation, I witnessed learners' eagerness and thirst for knowledge in these regions. Physical presence may only sometimes be feasible in the future, especially when collaborating across borders and continues. Therefore, I aspire to create a virtual platform that will bring together medical students and residents from East African countries, with experts from the US sharing their knowledge and expertise.
As I departed from AHMC, I had a newfound appreciation for the healthcare providers working in challenging conditions. I understood the burden that AHMC faces with the patient load, the impact of resource scarcity on patient outcomes, and the significance of training healthcare workers to improve patient outcomes. Witnessing the healthcare professionals’ dedication and resourcefulness in providing care with limited resources was inspiring.
Our training project represents a significant step towards enhancing the overall quality of healthcare in Adama and the country as a whole. However, I realized it was just a small part of the solution. The healthcare system in Ethiopia requires more support and resources to provide better care for its citizens.
My experience at AHMC left an enduring impression on me. It has motivated me to continue working towards a world where everyone can access quality healthcare regardless of background or location. I am committed to contributing my skills and expertise to support the improvement of healthcare systems in under-resourced communities like Adama, Ethiopia.
I am so grateful for the support Doximity foundation gave me by funding my flight expense. Thank you!